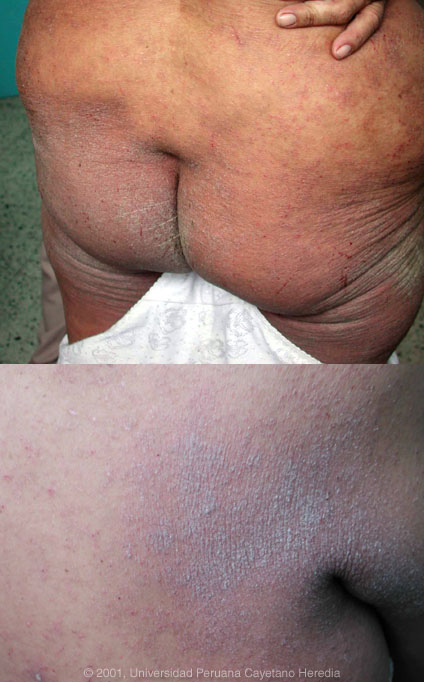
| Discussion: Skin scrapings viewed by direct microscopy disclosed 2-3 Sarcoptes scabei per each high power field, a remarkable density. ELISA and Western blot for HTLV-1 were both positive in the patient as well as in both her parents who are in their 70s.
The crusted diffuse highly pruritic skin lesions in this patient are very characteristic for Norwegian scabies. This condition is well described in many immunocompromising conditions including HIV infection, malignancy, and immunosuppressive therapy. The skin is hyperinfested with thousands of mites, so it is easily diagnosable with simple scrapings. The lesions are highly infectious and present a serious nosocomial risk.
At the Tropical Medicine Institute in Lima approximately 70% of all cases of Norwegian scabies are associated with HTLV-1 infection and are, in the absence of any other factors, associated with immunosuppression. Other opportunists associated with HTLV-1 are strongyloides infection (negative Baermann stool concentration in our patient) and onychomycosis.
Other conditions associated with HTLV-1 infection are acute T-cell leukemia/lymphoma (normal blood film in this patient) and autoimmune disease including tropical spastic paraparesis, Sjogrens, and thyroiditis. Neither this patient nor her parents had any neurological findings.
The prevalence of HTLV-1 in South America is generally underappreciated, normally being associated with Japanese and Caribbean populations. In Peru, the disease is highly endemic (2-3% seropositivity) in Andean areas of the country, in Quechua populations who have had no contact with Japanese immigrants to the country. Other South American countries with significant rates of HTLV-1 include Brazil, Colombia, and Ecuador. Transmission appears to be mainly vertical with high associations with breastfeeding and duration of breastfeeding (probable route in our patient). Transfusion, sexual transmission, and IV drug abuse are much less important.
Norwegian scabies is not responsive to normal topical agents such as benzyl benzoate or permethrin. Our patient was treated with ivermectin 200 micrograms/kg bid for 2 days which was repeated 15 days later. The lesions responded dramatically to therapy.
|