-
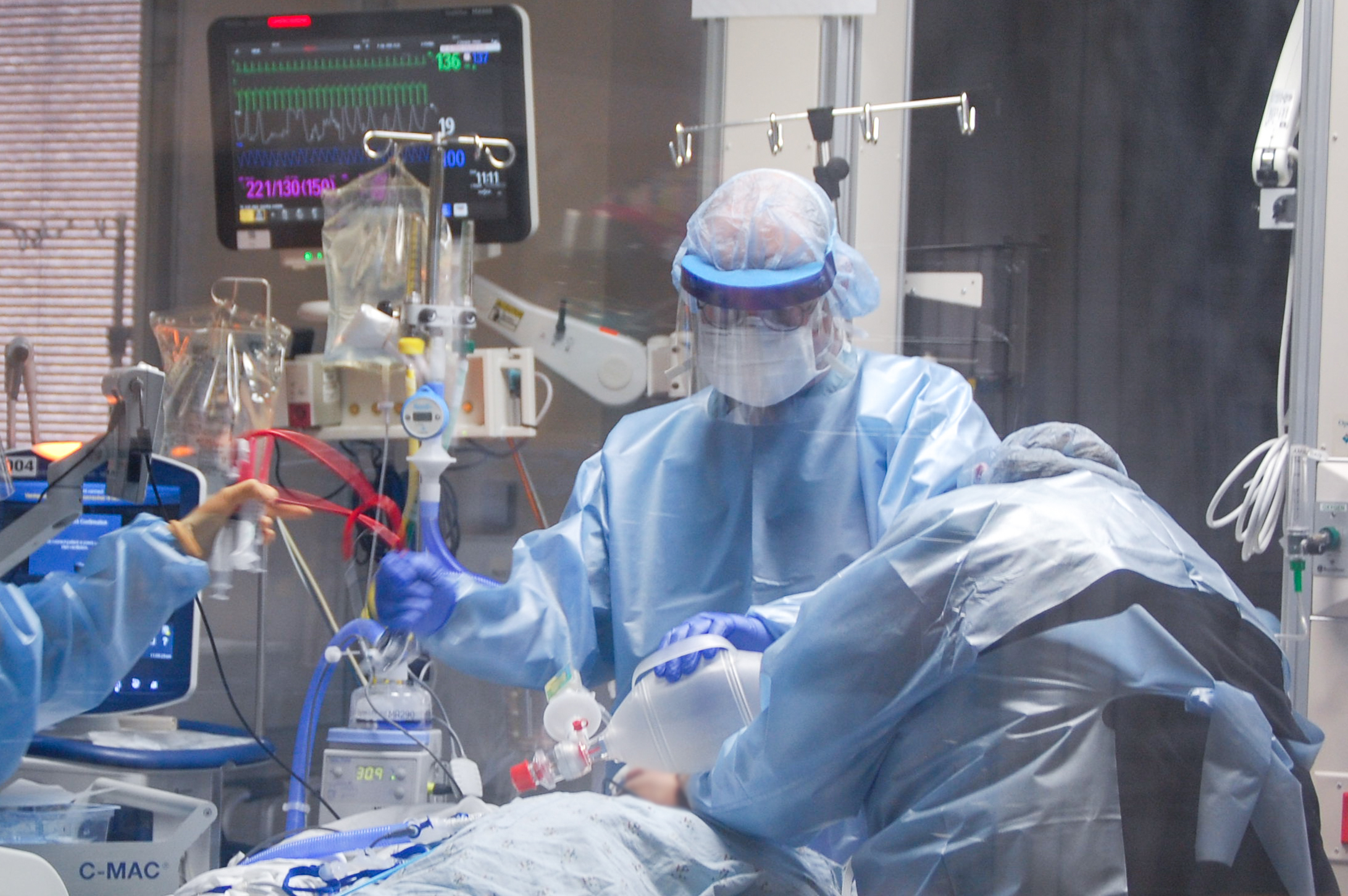
University Hospital - Medical ICU
Our critical care services continue to grow, as we are striving to meet the needs for more intensivists. As a result, we have transitioned to four medical intensive care unit teams. Two teams are comprised of interns/residents, a fellow, and an attending. The other 2 teams are non-teaching service comprised of an attending and Nurse Practitioners. The fellows rotating in the ICU will admit to their respective services during the day and will rotate transfer and admission responsibilities week to week. The fellow will be very familiar with patients and concentrate on new admissions each morning. The fellow will have the opportunity to become very comfortable with airway management, bronchoscopies, POC Ultrasound, mechanical ventilator management, and percutaneous tracheostomy. They will also closely supervise any procedures performed by the house staff (central venous catheters, thoracentesis, paracentesis, etc.). Education has a very important role in the ICU. To this end, the fellow will have an important role in teaching on relevant ICU topics.
-
University Hospital-Consultation Services
Fellows assigned to the University Hospital Consultation Services will be responsible for consultations received by the Pulmonary Division from the UAB Hospital. This includes both Pulmonary and Critical Care consultation. The fellow on UH Consults is in charge of leading the team, managing patient care, performing bronchoscopies, and supervising the residents during procedures. While patient care is the foremost responsibility of this service, diplomacy and interdisciplinary relationships are important part of professional development as you learn to become an effective consultant.
-
Special Care Unit and Inpatient Pulmonary Service
The Special Care Unit is an intermediate care unit for chronic ventilator weaning. Patients in this unit come from all the ICUs in the hospital for aggressive rehabilitative services and ventilator weaning. We have a dedicated Inpatient Pulmonary Service for chronic ventilator patients and advanced lung disease patients. This floor also has our adult Cystic Fibrosis Patients and Interstitial Lung Disease Patients. The patients in both units have a small group of hospitalists as their primary providers, while an attending and fellow from PCCM work closely with them to co-manage the respiratory issues. This rotation allows for 1:1 interaction between the PCCM attending and fellow to optimize education in the specialized care of pulmonary inpatients.
-
Medical Emergency Team
This is the Rapid Response Team for University Hospital. On this service you and an attending will respond to acute deteriorating patients and all patients with sepsis. You will assist with acute management, triage patients to appropriate care settings, and become comfortable with acute airway management. This rotation provides an excellent opportunity to better understand how the patient safety systems in the hospital operate.
-
Interventional Pulmonology
We have 3 Interventional Pulmonologists on faculty and 1 Interventional Pulmonary Fellow every year. You will round with this team and learn how to navigate airways in the OR during your first year. You will learn the appropriate work up for lung masses and when advanced endoscopic procedures are required. During the second and third years, fellows will participate and become certified in Endobronchial Ultrasound (EBUS), as well as participate in other advanced bronchoscopic procedures. On this rotation you will also learn how to do pleural procedures such as thoracoscopy and intrapleural catheters.
-
Lung Transplantation and Advanced Lung Disease Service
The goals of this rotation are to provide a comprehensive clinical experience in the management of pre- and post-lung transplant and ECMO patients. Fellows will have the opportunity of working in a non-medical ICU environment with a multidisciplinary team to 1) increase knowledge on the guidelines for referral and the appropriate timing for lung transplantation, 2) to increase knowledge on the chronic management of immune suppression in the outpatient setting, and 3) to enhance skills on bronchoscopy and associated techniques/procedures in the lung transplant setting. Fellows will be exposed to all aspects of lung transplantation medicine and management of patients with hypoxemic respiratory failure on ECMO. Fellows in this rotation attend pre-and-post-transplant clinics as well as rounds in the intensive care units that handle these patient populations.
-
Night Float
We have a Night Float team system for nocturnal care of our ICU patients instead of a call-system. First years will have 5-6 weeks of Night Float, second years 3-4 weeks, and third years 1-2 weeks. There is at least one attending, a fellow and 2 residents in house at night. This team does nighttime ICU rounds and new ICU admissions. The Night Float fellow is also responsible for going to BVAMC each night to assist with emergencies and make morning weaning plans for all ventilated patients.
-
BVAMC Medical ICU
All patients hospitalized in the 10-bed VA MICU are admitted to a dedicated MICU team consisting of 5 residents, a Pulmonary/CCM fellow, and one faculty physician. VA MICU Fellow Responsibilities consist of Monday-Friday rounds with the team, supervising performance of all major procedures (e.g. bedside bronchoscopies, thoracentesis, etc.), and assisting the attending in carrying out teaching and rounding responsibilities.
-
BVAMC Consult Service
The VA Consult Fellow will be responsible for consultations received by the Pulmonary Division from the VA Hospital. This fellow will see all consults, staff them with the VA attending and perform any procedures including bronchoscopy as needed. The VA Consult Fellow is also responsible for any outpatient bronchoscopies and will collaborate with the Section’s Nurse Practitioner and the Lung Mass Fellow. This fellow also gets exposure to outpatient subspecialty pulmonary medicine by attending weekly Asthma and Interstitial Lung Disease clinics.
-
BVAMC Lung Mass Rotation
This rotation is for senior fellows only. Fellows will be exposed to patients being evaluated for thoracic malignancies. Fellows will work closely with our interdisciplinary lung cancer team attending clinic, tumor board, and performing advanced endoscopies including EBUS. This team includes faculty from the Pulmonary, Thoracic Surgery and Clinical Oncology. This fellow will attend outpatient Lung Mass and COPD clinics.
-
Continuity Clinic
Every fellow will attend Continuity Clinic weekly, either at The Kirklin Clinic or BVAMC on a rotating basis. At The Kirklin Clinic, the fellows have their own panel of patients for whom they are the primary pulmonologist. At the BVAMC, the fellows will share panels of patients and operate in a more group practice system. Fellows are responsible for the diagnosis and management of the full breadth of outpatient pulmonary medicine and for managing their patients in between appointments. Continuity clinics span throughout all 3 years of the fellowship.
-
Electives
Fellows have opportunities to do electives in the following areas: Echocardiograms, Cardiac Care Unit, ECMO, Thoracic Radiology, Ambulatory Clinics, POC Ultrasound, Pulmonary Hypertension, Interstitial Lung Disease, Cystic Fibrosis, Neuro-ICU, Surgical ICU, Trauma ICU, Lung Transplant, Interventional Pulmonary, Pulmonary Hypertension