UAB Magazine Online Features
Aural Surgery
UAB Physician Pulls His Own Strings
By Caperton Gillett
 |
Click on the "play" button above to hear a clip of "From the Forest a Child" from Kirk Withrow's Lullaby CD. To hear more samples from Withrow's cigar-box guitars, click here. |
UAB head and neck surgeon Kirk Withrow, M.D., doesn’t stop operating when he gets home from work. His patients are a little smaller, however—and possibly more aromatic. Withrow finds his muse in cigar boxes of all sizes and shapes, which he turns into guitars that he gives away and plays himself.
UAB Magazine: How did you get interested in making cigar-box guitars?
Withrow: It was actually one of my patients who got me started. I began playing the banjo when I was 21, but during my residency I didn’t play that much. While I was on call one night—the funny thing is I had tried really hard to switch with someone else that night—a patient came in who was a cabinetmaker. He stuck around for three or four days, and over that time we talked about music. When he mentioned the idea of a cigar box guitar, I had no idea what he was talking about. But when he came back to see us at the clinic, he brought me one. I started making them and playing them, and that’s really all I play now.
Where do you get the boxes?
Mostly from cigar stores. At one store the lady actually knew which boxes would probably work well and would save them for me. The boxes are always empty when I get them. Come to think of it, I don’t actually think I have ever really smoked a cigar. (Story continues below the video)
Up in Smoke
Examining the Draw of E-Cigarettes
By Tara Hulen
 |
E-cigarettes offer a nicotine fix without the toxic smoke of traditional cigarettes, but are they really a healthier alternative to smoking? |
Cherie wants to quit smoking—again. As with a lot of former ex-smokers, this busy Birmingham businesswoman found that stress triggered a relapse. But she doesn’t yet feel ready to give quitting another try, so, in the meantime, she has chosen what she sees as a healthier option: electronic cigarettes.
E-cigarettes, as they are called, are becoming a popular intermediary step for smokers looking to gradually kick the habit—and for those, like Cherie, searching for a less toxic, less offensive substitute in the interim. The basic e-cigarette design has a tan mouthpiece designed to look like a cigarette’s filter and an LED light on the tip that can glow when active. When a smoker breathes in, a battery-powered internal atomizer creates a water vapor that draws nicotine into the mouth from a replaceable cartridge.
Clotbusters
UAB Explores Innovative Stroke Therapies
By Jo Lynn Orr
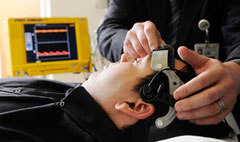 |
UAB neurologists are using ultrasound to help break up clots in the brain (above) and testing other new treatments to improve stroke care. |
In 1947, as tension between Russia and the United States threatened to erupt into nuclear war, the Bulletin of the Atomic Scientists added a new element to its cover: a stylized clock face with the hands set at seven minutes to midnight. For the past 63 years, the clock’s minute hand has moved back and forth to reflect the imminence of nuclear holocaust.
In the world of stroke care, the countdown to doomsday begins as soon as the brain’s oxygen supply is disrupted, either through a blood clot (ischemic stroke—the cause of 80 percent of strokes) or by bursting blood vessels (hemorrhagic stroke, which accounts for the other 20 percent of cases). Stroke kills more people worldwide than any other disease. It is the third leading cause of death in the United States and the leading cause of serious, long-term disability.
For years, the stroke clock was set at three hours. Patients receiving emergency treatment before that time stood a good chance of recovering significant function; after the three-hour window closed, there wasn’t much hope. But new advances in stroke treatment are steadily pushing open the treatment window and adding precious time back onto the clock. Neurologist Andrei Alexandrov, M.D., and his team at the UAB Comprehensive Stroke Research Center are contributing many of those breakthroughs, developing and testing revolutionary therapies that are effective several hours, days, and even weeks after stroke onset.
Peanut Perils
Answers About a Dangerous Allergy
By Kathy Seale
 It’s a sign of the times: Across America, the entrances to many elementary-school classrooms are now guarded by the image of a large peanut trapped behind the red circle and slash that is the international symbol for “NO.”
It’s a sign of the times: Across America, the entrances to many elementary-school classrooms are now guarded by the image of a large peanut trapped behind the red circle and slash that is the international symbol for “NO.”
Potentially deadly allergic reactions to peanuts have become a serious issue at schools, birthday parties, and anywhere else children and food mix in uncertain ways. And according to a heavily publicized study in the May 12 issue of the Journal of Allergy and Clinical Immunology, the problem is getting worse. Based on a 5,300-household survey, the study reported that the number of peanut allergies more than tripled over 10 years, from 0.4 percent of children surveyed in 1997 to 1.4 percent of children surveyed in 2008.
Extrapolating those findings nationwide is problematic, says UAB pediatric allergist and immunologist Prescott Atkinson, M.D. But the number of confirmed cases of peanut allergy in the United States is trending upward, he agrees.

