For almost a year, Mary Chris Ponder searched for someone to fill a nurse practitioner vacancy for clinics affiliated with Citizens Baptist Medical Center in Talladega, Alabama, and in the nearby community of Munford.
As director of operations for the Baptist Health Centers in the Citizens Hospital market, Ponder was accustomed to the challenge of hiring health care professionals – particularly physicians and nurse practitioners – for smaller urban and rural areas. But this one had proven bigger even than the big-time NASCAR stock car racing with which Talladega, located some 70 miles east of Birmingham, is synonymous.
You can imagine Ponder’s delight then when she got word from Skye Vise, MSN, CRNP, a 2015 graduate of the University of Alabama at Birmingham (UAB) School of Nursing with a Master of Science in Nursing degree, she would accept the job.
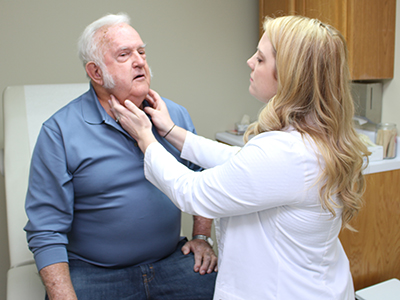 Skye Vise examines a patient who has come to the Citizens Baptist Medical Center-affiliated clinic in the small community of Munford, Alabama, for care.
Skye Vise examines a patient who has come to the Citizens Baptist Medical Center-affiliated clinic in the small community of Munford, Alabama, for care. “I may have done a little dance at my desk,” Ponder admitted with a laugh.
Ponder’s plight is one shared by many in her capacity throughout Alabama. How do you attract qualified, skilled health care professionals to areas like Talladega with its population of 15,846 and Munford, 10 miles up the road and 10 times smaller, when there are many more attractive options elsewhere?
In Ponder’s case, she turned to the School and its Graduate Nursing Education Primary Care Scholars (GNEPCS) program.
Put in place in early 2014, GNEPCS identifies and nurtures current nurse practitioner students with an expressed interest in providing primary care in one of Alabama’s rural-designated counties upon graduation. Vise, from nearby Lincoln, was one of those Primary Care Scholars.
“When I first applied for the nurse practitioner program at UAB, they required an entrance essay, and I actually wrote about my career goal -- to work in a community like my own,” Vise said. “Ideally Lincoln was what I was thinking of then, but Munford is right next door, and my husband, Jarrod, is from here. It’s the same concept now, but with me helping the community where he was raised.”
After graduation in August 2015, Vise went to work in November and quickly became a vital member of the care team in the clinics and the communities she serves, Ponder said.
“Skye was greatly needed, and she has certainly settled in nicely in a very short period of time,” Ponder said. “I’m also sure she’s learning more firsthand as an independent provider in these practices than she might have in certain other situations.
“I have to think she is seeing more and varied patient problems and diagnoses in this role and having a lot more ability to treat patients than somebody who may be doing the same thing every day in a more urban setting.”
It truly has been on-the-job training for Vise in many ways. One typical aspect has been the learning curve any recent graduate experiences in their first months on a new job. Another issue her colleagues who practice in a more urban setting may not face has been the adjustment to the realities of providing health care in a rural setting.
For instance, what does she do when an X-ray is needed? When she worked for a pulmonary practice in Birmingham in a big office building the patients were just told to go up to the second floor for their X-ray. Now if a patient in the Munford clinic needs one, it requires a trip to another city.
 Vise is proud to be providing health care services in the small town where her husband grew up and in nearby Talladega, Alabama.“They have to go 10 miles south to Talladega or 10 miles north to Anniston, and sometimes they have to find somebody to take them and sometimes that person can’t go that day,” Vise said. “It’s a lot about using your judgment as to what’s going to work best for the patient under the circumstances.”
Vise is proud to be providing health care services in the small town where her husband grew up and in nearby Talladega, Alabama.“They have to go 10 miles south to Talladega or 10 miles north to Anniston, and sometimes they have to find somebody to take them and sometimes that person can’t go that day,” Vise said. “It’s a lot about using your judgment as to what’s going to work best for the patient under the circumstances.”She has made other adjustments in her approach as well, particularly when treating low-income patients. It doesn’t help to order a preventative screening or write a prescription if they are cost prohibitive so she has quickly learned to take advantage of various low-cost pharmacy options and free screening opportunities.
“Low-income patients can’t afford a lot of expensive medicines,” Vise said. “So using the low-cost pharmacy options some retailers offer would be our first approach in treating conditions such as high blood pressure or diabetes. The same for preventative screenings. While it is very important to have them, patients are less likely to get them if they are very expensive, so you have to be aware while trying to help them.”
After just a short time on the job, Vise is fully convinced she made the best choice by coming to the School and choosing the Primary Care Scholars program.
“I think the Primary Care Scholars program is a great opportunity,” Vise said. “We’re all given general knowledge through the MSN program but to have such a specialized skill set directed toward your career objective is highly beneficial. I think it has already helped me tremendously as a nurse practitioner.”
Ponder is certainly pleased with her decision to offer the job to Vise, with Vise’s decision to accept the challenge, and with the impact she has made in a very short period of time on two communities that needed her talents and expertise. Ponder also said that should she have another vacancy in the future she will definitely look again to the School and Primary Care Scholars Program for help.
“Skye has truly been a blessing,” Ponder said. “We couldn’t have hit more of a home run than hiring Skye, and I hope she feels the same way. If there is a pipeline of talented people like Skye coming from the UAB School of Nursing on a regular basis who meet our needs, you can be sure we will continue to come back again and again to fill those needs.”
