UAB Magazine Online Features
Historic Breakthroughs in Research and Clinical Care
UAB has been at the vanguard of scientific and medical discovery for decades. Here are but a few examples:

In May 2006, an international team of scientists led by UAB researchers discovered a crucial missing link in the search for the origin of HIV-1, the virus responsible for human AIDS. That missing link is the natural reservoir of the virus, which the team has found in wild-living chimpanzees in southern Cameroon.
The UAB Center for AIDS Research (CFAR) was the first to perform clinical trails of the protease inhibitor Indinavir (Crixivan), one of the first protease inhibitors used in the “triple drug cocktail” to fight HIV.
The journal Science named three UAB faculty, Drs. Michael Saag, George Shaw, and Beatrice Hahn, among the top 10 AIDS researchers in the country, and highlighted the AIDS research program at UAB in 1996.
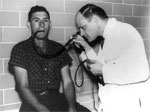 In 1960, Dr. Basil Hirschowitz (right), former director of the UAB division of gastroenterology, was the first to explore the stomach with his invention, the fiber optic endoscope, the prototype of which is now in the Smithsonian Institution.
In 1960, Dr. Basil Hirschowitz (right), former director of the UAB division of gastroenterology, was the first to explore the stomach with his invention, the fiber optic endoscope, the prototype of which is now in the Smithsonian Institution.
UAB researcher Dr. Max D. Cooper was the first to characterize B-cells as part of the human immune system. He also was first to successfully treat SCID (severe combined immunodeficiency disease) with the transplant of fetal liver cells.
 In 1977, Dr. Richard Whitley (left) administered a systemic antiviral for the treatment of the deadly HSV (herpes simplex virus) encephalitis, leading to the world’s first effective treatment for a viral disease.
In 1977, Dr. Richard Whitley (left) administered a systemic antiviral for the treatment of the deadly HSV (herpes simplex virus) encephalitis, leading to the world’s first effective treatment for a viral disease.
UAB researchers were the first to discover the protein that led to the development of the now well-known drug Viagra, causing what some have called the second sexual revolution.
UAB heart surgeon the late John W. Kirklin (right) developed a computerized intensive care unit that became a model for modern ICUs around the world. They help improve care and reduce complications. Kirklin initially gained fame by improving the safety and usefulness of the heart-lung bypass pump.
UAB was in the first handful of institutions to be designated by the National Institutes of Health as a Comprehensive Cancer Center. It is the only federally designated cancer center in Alabama and among the nation’s oldest. This means a wide range of research, education and clinical activities are available, and facilities and laboratories meet certain high standards.  UAB dentists were the first to develop the four-handed method of dentistry, where both a dentist and a hygienist treat a patient. Four-handed dentistry is now standard practice.
UAB dentists were the first to develop the four-handed method of dentistry, where both a dentist and a hygienist treat a patient. Four-handed dentistry is now standard practice.
Several UAB researchers have been the first to develop animal models for the study of a variety of diseases, including lupus, inflammatory bowel disease and sickle cell disease.  Dr. Eric Sorscher (right) was the first researcher in the United States to implant a corrected gene into the lungs of patients with cystic fibrosis using a lipid molecule delivery system.
Dr. Eric Sorscher (right) was the first researcher in the United States to implant a corrected gene into the lungs of patients with cystic fibrosis using a lipid molecule delivery system.
The first simultaneous heart-kidney transplant in the Southeast was performed at UAB by Drs. David C. McGiffin and David Laskow in 1995.  In August 1969, Dr. Henry B. Peters became the first dean of the School of Optometry, the nation’s first optometry school to be integrated into a medical center complex. The school is now one of the top optometry schools in the nation and still one of only three integrated into a medical center.
In August 1969, Dr. Henry B. Peters became the first dean of the School of Optometry, the nation’s first optometry school to be integrated into a medical center complex. The school is now one of the top optometry schools in the nation and still one of only three integrated into a medical center.
In 1987, the world’s first genetically engineered mouse-human monoclonal antibody was used at UAB Hospital in the treatment of cancer.
 In 1984, UAB Hospital became the first hospital in the United States to use color Doppler echocardiography for visualizing internal cardiac structures.
In 1984, UAB Hospital became the first hospital in the United States to use color Doppler echocardiography for visualizing internal cardiac structures.
Social Network
Behind the Scenes of BlazeRadio
By Caperton Gillett
 |
UAB students are reaching a nationwide audience and gaining valuable experience as programmers and managers of the university's Internet radio station. |
There’s a deejay booth sitting right behind a floor-to-ceiling panel of glass on a main artery in the Hill University Center, and yet most students don’t notice it until they tune in to BlazeRadio, UAB’s student-run online radio station. Each week, for several hours per day, students take to the airwaves—or, rather, the Internet—to send music, news, sports coverage, and conversation out to an audience that spans the country. Anything, that is, that “people can feed off of, that they can enjoy listening to,” says Ryan McLaughlin, junior broadcast major, deejay, and general manager of the station.
McLaughlin’s personal programming includes an eclectic mix of hip-hop music, banter, the occasional in-studio guest, and, on Wednesday evenings, a top-15 countdown show with two of his friends joining him behind the mic and call-in topics ranging from STDs to relationships to, in one case, old-school cartoon theme songs. The show is built on “the random thoughts you always have that you’ve never bothered to say,” McLaughlin says.
Communication Station
Unraveling a Cellular Mystery
By Matt Windsor
 |
 |
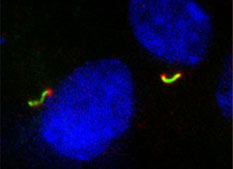
Once dismissed as the cellular equivalent of tonsils, primary cilia are now known to be invaluable antennae that help cells sense their environment. UAB's Bradley Yoder has helped connect primary cilia with a host of human ailments, from kidney disease to obesity and even cancer. At top, primary cilia (colored green and red) protrude from renal epithelial cells grown in culture. |
In cell biology, as in love, you often don’t know what you’ve got till it’s gone. For more than a century, scientists have known that most cells in the human body come equipped with an odd projection on their outer surfaces called the primary cilium. Unlike the wavy, hairlike cilia you may remember from biology class—the ones that sweep mucus out of the airways—the primary cilia are rigid and didn’t seem to have any useful function. They were written off as vestigial, like tonsils or the appendix.
But 10 years ago, a handful of cell biologists including UAB’s Bradley Yoder, Ph.D., began to unravel the secrets of this obscure organelle. Starting in green algae and only lately moving up to humans, they made a startling discovery: If a cell loses its cilium, bad things begin to happen. Their investigations have revealed that, far from being an artifact, the primary cilium is actually an important communications device—and a major player in human growth and development, kidney disease, obesity, wound healing, and even cancer.
“Human patients with ciliary defects are often blind, they can’t smell, and they have difficulty hearing,” says Yoder. “It turns out that the cilia are loaded with receptors and channels that allow a cell to sense its environment and communicate with that environment.”
Cilia in the embryo help determine the overall body plan, including the key directive to put the heart just to the left of the centerline. (One genetic defect in the cilia causes people to be born with a completely reversed body plan, says Yoder: “Everything’s on the wrong side.”) Cilia on the rods and cones of the eye gather and respond to light. Cilia in the nose sense and react to odors. Primary cilia are involved in so many sensory functions, Yoder says, that they have earned the name “the antennae of the cell.”
Green Growers
Tending a Student-Led Investment Fund in Tough Times
By Caperton Gillett
 |
For a group of students in the UAB School of Business, the colors green and gold evoke something besides school spirit. That’s the result of some wise moves by the Green and Gold Fund, UAB’s student-managed investment portfolio, which continues to rise even in the midst of a recession.
“We’ve got a lot of cash right now, which is fun, because there are a lot of long-term opportunities—if you’re particular about what you purchase,” says Stephen Garrett, a finance student who is the chief investment officer on the fund. Garrett describes his role as “part of a team that manages a chunk of money around here.” In other words, he monitors the fund’s portfolio and works with the analysts and managers to maximize performance while keeping risk to a minimum.
Finance faculty started the fund in 2005 to provide students with career experience in the fast-paced world of investments long before graduation. In 2008, the fund won first place against 50 other undergraduate growth-style portfolios at the RISE (Redefining Investment Strategy Education) forum and national collegiate competition. Both CNBC and BusinessWeek magazine have spotlighted the team’s success.
