Putting Preparedness to the Test
By Dale Short and Emily Delzell
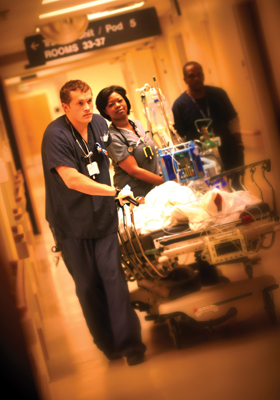 |
UAB's Department of Emergency Medicine operates two EDs at UAB Hospital and UAB Highlands. |
Expect the unexpected. That’s the challenge—and the goal—for everyone working in the field of emergency preparedness.
A quick review of news headlines in recent months highlights a variety of unanticipated dangers: highly destructive tornadoes, an oil-rig explosion, earthquakes, a nuclear accident, and a mass shooting. Influenza outbreaks and a large-scale bioterrorist release of smallpox or anthrax also lie within the realm of possibility. Then there is the day-to-day reality of delivering emergency care that is, at its most fundamental level, about dealing with unplanned, life-threatening situations.
As a leading medical center, UAB plays a crucial role any time a disaster strikes in the state or region. Preparing an effective response requires a blend of skill, science, meticulous planning, and coordinated action.
Emergency Central
Ground zero for emergency preparedness is the UAB Department of Emergency Medicine. UAB is Alabama’s only American College of Surgeons-accredited adult level 1 trauma center, meaning its physicians and nurses are trained and equipped with the technical resources to deliver the highest level of care to the sickest and most severely injured patients.
|
Tornado Outbreak: April 2011 After multiple tornadoes pounded Alabama on April 27, it was “busy, controlled chaos” in UAB Hospital’s ED, says Loring Rue, M.D., chief of trauma, burns, and surgical critical care. Many of the 134 patients treated had injuries consistent with high-speed motor vehicle accidents, Rue notes. To handle the influx, the hospital created an auxiliary ICU with 14 additional beds and postponed elective surgeries. The wounded patients came from Anniston, Cullman, Tuscaloosa, and the Birmingham area, and Rue credits the BREMSS Trauma Communications Center and regional field paramedics for safely triaging and transporting them to the hospital despite the massive devastation. “It has been a team effort,” Rue says of the physicians, nurses, and staff responding to the disaster. |
Approximately 80,000 people will come through the Department of Emergency Medicine this year. With that kind of volume, UAB Hospital’s Emergency Department (ED) is always a hive of activity with exam rooms and beds filled almost to capacity. Its medical personnel provide 24-hour acute medical and surgical services, including specialty care for trauma and burns, spinal cord injury, chest pain, and stroke. They also help uninsured patients who need treatment they would otherwise get from a primary care physician. Detailed planning is necessary to ensure that the department’s resources aren’t overwhelmed during a natural or manmade disaster.
The first move in a crisis, explains Janyce Sanford, M.D. (resident ‘91), chair of the UAB Department of Emergency Medicine, would be to activate the hospital disaster plan, which initially calls in extra emergency medicine personnel and clears the ED so that medical teams can receive large numbers of wounded people. “We would quickly move all patients in the ED to other areas of the hospital so that our beds would be open for victims,” she says. “We would set up a triage center outside the ED with tents and flags indicating injury severity, and physicians would be tasked with assessing incoming casualties—deciding, for example, who needs to go straight to an operating room (OR), who needs more evaluation in the ED, and who needs immediate admission to the hospital.”
Gustav and Katrina: 2008 and 2005
It’s a call that Laura Lee Demmons, R.N., M.B.A., will never forget. Hurricane Gustav, had come ashore, and a neonatal intensive care unit in New Orleans had to be evacuated. “We were told to come because they feared their hospital would be flooded and the babies would die,” recalls Demmons, director of the UAB Critical Care Transport (CCT) service.
Along with mobile intensive care units, the CCT fleet includes a state-of-the-art Cessna Citation Bravo jet custom-equipped for critically ill patients, which was making the circuit between New Orleans and Birmingham before the day was over. Though the jet’s official capacity is two beds, one of the flights carried eight babies.
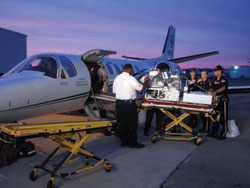 |
UAB Critical Care Transport tends to a patient from a New Orleans neonatal intensive care unit following Hurricane Gustav in 2008. |
“We were really pushing the envelope,” says Demmons of the modifications made to the Bravo so that it could evacuate more tiny patients. “We made it work for an extraordinary disaster situation, but it’s not something we would ever want to do again.”
Three years earlier—nearly to the day—CCT was among the first medical evacuation units to arrive in New Orleans after Hurricane Katrina flooded the city. In a letter published in UAB Synopsis, a UAB registered nurse who was part of the evacuation team sent to Oschner Medical Center described seeing destruction, water, uncontrolled fires, looters, and police and emergency personnel from the air. Oschner’s heliport was underwater, so the team, flying in a helicopter to ferry patients to the airport, landed on a parking deck. The Oschner unit staff had set up a makeshift nursery and was “overjoyed” that help had arrived. They were even more excited that CCT had the resources to transport multiple patients—and then come back for more.
CCT evacuated five infants and two adults within 48 hours of Katrina’s passing, eventually bringing out a total of 21 patients. On subsequent trips, CCT, which has transported more than 37,000 patients in its 28-year history, brought food, water, clothes, and medical supplies to hospital personnel working under extreme conditions without power, water, or reliable communication with the outside world.
Back in Birmingham, Sanford says, UAB medical teams worked alongside doctors and nurses from other area hospitals at Birmingham’s Air National Guard hangar, quickly assessing injuries and deciding which facility—a level 1, 2, or 3 trauma center or a community hospital—was the most appropriate destination for the 98 patients from New Orleans. Medical personnel triaged patients to injury-related color-coded tarps and had them en route to area hospitals within 45 minutes of aircraft arrival.
All-Hazards Approach
Sarah Nafziger, M.D. ’99, associate professor of emergency medicine, says that Hurricane Katrina helped reshape UAB’s approach to emergency services. “We learned that there’s just no way to plan for every kind of disaster,” she says. “We still train for tornados and other specific events, but we’ve moved away from the idea of trying to anticipate each possible hazard. Now we take more of an ‘all-hazards’ approach, which has two basic elements: communications and redundancy in supply lines.”
Thinking of a disaster in terms of the number of ambulances required is limiting, and a broader focus is important, Nafziger says. “Medicine is the most urgent piece of the puzzle, but it’s far from the only one. We must consider food, water, gasoline, shelter. So many other factors complicate things.”
Communication is undoubtedly one of the most vital parts of an effective emergency response system, says Loring Rue III, M.D. (resident ’88), the John H. Blue Chair of General Surgery; chief of the Section of Trauma, Burns, and Surgical Critical Care; and director of the Center for Injury Sciences.
“Studies have shown that about 20 percent of trauma deaths are potentially preventable and that the most frequent cause of these deaths is a delay in getting the right kind of care,” he says.
“The most important innovation in caring for trauma patients within a system involving multiple hospitals with a range of medical capabilities is a concept we call ‘right patient, right place, right time, right care,’” Rue says. “Alabama is fortunate to have a system that matches hospital resources with the needs of individual patients.”
F-5 Tornado: April 1998
In 1998, the Birmingham Regional Emergency Medical Services System (BREMSS), the trauma system that today coordinates emergency response in five of Alabama’s six designated trauma regions, was less than two years old.
On April 8, a tornado cut a 17-mile swath of devastation through Jefferson and St. Clair counties. Thirty people died on the scene, and another 224 suffered injuries requiring hospital treatment.
 |
The BREMSS Trauma Communications Center matches patient needs with hospital resources across most of Alabama. |
UAB provides medical direction to BREMSS, which uses a software program called LifeTrac to poll trauma centers and assess their available resources in real time. The system allows BREMSS to route each patient to the facility best equipped to treat his or her injuries.
Then—and now—the BREMSS Trauma Communications Center (TCC) enables this matching of patients with hospital resources and capabilities. “During the tornado, the TCC, which for a time after the storm was our only means of communication, helped emergency responders make sure the most severely injured patients went to level 1 centers like UAB, and that people with less serious injuries were seen at other hospitals,” Rue says. “This kept any one hospital from becoming overwhelmed with patients and probably saved lives.”
Of the more than 200 people seen at hospitals after the 1998 tornado, only two died: Both had been correctly routed to level 1 trauma centers and were receiving the most advanced care available.
“The system worked as it was designed to,” says Rue. Today, BREMSS is critical to making “right patient, right place, right time, right care” happen. “Having most of the state networked into a central system means that during a major disaster, patients are sent where they need to go,” Rue explains. “Centers that can take care of the sickest or most injured patients aren’t inundated with people who could be treated effectively elsewhere.”
Resources for Response
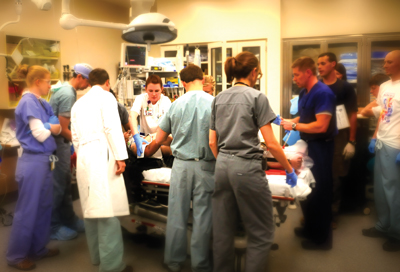 |
UAB Hospital's ED is designed to faciliate triage and patient flow, with 45 treatment rooms divided into five care areas. |
BREMSS serves as a model for other states that need to improve their trauma care, says Rue. “It’s an effective system, but it’s not cheap. Neither is maintaining a level 1 trauma center like UAB.
“There are huge resource requirements associated with the level of care we provide. UAB has board-certified faculty surgeons who sleep in the hospital so they can be ready to provide care every hour of the day, every day of the year. That preparation saves lives,” says Rue.
He notes that quick transport to a level 1 trauma center played a vital role in saving the life of U.S. Representative Gabrielle Giffords, who was shot through the brain in January during a gunman’s rampage in Arizona in which six people died. “She was in an OR with a team of neurosurgeons within a half an hour of the shooting,” Rue says. “A smaller hospital simply doesn’t have that kind of expertise standing by, and delays in care can mean the patient doesn’t survive.”
Sanford, who hopes she never has to be proved right, says, “If we were to have a mass shooting like the one in Arizona, I’m confident our ED could handle it well. We have an expert on call for nearly every medical specialty. We’re very fortunate to have an exceptional trauma system such as the one set up by people like Loring Rue and BREMSS Director Joe Acker, and we’re lucky to have a trauma center like UAB that’s prepared to respond to whatever comes. We’re ready to serve 24 hours a day, seven days a week, 365 days a year.”
