 “Studies have shown that being screened annually results in more lives saved from breast cancer than screening every other year.” Breast cancer is the most common cancer in women in the United States, according to the Centers for Disease Control and Prevention. That is why having an annual mammogram beginning at age 40 is the best way to prevent deaths from breast cancer.
“Studies have shown that being screened annually results in more lives saved from breast cancer than screening every other year.” Breast cancer is the most common cancer in women in the United States, according to the Centers for Disease Control and Prevention. That is why having an annual mammogram beginning at age 40 is the best way to prevent deaths from breast cancer.
Breast imagers at the University of Alabama at Birmingham School of Medicine explain when and why women should have mammograms, what having a mammogram feels like, and the risk factors women should be aware of when it comes to breast cancer.
When should women get mammograms?
“All women with no special risk factors should start having annual mammograms at age 40,” said Caroline Reich, M.D., Ph.D., breast imaging medical director in the Department of Radiology at UAB. “About 20 percent of the cancers found in asymptomatic women are in individuals between the ages of 40 and 49. To me, this is one of the biggest reasons to start having mammograms at 40.”
Reich adds that the cancers found in premenopausal women tend to be more aggressive than those found in postmenopausal women.
“Studies have shown an increase in breast cancer incidence in women at and beyond the age of 40 with statistically significant reduction in mortality among those women screened starting at age 40,” said Lawrence Manalo, M.D., Ph.D., a breast imager at UAB.
Why should women have annual mammograms? Why not every other year?
“The benefits of a yearly screening mammogram far outweigh the risks,” Manalo said. “Detecting cancer while it is small and hasn’t had a chance to spread and getting treated appropriately significantly improve a woman’s mortality.”
| While a family history of breast cancer plays a role in the risk, it does not mean you are in the clear if you do not have a history of the disease. |
Manalo adds that most breast cancers are sporadic and are detected in women of average risk, including women with no family history of breast cancer.
The largest and longest-running breast cancer screening trials in history have reconfirmed that regular mammography screening cuts breast cancer deaths by roughly one-third of all women age 40 and over, according to the American College of Radiology and the Society of Breast Imaging.
“Annual mammography screening saves lives,” Reich said. “Studies have shown that being screened annually results in more lives saved from breast cancer than screening every other year.”
Why are some women reluctant to have mammograms?
One reason some women may avoid having mammograms is the fear that it will hurt from the compression.
“I think patients worry about discomfort and are scared of the compression, especially those women who have never experienced a mammogram before,” Reich said. “However, with every generation of new technology, adjustments are being made to make patients more comfortable and make the procedure less intimidating. New technology has enhanced the design of mammography machines to minimize discomfort and make the screening faster.”
“It is important to educate women that having their breasts compressed appropriately aids in cancer detection due to less overlap or superimposed normal breast tissue that can hide cancers,” Manalo said.
Reich says exposure to radiation is another concern she hears from her patients.
“There is a perception that you will be exposed to a high amount of radiation, but that is not the case,” Reich explained. “The amount of radiation a woman receives during a screening mammogram is the equivalent to what they receive from background radiation walking around for a seven-week period. The benefits of early detection far outweigh the risks of such a small amount of radiation.”
Anxiety about finding a cancer is also a factor that may deter women from annual screenings.
“Anxiety, especially in women with a history of breast cancer or a family history, can be overwhelming for patients,” said Stefanie Woodard, M.D., a breast imager at UAB. “Our technologists are excellent at comforting patients during their exams. We want patients to feel confident and supported when they come for their screenings.”
What happens during a mammogram?
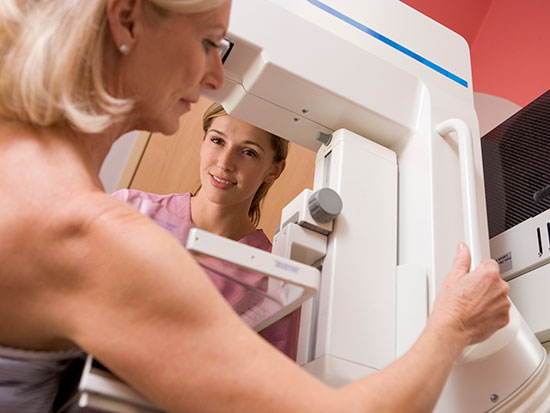
During a mammogram, a technologist will walk you through the process, then assist you throughout the screening by positioning your breast for each image.
“We take anywhere from four to six images of the breast,” said Tricia Reed, a mammography technologist at UAB. “There will be some compression, but it is not as bad as what patients typically expect.”
As for the compression, Reed says the purpose is to take the best image of the breast tissue. Each compression lasts for about10 seconds per image.
“The tighter the compression, the better images we can get from you so the doctor can see more tissue,” Reed explained. “The breast is made up of fibroglandular and fatty tissue, and if we don’t spread it out, you can’t see clearly through the tissue.”
The technologists will take images of the breasts from top to bottom, the sides and the lymph nodes.
“A lot of people don’t realize that your breast tissue goes under your arm,” said Kernesha Weatherly, manager of Breast Imaging at UAB. “This image gives us the best picture of the lymph nodes and muscle tissue where cancers may be found.”
Patients who are active portal members will receive the results within 24 hours of their images’ being read.
What does it mean if I receive a breast density notification?
Alabama has a breast density notification law, meaning health care providers are required by law to tell patients if 50 percent or more of their breast tissue is dense.
“A lot of people become nervous when they hear they have dense tissue,” Weatherly explained. “The notification does not mean there is a problem. It is only because it is a state requirement.”
However, dense breast tissue may make it harder to find cancer on a mammogram, which is why women with dense breasts may benefit from digital breast tomosynthesis or semi-3D mammography in addition to clinical breast examinations.
Who is more at risk for breast cancer?
Simply being a woman is the main risk factor for breast cancer, according to the American Cancer Society. Men can get breast cancer too, but the disease is about 100 times more common in women than in men.
While a family history of breast cancer plays a role in the risk, it does not mean you are in the clear if you do not have a history of the disease.
“The majority of women who get breast cancer do not have a family history,” Reich said. “However, people with a family history have a greater chance of developing breast cancer, particularly if someone has a mother or a sister who developed pre-menopausal breast cancer.”
If you do have an immediate family history of the disease, meaning a mother or a sister has had breast cancer, particularly at an early age, Reich suggests that you discuss this with your doctor to see if you should begin screening before age 40.
How can I schedule a mammogram at UAB?
To schedule a mammogram, contact the UAB HealthFinder line at 800-822-8816. You may also request an appoint online.
UAB offers mammography screening at The Kirklin Clinic and at UAB Medicine Leeds. Breast imaging will also be offered at UAB’s Gardendale clinic once it opens next year.