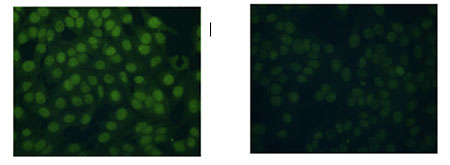
 Circulating autoantibodies against epithelial cells are detected by green fluorescence in patients with acute exacerbation of idiopathic pulmonary fibrosis. The intensity of the fluorescence is proportional to the autoantibody concentration. All IPF patients with acute exacerbations had abnormal increases in autoantibody concentrations pre-treatment (left image). The right image shows the reduction of fluorescence which was typical among patients who responded to treatment.Patients with acute exacerbations of idiopathic pulmonary fibrosis responded well to therapies similar to those used to treat autoimmune diseases, according to findings published today in PLOS ONE. The study suggests that autoantibodies — implicated in many autoimmune diseases such as rheumatoid arthritis or lupus — also play an important role in patients with acute exacerbations of IPF, a devastating lung disease.
Circulating autoantibodies against epithelial cells are detected by green fluorescence in patients with acute exacerbation of idiopathic pulmonary fibrosis. The intensity of the fluorescence is proportional to the autoantibody concentration. All IPF patients with acute exacerbations had abnormal increases in autoantibody concentrations pre-treatment (left image). The right image shows the reduction of fluorescence which was typical among patients who responded to treatment.Patients with acute exacerbations of idiopathic pulmonary fibrosis responded well to therapies similar to those used to treat autoimmune diseases, according to findings published today in PLOS ONE. The study suggests that autoantibodies — implicated in many autoimmune diseases such as rheumatoid arthritis or lupus — also play an important role in patients with acute exacerbations of IPF, a devastating lung disease.
“Severe acute exacerbations of IPF are medically untreatable and often fatal within days,” said Steve Duncan, M.D., professor in the University of Alabama at Birmingham Division of Pulmonary, Allergy and Critical Care Medicine. “We wanted to test the hypothesis that autoantibody-targeted therapies used to treat autoimmune disease also may benefit IPF patients with acute exacerbations.”
Duncan conducted the study between April 2011 and October 2013 while on the faculty of the University of Pittsburgh. Ten critically ill patients at the University of Pittsburgh Medical Center and one at the University of Texas Medical Branch in Galveston with acute exacerbations of IPF were involved in the study.
The 11 patients were treated with therapeutic plasma exchanges and a biologic drug called rituximab, supplemented in later cases with intravenous immunoglobulin. Outcomes among the trial subjects were compared to those of 20 historical control IPF patients treated with conventional steroid therapy prior to this experimental trial.
Autoimmune diseases are caused by a dysfunctional immune response in which the body creates autoantibodies that attack the individual’s own proteins. One of the common targets in autoimmune therapy are B cells, which are responsible for the production of autoantibodies.
The research team used between five and nine therapeutic plasma exchanges on each patient. The exchanges pumped the patient’s blood into a machine that removed autoantibodies, then returned the cleansed blood to the patient, significantly reducing the amount of autoantibodies present in the patient. The drug rituximab was then administered to further attack and kill B cells. Four of the 11 patients also received intravenous immunoglobulin, which helps to suppress B cells that may have escaped the rituximab.
Nine of the trial subjects showed improvement in pulmonary function following treatment, compared to only one of the historical controls. Two of the three patients who relapsed after five plasma exchanges responded positively with additional exchange procedures. No serious adverse events were attributable to the experimental medications.
“One-year survival of trial subjects was nearly 50 percent, which is remarkable,” said Duncan. “Acute exacerbations of IPF are almost always fatal in a very short period of time. None of the 20 historical controls survived for even a year.”
Duncan said the research team was making adaptations to the therapy as time progressed. They originally considered performing five plasma exchanges but expanded to nine for each patient as they observed the early results. They added the intravenous immunoglobulin for only the last four patients.
“No one had ever really done this before,” Duncan said. “There is not widespread agreement that IPF is an autoimmune disease. Our findings indicate that specific treatments that reduce autoantibodies might benefit some severely ill IPF patients with acute exacerbations. Therapies that have been developed to treat autoimmune diseases may prove to be beneficial in the treatment of these IPF patients.”
Duncan suggests that incremental trials of autoantibody-targeted therapies in IPF patients with acute exacerbations are justified by these results.
“Even though IPF is not considered a prototypical autoimmune disease, acute exacerbations may be driven by autoantibody production and the treatment strategy that Dr. Duncan advocates is highly innovative with the potential to reduce IPF mortality,” said Victor Thannickal, M.D., director of the Division of Pulmonary, Allergy and Critical Care Medicine. “It is now time for a randomized controlled trial of this treatment approach in IPF patients”.
Idiopathic pulmonary fibrosis is a disease of unknown origin with no approved treatments. It results in scar tissue building up in the lungs. It affects more than 100,000 people in the United States and 5 million worldwide. The median survival rate is less than three years, and only 20 percent of patients survive five years beyond diagnosis.
Study co-authors include Michael Donahoe, M.D., Kevin F. Gibson, M.D., Jianmin Xue, M.D., Ph.D., Yingze Zhang, Ph.D., and Nydia Chien, M.S.N., from the Department of Medicine, University of Pittsburgh; Melissa Saul, M.S., from the Department of Biomedical Informatics, University of Pittsburgh; Vincent G. Valentine, M.D., Department of Medicine, University of Texas Medical Branch, Galveston; and Jay S. Raval, M.D., Department of Pathology and Laboratory Medicine, University of North Carolina.
