Need more information? Contact us
End stage kidney disease affects more than 600,000 people in the United States. A team of physicians and researchers from the University of Alabama at Birmingham and spinoff startup company Endomimetics is looking to improve the care for these patients with a grant from the National Institutes of Health.
More than 80 percent of the affected patients use hemodialysis as their renal replacement modality of choice. The Achilles’ heel in the care of dialysis patients is the development of a functioning and durable vascular access, preferably an arteriovenous fistula.
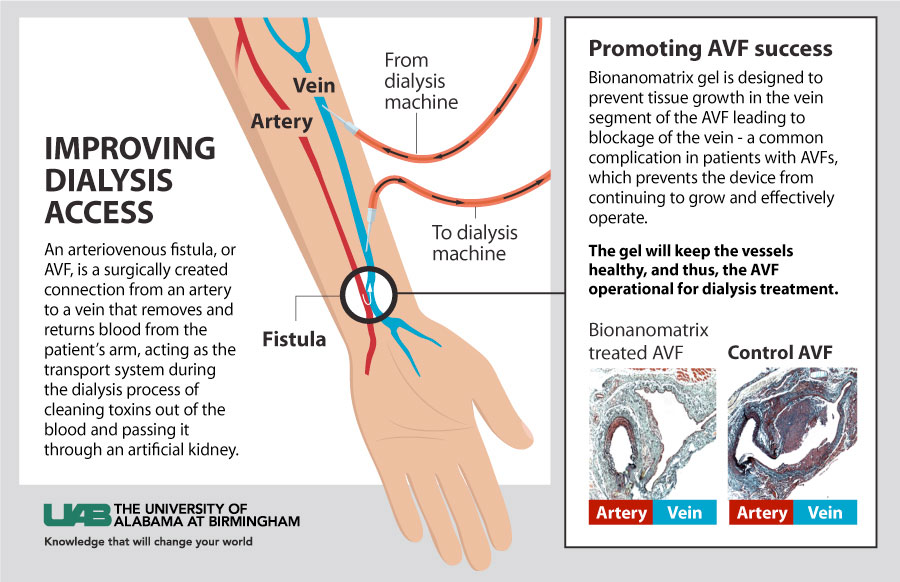
 (Standing) Brigitta Brott, M.D., Joseph Garner, Ph.D., Ho-Wook Jun, Ph.D., (seated) Timmy Lee, M.D., and Patrick Hwang, Ph.D.An arteriovenous fistula, or AVF, is a surgically created connection from an artery to a vein that removes and returns blood from the patient’s arm, acting as the transport system during the dialysis process of cleaning toxins out of the blood and passing it through an artificial kidney. “When you need dialysis, you have to have a needle put in three times a week to get the fluid exchanged,” said Brigitta Brott, M.D., UAB cardiologist and professor of medicine, and co-founder of Endomimetics. “The best way to do that is to have a direct connection between the artery and vein.”
(Standing) Brigitta Brott, M.D., Joseph Garner, Ph.D., Ho-Wook Jun, Ph.D., (seated) Timmy Lee, M.D., and Patrick Hwang, Ph.D.An arteriovenous fistula, or AVF, is a surgically created connection from an artery to a vein that removes and returns blood from the patient’s arm, acting as the transport system during the dialysis process of cleaning toxins out of the blood and passing it through an artificial kidney. “When you need dialysis, you have to have a needle put in three times a week to get the fluid exchanged,” said Brigitta Brott, M.D., UAB cardiologist and professor of medicine, and co-founder of Endomimetics. “The best way to do that is to have a direct connection between the artery and vein.”
“AVFs are the current gold standard of care for patients of dialysis,” said Timmy Lee, M.D., professor in UAB’s Division of Nephrology. “Unfortunately, that gold standard of care is not perfect — most AVFs never develop successfully to be used for dialysis treatment.”
Patients who have AVFs that fail are faced with months of time before they are able to receive another AVF, which means they must receive dialysis with a catheter, which carries a host of its own issues.
The annual cost of treating vascular access dysfunction totals more than $1 billion. This is largely due to the high proportion of arteriovenous fistulas that fail to mature.
After creation, 60 percent of AVFs fail to mature successfully for dialysis use, due to early venous neointimal development and inadequate vasodilation. At present, there are no effective therapies to promote vascular access maturation.
The team’s solution is a bionanomatrix gel that will promote AVF maturation.
The UAB-developed substance mimics the tissue lining our blood vessels — endothelium. Previous studies on the material showed that it could prevent the narrowing of the artery known as stenosis, allowing maturation of the AVF to continue.
“Our tests in the lab showed that this new coating promotes AVF maturation, and may have significant impact in the treatment of patients requiring dialysis,” said Ho-Wook Jun, Ph.D., biomedical engineering professor and co-founder of Endomimetics.
| “Our tests in the lab showed that this new coating promotes AVF maturation, and may have significant impact in the treatment of patients requiring dialysis.” |
“We believe the use of the bionanomatrix gel can substantially increase the success rate of AVF formation, addressing this unmet clinical need,” said Patrick Hwang, Ph.D., director of research and development for Endomimetics. “This would result in a significant decrease in the cost of creating AVFs as well as improving the overall life of the patient.”
“Obviously, we are very excited about receiving the grant, which will allow for the continued development of the bionanomatrix gel and its use in the creation of an access point, or AVF, to veins for patients requiring dialysis,” said Joseph Garner, Ph.D., CEO of Endomimetics and Assistant Professor in the School of Health Professions. “It is our belief, which is being supported by our data, that the bionanomatrix gel has the potential to greatly increase the rate at which the AVFs are successfully created, which will dramatically reduce the cost and physical pain endured by the patient.”
The Small Business Innovation grant totals $2 million and will support the development through further testing of the product. The grant is in phase two, which means the team will be able to continue the research and development efforts initiated when they were awarded a phase one grant last year. This phase will last two years, with the goal of being awarded a phase three grant to pursue commercialization.
“UAB has provided a unique environment in which engineers and clinicians can work together to develop an innovative idea to tackle clinically significant problems,” Jun said. “We have had so much support from the School of Engineering, School of Medicine, and the Bill L. Harbert Institute for Innovation and Entrepreneurship here at UAB, and we are looking forward to developing this solution further.”
