 After decades of leading statistical and data management of several multicenter studies of stroke prevention methods, the University of Alabama at Birmingham has been awarded $10 million to provide statistical leadership and coordinate the national data for CREST-2, a $50 million pair of clinical trials that will compare various approaches to maintaining blood flow to the brain.
After decades of leading statistical and data management of several multicenter studies of stroke prevention methods, the University of Alabama at Birmingham has been awarded $10 million to provide statistical leadership and coordinate the national data for CREST-2, a $50 million pair of clinical trials that will compare various approaches to maintaining blood flow to the brain.
The management of these studies is a joint effort between UAB and the Mayo Clinic–Jacksonville, which will provide the clinical leadership. CREST-2 began at UAB’s School of Public Health this spring and is funded through 2022.
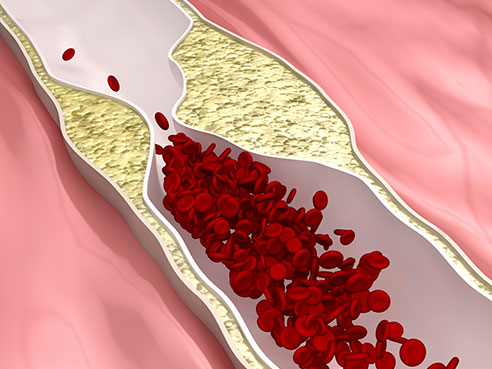
Stroke, the fourth-leading cause of death in the nation, is caused by an interruption in blood flow to the brain by a clot or bleeding. The carotid arteries on each side of the neck are the major sources of blood flow to the brain. The buildup of cholesterol in the wall of the carotid artery, called atherosclerotic plaque, is one cause of stroke. Revascularization clears the buildup in arteries to restore blood flow to the brain, to aid in preventing stroke.
Past studies have investigated various revascularization methods. The Asymptomatic Carotid Atherosclerosis Study, with co-principal investigator Virginia Howard, Ph.D., professor of epidemiology, found that asymptomatic patients who were revascularized by endarterectomy, a surgical procedure to clear blocked blood flow and prevent stroke, had a 50 percent reduction in risk of stroke.
Following the ACAS was the Carotid Revascularization Endarterectomy vs. Stenting Trial, or CREST, which was co-led by Virginia Howard and George Howard, Dr.P.H., professor of biostatistics. CREST compared endarterectomy with carotid stenting, a procedure that involves threading a stent and expanding a small protective device in the artery to widen the blocked area and capture dislodged plaque. CREST found that both were good techniques, as there were no big differences in results between the two procedures.
| The CREST-2 trials will look at the revascularization procedures as well as best medical management, including physician office visits, use of pharmaceuticals and addressing health behaviors. The two trials will each have 1,240 randomized patients recruited from approximately 120 centers in the United States and Canada. |
“Halfway through CREST, the picture changed,” George Howard said. “Primarily with the advancement of statin treatment for lipids, just being aggressively medically managed began to be debated as an attractive alternative for revascularization. So what used to be clear became totally muddy during CREST. As the trial was finishing up, the investigators and scientific community were wondering what the results would have been in comparison to a group of people who only got medicine.”
The CREST-2 trials will look at the revascularization procedures as well as best medical management, including physician office visits, use of pharmaceuticals and addressing health behaviors. The first trial will compare using best medical management in addition to endarterectomy to best medical management alone. The second trial will compare using best medical management along with carotid stenting to using best medical management alone. The two trials will each have 1,240 randomized patients recruited from approximately 120 centers in the United States and Canada.
“We will get to look at each procedure compared to medical management that includes stronger cholesterol management, better blood pressure control and other modes that were not widely used 20 years ago,” George Howard explained. “Most of the time, the intervention is the novel new treatment you’re comparing. In this case, we expect to know what happens in the groups getting the procedure. In a funny way, medical management is the new novel way. We want to know if it is better enough that a procedure is no longer needed.”
The 120 medical centers across the U.S. and Canada have not been confirmed yet, but the work at the UAB School of Public Health and Mayo Clinic–Jacksonville begins now to get all the data systems built and tested to be able to receive and analyze the data as quickly and efficiently as possible.
UAB researchers for CREST-2 include George and Virginia Howard, Virginia Wadley, Ph.D., Joan Hilner, and Richard Mailhot. CREST-2 has been awarded by the National Institute of Neurological Disorders and Stroke of the National Institutes of Health.