We're Moving!

The UAB Department of Otolaryngology Admin Office will be moving offices effective Monday, May 13th. Below you will find our updated contact information.
PHYSICAL ADDRESS
1155 Faculty Office Tower
510 20th Street South
Birmingham, AL. 35233
P: 205-801-7801 F: 205-801-7802
MAILING ADDRESS
FOT 1155
1720 2nd Avenue South
Birmingham, AL. 35294-3412
Welcome New ResidENTs!
The Department of Otolaryngology is excited to welcome four residents to UAB this summer. Meet our new PGY-1 team:
 Jessica Lee Bishop attended the Medical College of Georgia at Augusta University for medical school. She received her Bachelor of Science from the Georgia Institute of Technology. Jessica was born in Birmingham, Alabama.
Jessica Lee Bishop attended the Medical College of Georgia at Augusta University for medical school. She received her Bachelor of Science from the Georgia Institute of Technology. Jessica was born in Birmingham, Alabama.
 Sudhir Manickavel was born in Gobichettipalayam, India and attended the University of California for his undergraduate degree. He completed medical school of the University of South Florida Morsani College of Medicine in Tampa, Florida.
Sudhir Manickavel was born in Gobichettipalayam, India and attended the University of California for his undergraduate degree. He completed medical school of the University of South Florida Morsani College of Medicine in Tampa, Florida.
 Jake Patrick Morgan completed medical school at the University of Oklahoma School of Medicine in Oklahoma City. Born in Tulsa, Oklahoma, he attended the University of Oklahoma for his undergraduate degree.
Jake Patrick Morgan completed medical school at the University of Oklahoma School of Medicine in Oklahoma City. Born in Tulsa, Oklahoma, he attended the University of Oklahoma for his undergraduate degree.
 Ashwini Milind Tilak was born in Sabt Al Alayah, Saudi Arabia. Before attending medical school at the University of Viriginia in Charlottesville, she received her Bachelor of Science from the University of Miami.
Ashwini Milind Tilak was born in Sabt Al Alayah, Saudi Arabia. Before attending medical school at the University of Viriginia in Charlottesville, she received her Bachelor of Science from the University of Miami.
Q&A: Earbuds and Hearing Loss
 We sat down Dr. Benjamin McGrew, a neurotologist with the Department of Otolaryngology at UAB, to discuss the how earbuds can cause hearing loss and how to use them safely.
We sat down Dr. Benjamin McGrew, a neurotologist with the Department of Otolaryngology at UAB, to discuss the how earbuds can cause hearing loss and how to use them safely.
- Is noise from headphones more dangerous because it's closer to our eardrums?
It’s really all about volume and duration of noise exposure. No headphones or earbuds are inherently good or bad for your hearing; however, sound intensity is likely increased because of the close proximity of earbuds to your ear drums. - Are people experiencing hearing loss at younger ages because of the prevalence for wandering around with our headphones and earbuds in?
I have seen children with noise-induced hearing loss because of earbud/headphone use for long periods of time at loud levels; however, exposure to harmful noise can happen at any age. - What's the highest decibel we should ever go to when listening on our headphones and earbuds? And the maximum length of time?
Whether or not you’re using earbuds, attending a concert or participating in certain recreational activities, sounds at 85 decibels can lead to hearing loss if you listen to them for more than eight hours at a time. Anything above 91 decibels, your safe listening time is cut down to two hours. You can listen to sounds below 85 decibels for as long as you want without causing any nerve damage.
Some smartphones are able to reach 120 decibels. According to the Occupational Safety and Health Administration (OSHA), decibels at this level are capable of causing noise-induced hearing loss in less than 15 minutes. - What should we look for in headphones/earbuds to protect our hearing?
Competing sounds may cause earbud users to increase the volume on their devices to dangerous levels. Noise-isolating over ear headphones or squishy earbuds can limit the ambient noise you hear from the world around you, thus helping you resist the need to turn up the music. - How do we know if we've already damaged our hearing?
Because the damage from noise exposure is usually gradual, you may not notice you’ve damaged your hearing until the symptoms become more pronounced. Sounds may become distorted or muffled and you might find yourself turning up the volume on the television or have difficulty understanding people.
If you’ve ever experienced ringing in your ears after loud noise exposure, you have damaged your ears. Tinnitus from loud noise exposure often results in temporary hearing loss and resides in less than 72 hours.
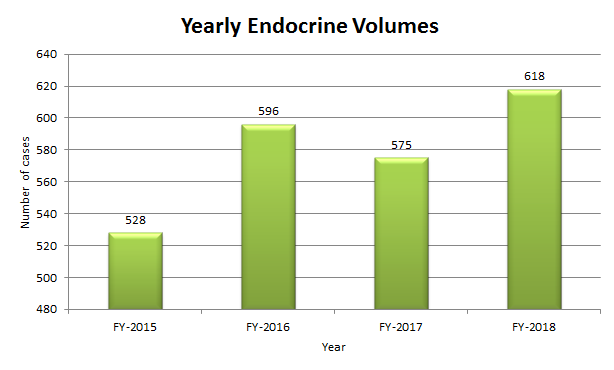
Latest Endocrine Update
The Department of Otolaryngology’s endocrine volumes have been on the rise in recent years. In 2018, the department had more than 618 thyroid and parathyroid cases.
 “Our endocrine volumes are some of the highest in the nation,” said Dr. Glenn Peters, Julius N. Hicks Professor of Otolaryngology. “Our numbers have been on the rise the last four years and I believe they will continue to trend upward.”
“Our endocrine volumes are some of the highest in the nation,” said Dr. Glenn Peters, Julius N. Hicks Professor of Otolaryngology. “Our numbers have been on the rise the last four years and I believe they will continue to trend upward.”
The department sees everything from parathyroid and thyroid cases.
In case you missed it, Dr. Erin Buczek, Dr. Benjamin Greene and Dr. Brian Hughley were featured twice on UAB MedCast, a continued medical education podcast that highlights the latest clinical and research innovations at UAB Medicine. Each podcast episode qualified for a 0.25 AMA PRA Category 1 credit. Listen to their podcasts by following the links below.
Thyroid Disease and Thyroid Cancer
The Intricate Nature of Head and Neck Surgery
Woodworth Attends 48th Brazilian Congress of Otorhinolaryngology
Dr. Bradford Woodworth recently traveled to João Pessoa, Paraíba, Brazil for the 48th Brazilian Congress of Otorhinolaryngology and Head and Neck Surgery and was one of nine international guests. During his time there, Dr. Woodworth was involved in multiple roundtable discussions and gave several presentations, including:
-
Acquired CFTR dysfunction in chronic rhinosinusitis
-
Revision endoscopic sinus surgery: How to improve outcomes
-
Evolving treatment paradigms for CSF leaks and frontal sinus trauma
During his free time, Dr. Woodworth was able to visit Ponta do Seixas, a cape on the Atlantic coast that forms the easternmost point of the American continents. The landmark defines the place where the sun first rises in the Americas.

Alumni Spotlight: Dr. Angela Blount
 When did you graduate from UAB?
When did you graduate from UAB?
I graduated in 2012.- What city are you located in?
I live in Birmingham, AL and work for ENT Associates of Alabama. Our practice covers 8 hospitals/clinics in and around Birmingham. My office is located at Baptist Walker Regional Medical Center in Jasper. - What are your clinical/research interests?
General Otolaryngology. I appreciate the amazing research being done in ENT but hope I never have to write another research paper again. - How did you choose to practice this area of otolaryngology?
I know everyone says the variety, but it’s true, I get bored doing the same thing. - What aspect of your time at UAB do you believe was most valuable as you started your career?
The most valuable and yet worst part of residency was being on call. Making the best decisions you can on your own is the foundation of practicing medicine. After residency call, all other calls seem to pale in comparison. You can pretty much handle anything. - Did you have a particular mentor while at UAB? Why were they a good mentor?
I had so many good mentors that it is hard to pick just one. The attendings poured so much into me, and because of them I have a great livelihood. I still remember a particularly bad day, when Dr. Scott Hill told me to go home, relax, have a glass of wine, and come back tomorrow to do it all again. They taught me to just keep going. - What is one of your fondest memories from UAB?
My fondest memories would be the relationships I formed with my co-residents. Their humor made residency so much more enjoyable. I still keep in touch with them today. - Give one piece of advice you’d like to share with the current residents or those recently graduated.
Residency is only a small part of your life, and be assured your life will be your own again. - Hobbies/Interests: When you’re not working, how do you spend your time?
Haha what time? I have 2 young kids, and so most of my time is spent taking care of them. If I am lucky, I can get a run in a few times a week.
Second Annual Head & Neck Recon Lecture and Cadaver Course
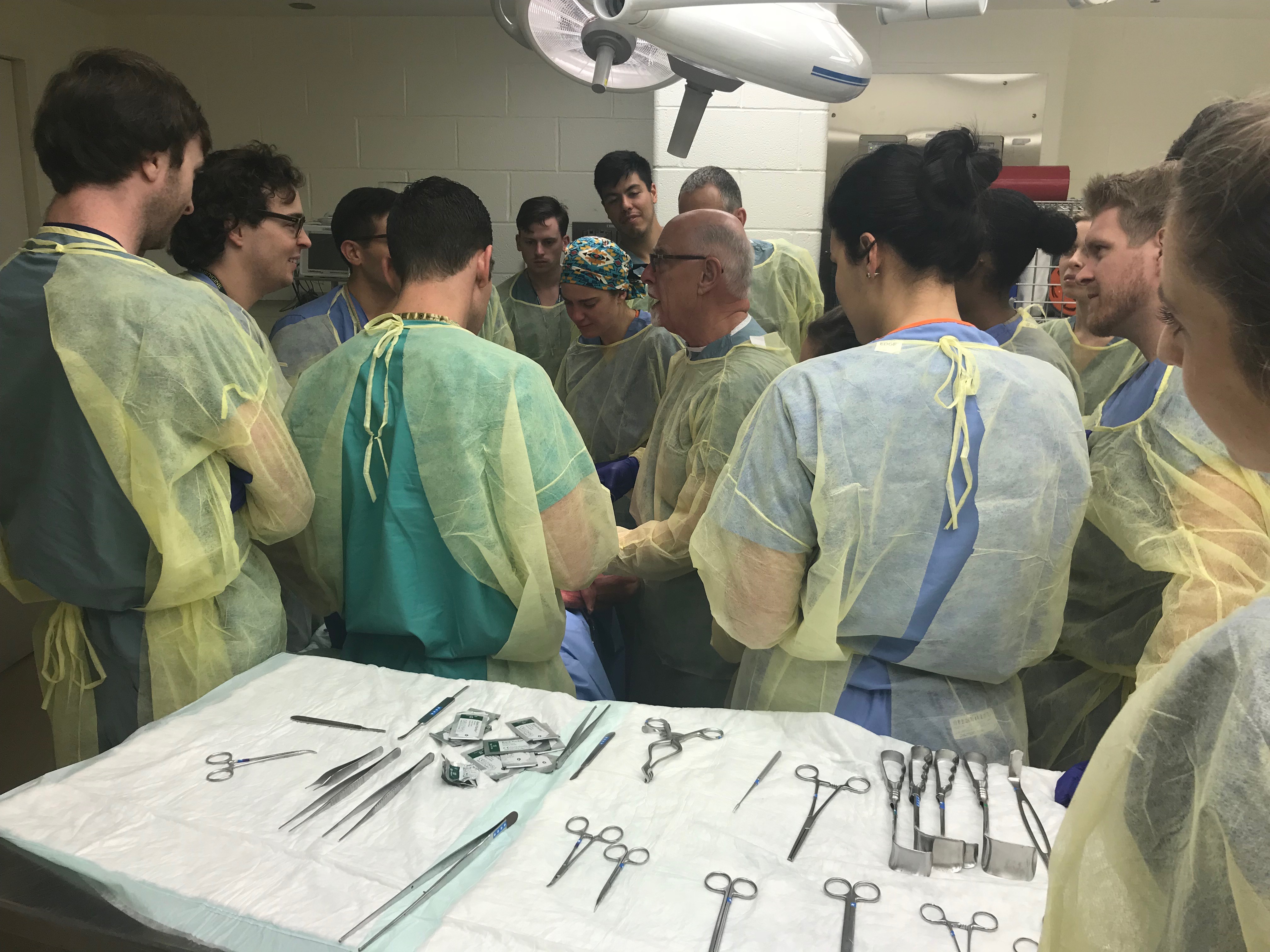
The Department of Otolaryngology’s second annual Head and Neck Reconstruction Lecture and Cadaver Course was held on October 26-27 for UAB and University of Mississippi otolaryngology residents. The two-day course was led by Dr. Richard Hayden, Professor of the Department of Otolaryngology-Head & Neck Surgery at the Mayo Clinic. Attendees participated in a lecture on “Training in Pedicle Flaps and Small/Large Free Flap Reconstruction” and were later able to practice what they learned in a hands-on, instructed cadaver lab. Hayden is also the education director at the Center for Regenerative Medicine.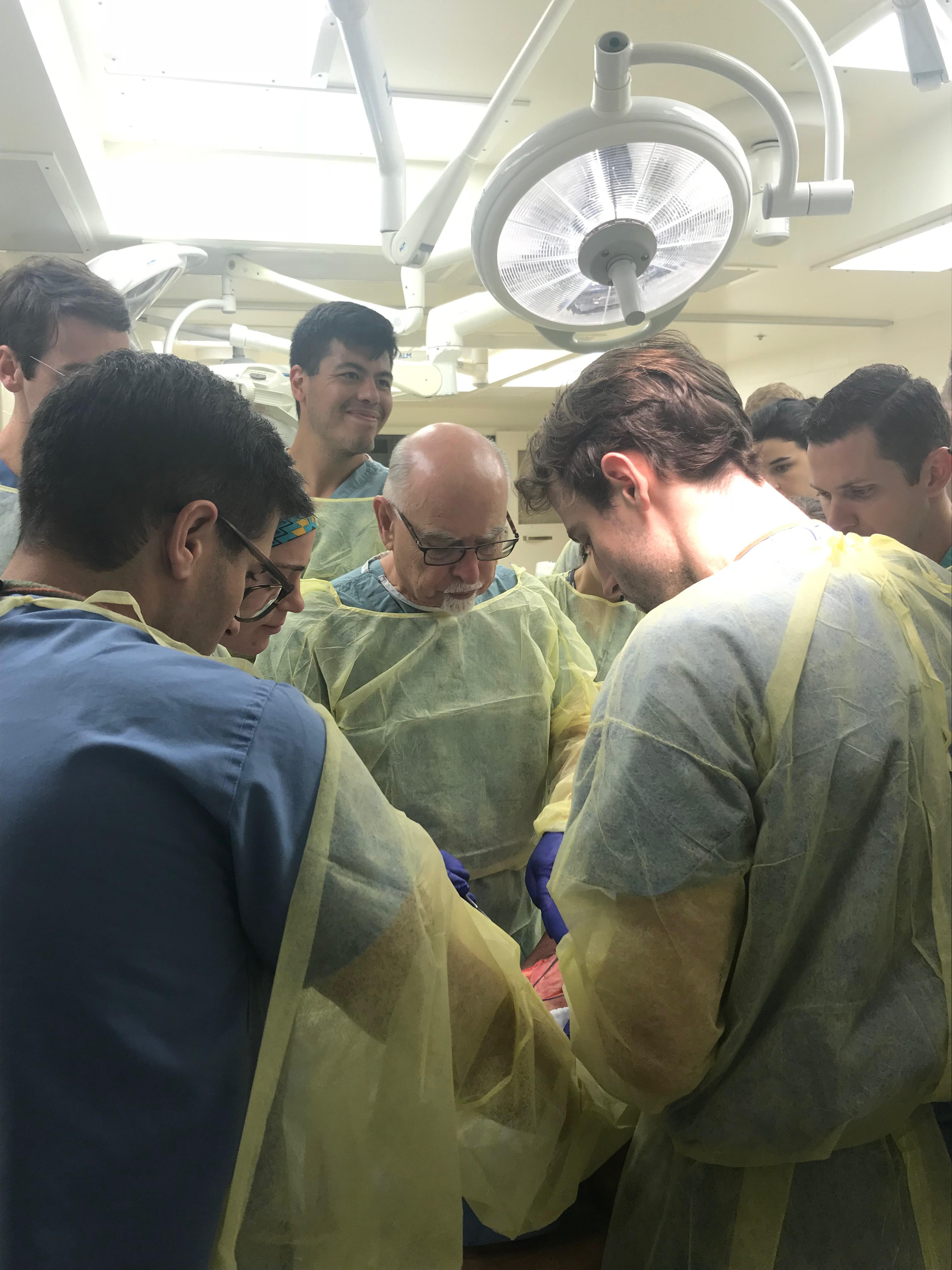
2018 George W. Barber, Jr. Lectureship
 The 2018 George W. Barber, Jr. Lectureship in Otolaryngology was a favorite for many faculty, residents and staff. The topic, "Inspiring Change from Within: What We Can Do to Address Biases for the Future of Healthcare," was presented by Dr. Dana Mara Thompson, Professor of Otolaryngology Head and Neck Surgery, Northwestern University Feinberg School of Medicine, The Lauren D. Holinger Chair in Pediatric Otolaryngology, Division Head, Otolaryngology - Head and Neck Surgery, Ann & Robert H. Lurie Children's Hospital of Chicago.
The 2018 George W. Barber, Jr. Lectureship in Otolaryngology was a favorite for many faculty, residents and staff. The topic, "Inspiring Change from Within: What We Can Do to Address Biases for the Future of Healthcare," was presented by Dr. Dana Mara Thompson, Professor of Otolaryngology Head and Neck Surgery, Northwestern University Feinberg School of Medicine, The Lauren D. Holinger Chair in Pediatric Otolaryngology, Division Head, Otolaryngology - Head and Neck Surgery, Ann & Robert H. Lurie Children's Hospital of Chicago.
Dr. Do-Yeon Cho, Assistant Professor and Director of Otolaryngology Research, UAB Department of Otolaryngology, speaks in detail about Dr. Thompson's lecture:
-
How will attendees be able to use lessons from Dr. Thompson's talk in their own careers, whether as students, educators, researchers or clinicians?
Millennial education required a change from within myself and we need to continue to change and stay relevant. We aspire to cultivate an environment of diversity and inclusion, advance diversity (race, gender, religion, etc.) as a key to excellence and enhance the recruitment, career development, and retention of students, trainees and faculty. -
How did the lecture speak to the present and future of the field of otolaryngology?
Dr. Dana Thompson is a world renown pediatric otolaryngologist and calls for more diversity in medicine, which means more female and minority representation in the field of otolaryngology. Her grandfather, who graduated from Meharry Medical College in Nashville, Tenn. in 1927, was the only African American general practitioner within a 100-mile radius of his office in Aberdeen, Miss. Dr. Thompson’s father was another Meharry Medical College alumni, an obstetrician in Kansas City, Kan. He told his daughter early on that she couldn’t live her dream of being Howard Cosell of Monday Night Football fame, but instead, he brought her to his office and to the hospital to make rounds with him to show her what she could be. He instilled into her psyche that she would have to work four times harder than everyone else just to be on the same playing field. African Americans make up only 2.3 percent of all otolaryngologist residents in training, well below percentages in other specialties and the overall population. “Continued success requires recognition of how one’s own biases get in the way of compassionate patient centric care,” Thompson said. Then our future will be brighter. -
How did this talk relate to previous George Barber Lectures?
Since becoming the director of research of our department, I have been inviting the most world-renown otolaryngologists or pioneer scientist in the field of otolaryngology who can motivate and inspire our department and community. This year was different from most as we focused more on our culture than surgical practices. Dr. Thompson left us all very inspired and wanting to do better. She was the first African American female intern in general surgery, the first African American female resident in Otolaryngology, the fourth African American resident in Otolaryngology and the fourth female resident in Otolaryngology. Her lecture, “Inspiring Change from Within: What We Can Do to Address Biases for the Future of Healthcare,” was as much a heartfelt explanation of her personal journey as it was a prism through which to view a future for our society.
Alumni Spotlight: Dr. Jasper Castillo
When did you graduate from UAB?
I finished the UAB Otolaryngology Residency Program in 1993.- Where are you now?
I currently live in Gurley, Alabama and work in Huntsville, Alabama. We have 9 ENT docs in our practice, North Alabama ENT Associates. I completed a Pediatric Otolaryngology Fellowship in San Diego and then worked at Nemour's Children's Clinic in Jacksonville, Florida for 2 years before coming to Huntsville. 99% of my practice is pediatric and I see consults at the Women's and Children's part of Huntsville Hospital almost daily. When taking call, I see "all comers". - What aspect of your time at UAB do you believe was most valuable as you started your career?
Obviously, my time at Children's Hospital in Birmingham was very important. Dr. James Reilly was the Chief of Pediatric Otolaryngology and he was instrumental in helping me to land the fellowship in San Diego. - Did you have a particular mentor while at UAB? Why were they a good mentor?
Dr. Reilly was a great mentor. Dr. Peters was outstanding as well. I don't believe any program in the country had better Head and Neck training than UAB had under the tutelage of Dr. Peters. We were "fellowship trained" in Head and Neck while in residency. - What is one of your fondest memories from UAB?
We had great camaraderie among the residents. John Jebeles and Mike Sillers were in my year and we instituted the DNR Trach/FESS during the PGY-3 consult service. - Give one piece of advice you’d like to share with the current residents or those recently graduated.
The best advice for training is to consider that any and every day, a patient can show up on your doorstep and you're it. No one else to punt to, no transfers available. See as much as you can and do as much as you can while you have back-up available. - Hobbies/Interests: When you’re not working, how do you spend your time?
My kids are all out of the house now. Oldest son is a meteorologist with the National Weather Service. Oldest daughter is in medical school at Baylor in Houston. Youngest daughter and son are both in college at Alabama. I coached travel hockey for almost 20 years and now play hockey 2-3 mornings a week before work. Also still ride bikes a lot. Dr. Teachey (UAB Otolaryngology 1995) and I are participating in the Race Across America in June 2019. I try to find time in my day to play guitar.

Take 5 with Dr. Do-Yeon Cho
 What made you want to become a physician?
What made you want to become a physician?
After finishing medical training in South Korea, I was appointed to work as a humanitarian medical officer for the Korean Government for three years in lieu of military duty. During those three years, I had thought about switching my career from a clinician to an administrative officer. Although my work was gratifying, I came to believe that advances in translational research held the potential for even more significant impact on disease prevention and management than was possible through administrative outreaches. Therefore, I decided to re-train in the US (enriched research environment) and finished my Otolaryngology residency at Stanford University with two additional years of a research fellowship.- What is the best part of your job?
The evolution of medicine depends on the successful translation of basic science research from the bench to clinical implementation at the bedside. As a clinician-scientist, I am trying to bridge the gap between research in the basic sciences and clinical medicine in the field of upper airway diseases (chronic rhinosinusitis, chronic rhinitis, cystic fibrosis), and eventually make important contributions to healthcare. - Who is a mentor who has had a profound influence on your life?
There are a lot of people who have had a tremendous influence on my life. Regarding my career development, there are two mentors: Dr. Peter H. Hwang at Stanford University and Dr. Bradford A. Woodworth at UAB. Dr. Hwang has always supported and encouraged me to pursue my dreams while challenging me to be the best that I can. Dr. Woodworth is an excellent goal-setter and has inspired me to set high goals for myself and work hard to reach them. They are great writers and editors. They magically edit what I write and are always to the point. - What does the future of medicine look like in your area of interest?
About two years ago, I did have a book club with our residents focusing on "The Digital Doctor" by Robert Wachter. Based on that book, I would imagine this: In the clinic, the clinic note will be created by physicians and other team members mainly through speaking, rather than writing and thousands of clicking. Consultations with specialists will be completely reimagined. A new system of national physician licensure, enacted to facilitate telemedicine, will allow consultations to cross state boundaries. There may even be instances in which consultants are in other countries. While physicians will still be ultimately responsible for making a final diagnosis, the electronic health records will suggest possible diagnoses for the physicians to consider, along with the tests and treatments based on guidelines and literature that are a click or a voice command way. - How do you like spending your time off?
I love traveling and cooking. I am try to make very authentic Korean cuisine using traditional ingredients. Usually, my reference is YouTube videos. I once made Kimchi (fermented spicy cabbage) here in Birmingham by myself, which wasn’t easy at all. I have visited about 40 countries, including North Korea and Eritrea (the two most isolated countries in the world). During my time off, I am planning my next trip. I would like to visit Easter Island and Iceland in the near future.
AAO-HNSF 2018 Annual Meeting Recap
AMERICAN RHINOLOGIC SOCIETY MEETING
- Top 15 Abstract Session
“The ciprofloxacin and ivacaftor coated sinus stent has sustained activity against pseudomonas aeruginosa biofilms” - Do-Yeon Cho, MD - Moderator: Do-Yeon Cho, MD / Bradford A. Woodworth, MD
“Ivacaftor Improves Rhinologic, Psychologic, And Sleep-related Quality Of Life In G551d Cystic Fibrosis Patients” - Justin McCormick, MD - Top 15 Abstract Session
“Herbal Dry Extract BND 1011 Improves Clinical and Mucociliary Parameters in a Rabbit Model of CRS” - Do-Yeon Cho, MD
KOREAN AMERICAN SATELITE SYMPOSIUM DINNER
- Korean American Otolaryngology Society Travel Grant – Sean Evans, MD (PGY5, UAB)
SOHN 42ND ANNUAL CONGRESS AND NURSING SYMPOSIUM
- “Pediatric Congenital Hemangioma and Vascular Malformations” - Brian Kulbersh, MD
AAO-HNSF ANNUAL MEETING
- Oct 7th: Panel Presentation “Smoking Cessation: What Treatments Works and How to Bill Effectively” - Richard Waguespack, MD (Panelist)
- Oct 7th: Expert Series “Coding and Auditing for the Compliance Officer: Part I" - Richard Waguespack, MD (Co-Presenter)
- Oct 7th: Expert Series “Coding and Auditing for the Compliance Officer: Part II” - Richard Waguespack, MD (Co-Presenter)
- Oct 7th: Expert Series “Hot Coding Topics in Otolaryngology 2018” - Richard Waguespack, MD (Lead Presenter)
- Oct 7th: Panel Presentation “Board of Governors Hot Topics: Infection Control 2018-Safety, Sterility, and Control” - Susan D. McCammon, MD (Panelist)\
- Oct 8th: Panel Presentation “21st Century Carrier Relations: Building Collaboration and Trust: Part I” - Richard Waguespack, MD (Panelist)
- Oct 8th: Panel Presentation “21st Century Carrier Relations: Building Collaboration and Trust: Part II” - Richard Waguespack, MD (Panelist)
- Oct 8th: Lunch with the Experts – Rhinology: Expert Host Bradford A. Woodworth, MD
- Oct 8th: Scientific Oral Presentations: Sleep Medicine “Response to Upper Airway Stimulation in Older Adults with Moderate to Severe Obstructive Sleep Apnea” - Sean Evans, MD (Presenter)
- Oct 8th: Scientific Oral Presentations: Rhinology/Allergy: Do-Yeon Cho, MD (Moderator)
- Oct 8th: Expert Series “Laryngectomy in the Era of Chemoradiation 2018” - William R. Carroll, MD (Lead Presenter)
- Oct 9th: Panel Presentation “Advance Practice Providers in ENT: Justify, Recruit, and On-Board for Success: Part I” - Kristina Gidley PA-C, MSHA (Panelist)
- Oct 9th: Panel Presentation “Advance Practice Providers in ENT: Justify, Recruit, and On-Board for Success: Part II” - Kristina Gidley PA-C, MSHA (Panelist)
- Oct 9th: Expert Series “Management of Chronic Rhinosinusitis in Systemic Inflammatory or Genetic Diseases” - Bradford A. Woodworth, MD (Lead Presenter), Do-Yeon Cho, MD (Co-Presenter)
- Oct 9th: Rapid Poster Presentations: Do-Yeon Cho, MD (Moderator)
UAB Ear, Nose and Throat ranked #29 in U.S. News Best Hospitals
 The U.S. News & World Report’s (USNWR) Best Hospitals Rankings 2018-2019 lists UAB Ear, Nose and Throat (ENT) No. 29 nationally. This is the ninth consecutive year UAB ENT has been recognized by USNWR Best Hospitals.
The U.S. News & World Report’s (USNWR) Best Hospitals Rankings 2018-2019 lists UAB Ear, Nose and Throat (ENT) No. 29 nationally. This is the ninth consecutive year UAB ENT has been recognized by USNWR Best Hospitals.
“UAB ENT is committed to providing outstanding patient care and we believe this national recognition reflects both our dedication and expertise across the spectrum of head and neck disorders,” said William R. Carroll, M.D., Chair, UAB Department of Otolaryngology.
A hospital’s score for ENT is based on various data categories, including volume of high-risk patients, nurse staffing and patient survival. UAB ENT was ranked highly for patient safety, number of patients and patient services, among other factors.
Overall, UAB Hospital was again ranked No. 1 in Alabama. Nine other UAB adult specialties joined ENT in the nation’s top 50, and three adult specialties and seven procedures/conditions were named High Performing.
UAB's highest ranked programs include:
- Rheumatology (10)
- Nephrology (13)
- Pulmonology (16)
- Cardiology & Heart Surgery (18)
- Gynecology (25)
- Diabetes & Endocrinology (28)
- Ear, Nose & Throat (29)
- Urology (34)
- Neurology & Neurosurgery (36)
- Geriatrics (42)
USNWR also recognized UAB for High Performance in three adult specialties, including gastroenterology & GI surgery, Cancer and Orthopedics.
Take 5 with Dr. Susan McCammon
- What made you want to become a physician?
A passion for helping. All people have an equal shot at health and a sense of safety and well-being.
- What is the best part of your job?
Listening to patients talk with me and their loved ones about what is really important to them and learning how they make choices so that I can help them with high-risk health care decisions. Similarly, working with students of all levels to help them find their purpose and flourish in it.
- Who is a mentor who has had a profound influence on your life?
Dr. Glenn Peters and Dr. Bill Carroll taught me how to care for people with head and neck cancer from the very beginning. I still hear their voices in my ear when operate. Dr. Lee Grumbles helped me understand the incredible power of supportive care and palliative medicine in surgical patients.
- What does the future of medicine look like in your area of interest?
The future of medicine in both head and neck surgery and in palliative medicine and supportive care will be shaped by the voices and identities of individual patients. Goals for treatment and survivorship will be discussed from the very beginning of a serious illness diagnosis. Supportive and advance care planning will be integrated into all patient-centered care, not just end-of-life care.
- How do you like spending your time off?
Cooking, reading, driving the back roads of Alabama and getting to know the different counties. I also love visiting and sharing books and recipes with my husband Tom and my family in Tuscaloosa, Prattville and Mobile.
Farewell 2018 PGY-5 Residents!



Alumni Spotlight: Dr. Nathan Alexander
 Dr. Alexander and his wife Kim at Cure Hospital in Kijabe, Kenya where he goes on an annual mission trip for cleft lip and palate repair. This year, he will help with airway surgery.When did you graduate from UAB?
Dr. Alexander and his wife Kim at Cure Hospital in Kijabe, Kenya where he goes on an annual mission trip for cleft lip and palate repair. This year, he will help with airway surgery.When did you graduate from UAB?
2012- Where are you now?
Greenville Health System Children's Hospital in Greenville, SC. - What are your clinical/research interests?
Clinical – pediatric otolaryngology – pediatric airway, cochlear implantation, and head/neck. - How did you choose to practice this area of otolaryngology?
I felt like it was a very rewarding facet of otolaryngology as it provides such a life changing impact early on in the life of a child, and their family. - What aspect of your time at UAB do you believe was most valuable as you started your career?
The attendings at UAB had an excellent ability to balance instruction and autonomy with surgical progression. We were able to do an incredible number of cases and that helped to increase surgical confidence as I transitioned into fellowship and then practice. These things also helped to solidify principles and memories that still surface every time I do a particular case. - Did you have a particular mentor while at UAB? Why were they a good mentor?
I didn’t have one particular mentor while in residency. Several attendings at UAB and Children’s helped really shape the way that I practice, operate, and maintain work-home balance. - What is one of your fondest memories from UAB?
I am particularly fond of the unique dynamic where we fostered real friendships with our attendings all while they trusted and allowed us to share in their operations and their day to day practice. I worked a ton and felt like we made a real difference. - Give one piece of advice you’d like to share with the current residents or those recently graduated.
Take notes. There are so many pearls within the five years of residency, it’s easy and unfortunate to leave some in short term memory. The details of a Peter’s thyroid, a Carroll neck, a McGrew mastoid, a Woodworth FESS (just to name a few) are priceless. - When you’re not working, how do you spend your time?
When not at work, I enjoy being home with my wife and five kids and exercising.
Caring for Your Voice
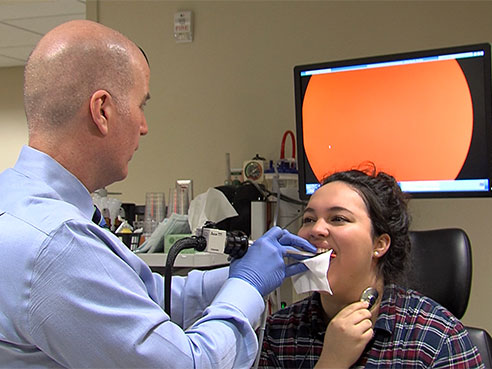 Forget texting with friends and emailing coworkers. The most important asset we have to engage in meaningful conversation is our voice. What other tool can explain, encourage or make a difference?
Forget texting with friends and emailing coworkers. The most important asset we have to engage in meaningful conversation is our voice. What other tool can explain, encourage or make a difference?
But like any part of our bodies, our voices need to be looked after. World Voice Day is an annual worldwide event devoted to the celebration of that invaluable tool.
Each of us has a unique vocal signature comparable to a fingerprint. The voice includes defining characteristics of pitch, loudness, resonance and clarity, all of which lead to presumptions about our intelligence, mood, influence, confidence and desires. The unique variation of these characteristics is distinctly recognizable, closely associated with our identity and therefore should be something that we cherish when navigating the many thousands of choices that we make daily.
Richard McHugh, M.D., assistant professor for the University of Alabama at Birmingham Department of Otolaryngology and co-director for the UAB Voice Center suggests making your vocal hygiene a priority by implementing these healthy lifestyle choices:
- Drink an adequate volume of water each day
- Avoid overuse and abuse (yelling, strain, chronic throat clearing, speaking in glottic fry)
- Quit smoking, avoid smokeless tobacco and exposure to secondhand smoke
- Limit intake of acid reflux-inducing foods and activities
“One of the most common problems that people experience is called muscle tension dysphonia,” said McHugh. “This occurs when the act of speaking with muscle over usage and strain leads to hoarseness. It can be a result of many different things including voice overuse or abuse, or from laryngitis among many other causes.”
If you feel that your voice is having problems such as roughness, strain, hoarseness or weakness lasting more than a few weeks, make an appointment with your otolaryngologist or laryngologist for an evaluation.
A laryngologist may be needed for treatment of problems that require surgery. These specialists are also able to diagnose uncommon voice disorders. Another part of your patient care team may include a speed pathologist who works to teach the healthiest technique to produce voice by optimizing breath support and minimizing laryngeal muscle strain through rehabilitative exercises and techniques.
“We are so privileged to be a part of caring for patients with voice trouble, said Bridget Hopewell, M.D., Assistant Professor of Otolaryngology at UAB. “There are so many people who rely on their voices for their careers in addition to facilitating relationships with other people. Our goal is to help keep voices healthy so patients can continue speaking, teaching, preaching, or singing!”
For more information, visit www.uab.edu/medicine/otolaryngology.
Lectures Around the World
Dr. Bradford Woodworth has been traveling a lot lately, but not for pleasure. He has been asked to present lectures at institutions as close as San Antonio, Texas and as far as Melbourne, Australia. Dr. Woodworth is always eager to provide his insight on various topics like rhinosinusitis, cystic fibrosis, sinus trauma and CSF leaks. Below is a list of some of his recent lectures:
- International Congress Faculty/Scientific Program Speaker, "Transnasal Endoscopic Management of Frontal Sinus Trauma." Rhinology World Congress, Hong Kong, China, August 31-September 3, 2017.
- Keynote Speaker, "Acquired CFTR Dysfunction in Chronic Rhinosinusitis." Stanford University Otolaryngology 8th Annual Research Day, Stanford, CA, October 23, 2017.
- International Guest Faculty/Invited Speaker, "Cystic Fibrosis" & "Endoscopic Management of Frontal Sinus Fractures" & "Management of Spontaneous CSF leaks and Idiopathic intracranial hypertension", 2017 Victorian Sinus and Rhioplasty Dissection Course, Oct 27-29, Melbourne, Australia.
- Visiting Professor/Invited Speaker, “Evolution of Treatment Paradigms for CSF Leaks and Frontal Sinus Trauma.” University of Pennsylvania Department of Otorhinolaryngology Grand Rounds, Philadelphia, PA, November 9, 2017.
- International Guest Faculty/Invited Speaker, “Management of AFS, ASA Triad, and CD Frontal Sinus Disease.” & “Draf IIB Frontal Sinusotomy: How I Do It.” 7th Nottingham Advanced Frontal Sinus Surgery Course, Coventry, UK, January 22-23, 2018.
- Invited Speaker, "Transnasal Endoscopic Management of Frontal Sinus Trauma" for panel on Management of Anterior Skull Base Trauma. North American Skull Base Society Annual Meeting, February 18, 2018.
- Holt Visiting Professor on Translational Research. “Acquired CFTR Dysfunction in Chronic Rhinosinusitis.” University of Texas Health – San Antonio, San Antonio, TX, March 6, 2018.
- Holt Visiting Professor on Translational Research. “Evolving Treatment Strategies for CSF Leaks and Frontal Sinus Trauma.” University of Texas Health – San Antonio, San Antonio, TX, March 6, 2018.
 Dr. Woodworth and Dr. Philip Chen, program director at UTSA, in front of the Alamo.
Dr. Woodworth and Dr. Philip Chen, program director at UTSA, in front of the Alamo.
Alumni Spotlight: Dr. Alexandra Kejner
- When did you graduate from UAB?

2014. - Where are you now?
Univeristy of Kentucky Markey Cancer Center in Lexington, Kent. - What are your clinical/research interests?
Immunonutrition in cancer patients, microvascular free tissue transfer, resident burnout. - What aspect of your time at UAB do you believe was most valuable as you started your career?
All of it. When entering fellowship, I felt that I was better prepared than some of my counterparts because of the autonomy, responsibility, and communication that I learned during my time at UAB. - Did you have a particular mentor while at UAB?
Several - but mainly Bill Carroll and Eben Rosenthal. - What is one of your fondest memories from UAB?
Going into the OR on a Saturday to film "Flap You" with all the residents. - Give one piece of advice you'd like to share with the current residents or those recently graduated.
When you become an attending, you will understand. Don’t get frustrated. - When you're not working, how do you spend your time?
Movies, hiking, traveling, eating all kinds of food, following the Michigan Wolverines
2018 Match Day
The Department of Otolaryngology is excited to welcome our new interns to UAB. We matched with our four residents in one of our highest-ranked classes ever! Meet our new PGY-1 team:




FREE Oral, Head and Neck Cancer Screening
Informational Flyer
WHAT: Free oral, head and neck cancer screening
WHERE: UAB Kirklin Clinic, Otolaryngology 5th Floor Clinic; 2000 6th Ave S.
WHEN: Friday, April 13th 1-4 p.m.
Oral, head and neck cancers refer to many types of cancers, including those that arise in the nasal cavity, sinuses, lips, mouth, thyroid glands, salivary glands, throat or larynx (voice box). In 2018, it is estimated that there will be more than 650,000 new cases of oral, head and neck cancers world-wide, and unfortunately, many individuals will not be aware of their cancer until it has reached an advanced stage. Oral, head and neck cancers now ranked in the top six cancers worldwide.
Most oral cancers arise on the lips, tongue or the floor of the mouth. They also may occur inside your cheeks, on your gums or on the roof of your mouth. Oropharyngeal cancers related to HPV are often found in the tonsil or base of tongue. Other head and neck cancers arise from the voice box or throat, or from salivary (spit) glands or the thyroid gland.
Some early signs and symptoms include:
• A red or white spot in your mouth that doesn't heal or that increases in size
• Sore throat or swollen tonsil
• Changes in your voice
• A lump in your neck
• Earache
• Difficulty swallowing
Tobacco (including smokeless tobacco) and alcohol use are very high risk factors for oral, head and neck cancers, particularly those of the tongue, mouth, throat and voice box. People who use both tobacco and alcohol are at greater risk for developing these cancers than people who use either tobacco or alcohol alone.
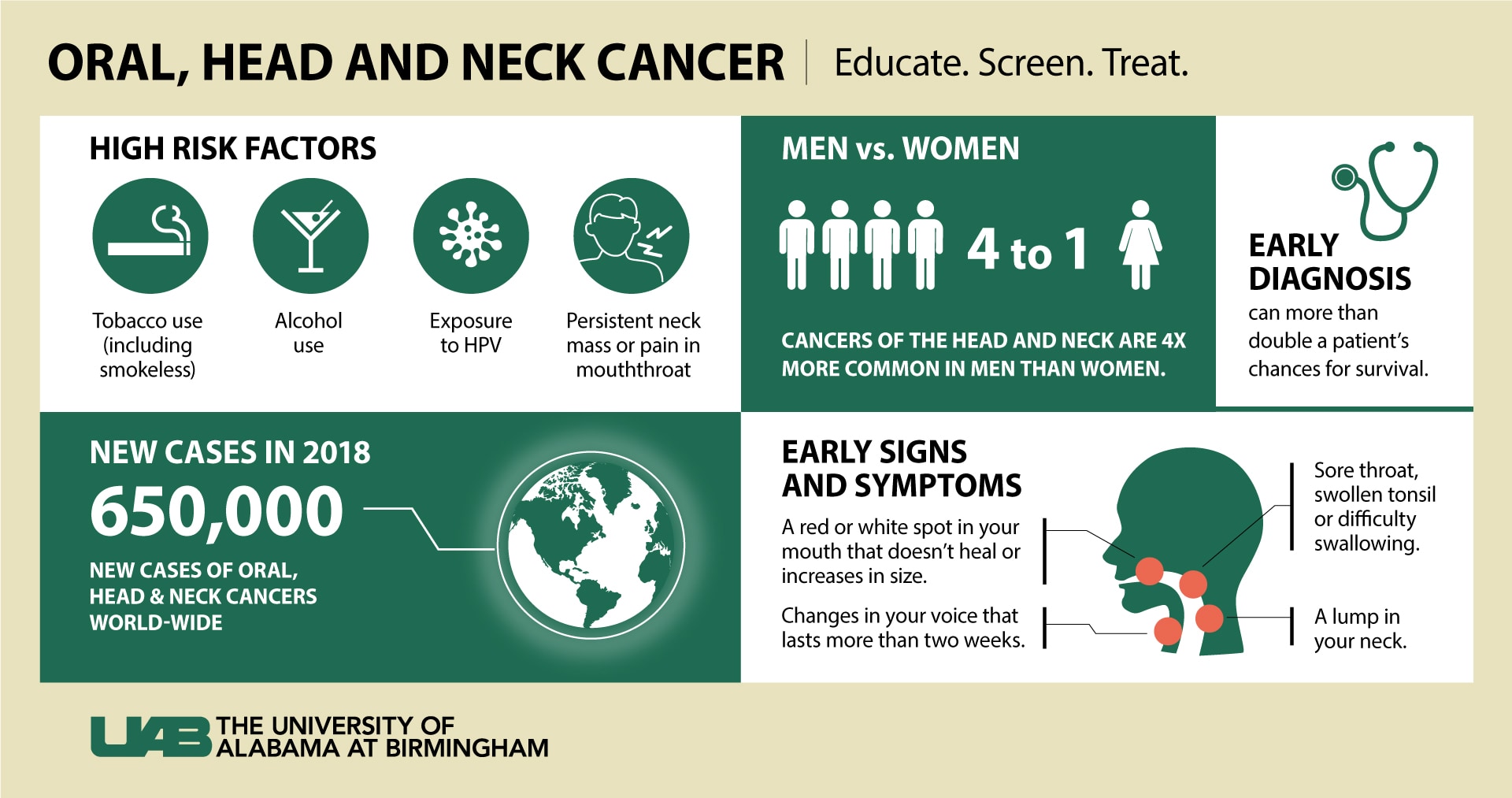
Sources: National Cancer Institute, Head and Neck Cancer Alliance