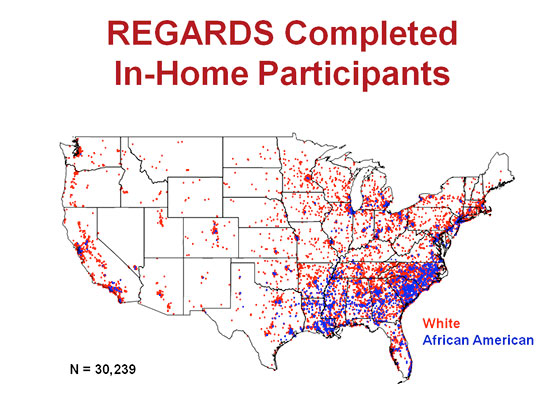
 More than 30,000 people from across the country have participated in the REGARDS study. The blue dots represent the locations where African-Americans participating in the study live and the red dots represent where white participants live.A long-running national study that examines why more African-Americans die from strokes than other races, and why people in the Southeast develop more strokes than those in other areas of the nation, will be funded for another five years thanks to a multimillion-dollar grant.
More than 30,000 people from across the country have participated in the REGARDS study. The blue dots represent the locations where African-Americans participating in the study live and the red dots represent where white participants live.A long-running national study that examines why more African-Americans die from strokes than other races, and why people in the Southeast develop more strokes than those in other areas of the nation, will be funded for another five years thanks to a multimillion-dollar grant.
The REGARDS (REasons for Geographic and Racial Differences in Stroke) study will be funded through 2023 by a $20.4 million grant from the National Institutes of Health’s National Institute of Neurological Disorders and Stroke (NINDS). It has received nearly $100 million in grant funding since it began in 2003.
The study, based at the University of Alabama at Birmingham School of Public Health, is run by a team of biostatisticians, epidemiologists, hematologists, psychologists, neuropsychologists and neurologists. The team includes collaborators from the University of Vermont, University of Cincinnati, Indiana University, Drexel University and Columbia University.
The goal of the study is to better understand racial and regional differences in deaths from strokes in the United States. More than 30,000 people have participated in the study since it began. Researchers initially assessed stroke risks in 30,329 black and white people ages 45 and older between 2003 and 2007. They recently finished visiting more than half of the patients for second in-person assessments and follow-up exams. Some of the study participants have been in the study for 14 years.
Lead study principal investigator George Howard, DrPH, UAB professor of biostatistics in the School of Public Health, says the study participants are the heroes of this work.
“Because of the contributions of the study participants, a lot has been learned,” Howard said. “Because of them, I honestly think the burden of stroke can be reduced for everyone, but particularly for African-Americans and Southerners. If we do this, the implications are staggering.”
 George Howard, DrPHWhile the participants will continue to be followed to study stroke risk, factors associated with healthy cognitive aging will also be studied in the next five years of the project. That portion of the research is being led by Jennifer Manly, Ph.D., an associate professor of neuropsychology at Columbia University.
George Howard, DrPHWhile the participants will continue to be followed to study stroke risk, factors associated with healthy cognitive aging will also be studied in the next five years of the project. That portion of the research is being led by Jennifer Manly, Ph.D., an associate professor of neuropsychology at Columbia University.
“This study will increase understanding of what causes racial and regional differences in brain health so that we can all maintain memory and other thinking abilities as we age,” Manly said.
When the study began, stroke was the third leading cause of death in the United States. Today, it is the fifth. Howard says it is good that the stroke mortality rate is decreasing, but it is not falling fast enough for everyone.
“Stroke mortality is going down in white people, and it’s going down in African-Americans,” Howard said, “but it’s going down faster in white people than in African-Americans, so the racial disparity is getting larger. The bad news is that, if you look at the stroke mortality rate by age, between the ages of 45-65, it is 200-300 percent higher for African-Americans.”
Howard says 11 percent of deaths from strokes in white people happen before age 65, while that number rises to 28 percent in African-Americans.
The study has provided critical data about differences in stroke incidence and mortality throughout the United States. In 2013, experts found that living in Stroke Belt states — Alabama, Arkansas, Georgia, Louisiana, Mississippi, North Carolina, South Carolina and Tennessee — early in life, increases the risk of stroke.
“Living in the Stroke Belt at any age tended to increase stroke risk,” said Virginia Howard, Ph.D., the study’s lead epidemiologist and UAB professor of epidemiology. “But living in the Stroke Belt as a teenager or young adult appears to impart even greater stroke risk than living there as an adult.”
The type of neighborhood where one lives is also a variable. Researchers using REGARDS data found that the lower a neighborhood’s socioeconomic status, the higher a person’s stroke risk. The risk was the same whether the participants were white or black. With more research, Howard hopes they will be able to identify specific risk factors that are tied to neighborhoods, and discover what changes can lessen those risks.
 Virginia Howard, Ph.D.While the REGARDS study started with a focus on stroke, the data has been used by scientists from UAB and institutions around the nation in more than 100 ancillary studies, leading to hundreds of scientific discoveries.
Virginia Howard, Ph.D.While the REGARDS study started with a focus on stroke, the data has been used by scientists from UAB and institutions around the nation in more than 100 ancillary studies, leading to hundreds of scientific discoveries.
In 2012, UAB researchers found that black men and women still have twice the risk of fatal coronary heart disease compared with white men and women. The data was also used in a study that found that eating a Mediterranean diet may be linked to preserving memory and thinking abilities.
Howard believes the discoveries that can come out of the REGARDS study are endless.
“Working with other scientists from across the nation, we’ve added new outcomes: heart disease, fractures, sepsis, end-stage renal disease,” Howard said. “These have been added since the study began. Thanks to this new grant, even more studies will come out of it.”
When the NIH gave Howard and his team the first grant of $28 million to fund the project, it was the largest grant ever awarded to UAB for a single, five-year study.
When asked what the overall goal of the study is, Howard says it is to reduce racial and geographical disparities in stroke. But he is not ready to stop there.
“My life’s goal would be to understand why African-Americans have more hypertension than white people,” he said. “I think if we could understand that, we could design better health care strategies to prevent it or manage it better.”
