 |
Gorgas Case 2003-12 |
 |
|
The Gorgas Courses are now finished for 2003. Please find below the 12th and final Gorgas Course Case of the Week for this year. The patient was seen by the Gorgas Course participants in the outpatient department of the Tropical Medicine Institute. We thank Drs. Alejandro Busselau and Angélica Terashima for advice on this case.
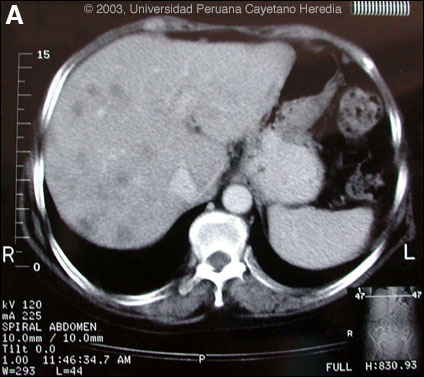
 History: Previously very healthy 62-year-old female with 3 months of fever, severe general malaise, loss of appetite, 10 kg weight loss, right upper quadrant pain and initially some icterus. On no regular medication. Evaluation at an outside hospital 1 month earlier had shown an absolute eosinophil count of 7,500, alkaline phosphatase 8X normal, transaminases twice normal, and 3 negative stool concentrations for O & P. Chest X-ray was normal and an abdominal ultrasound showed numerous small (<15 mm) lesions throughout the liver. She was treated empirically with 7 days of praziquantel without effect. No significant past medical history.
Epidemiology: Farmer from just outside Lima. Her husband, who had a history of chronic alcoholic liver disease, had become ill at the same time and died with icterus, ascites, and hypereosinophilia. Just prior to the illness the husband had heard of beneficial health effects of watercress (called berros in Perú) and she had bought a large amount of it, which was consumed on only one occasion. Physical Examination: Pale. Afebrile. Liver non-tender 3 cm below costal margin. No splenomegaly. Laboratory Examination: Hematocrit 31. WBC 15,600 with 21 neutrophils, 18, lymphs and 56 eosinophils. Blood cultures negative. Liver function not repeated. Hepatitis A, B, C, serology negative. Stool O & P and serological tests were ordered. Available CT image [Image A] is from 3 months later but is representative of findings throughout the illness.
|
|
Diagnosis: Massive infection with Fasciola hepatica.
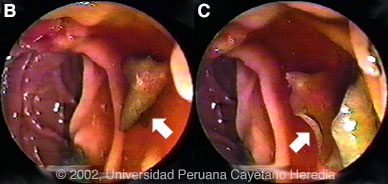
 Discussion: 2 of 6 stool concentrates showed scanty eggs of Fasciola hepatica. Arc-2 immunoelectrophoresis and western blot were both positive for Fasciola hepatica. Fasciola hepatica is a trematode (fluke or flatworm) in which the adults inhabit the large biliary ducts. The adults are from 1 to 3 cm long and attach to the biliary epithelium by a single ventral sucker [see Images B, C from our files for endoscopic view of an adult in the common bile duct]. In the absence of direct visualization, characteristic eggs can be seen on stool examination but more often, especially in the early migratory phases of infection, as should have been done at the referring hospital, specific serology must be obtained. As with all other trematodes, Fasciola hepatica requires a snail intermediate host. Eggs produced by the hermaphroditic adults pass with the feces and hatch, releasing larvae in fresh water. After passing through a snail, mature cercariae emerge and rapidly encyst on various kinds of aquatic vegetation such as watercress. After ingestion by a human or animal definitive host, the metacercariae excyst in the duodenum and larvae pentetrate the intestinal wall and subsequently migrate directly into the liver via Glisson's capsule. The larvae then migrate through the hepatic parenchyma for 3 to 4 months until they reach large biliary ducts where they mature to adults. The distribution of Fasciola hepatica is cosmopolitan, but is by far the most common in sheep-raising areas where these herbivores are common definitive hosts. Heavily infected sheep develop "sheep liver rot". Other important definitive hosts are goats, cattle, horses, llamas, vicunas, and camels. The contiguous altiplano regions of the Peruvian and Bolivian Andes are highly endemic, with human prevalence rates of as high as 67% in some villages. Egypt, Cuba, and Northern Iran are also highly endemic. Cooking, which would kill the metacercariae, dramatically changes the flavor of watercress and the population is reluctant to adopt this simple measure. Clinically, the disease can be divided into acute and chronic phases. In the acute phase, migrating larvae cause inflammation and necrosis of hepatic parenchyma during the 3 to 4 months it takes to reach the large biliary ducts. High fever, eosinophilia, right upper quadrant pain and especially significant anorexia, vomiting and weight loss of 20 kg or more may develop, which usually abates when the larvae mature to adults. The adult flukes in the biliary tree are generally asymptomatic but some patients develop chronic manifestations including right upper quadrant pain, nausea, vomiting, and hepatomegaly. Eosinophilia and abnormal liver function may develop but are less common than with acute disease. Adult flukes may cause hyperplasia, desquamation, thickening, and dilatation of the bile ducts. Malignant degeneration and cholangiocarcinoma such as results from chronic infection with the oriental liver fluke Clonorchis sinensis has not been reported with Fasciola hepatica. The differential diagnosis of hypereosinophilia with accompanying destructive hepatic lesions is limited. Toxocariasis causes hypereosinophilia with hepatomegaly but the pathology results from small granulomas around individual non-migrating larvae and not the large destructive tracks as was seen on the CT in our patient. Only case reports but no series of sequential CT scans of the acute phase of fascioliasis have been published. Lesions are irregular, hypodense, sometimes oblong and branching. One recent published case shows serial CT scans over a 9-month period demonstrating changes in position, and shape of lesions over time, as would be consistent with the destructive nature of the migrating flukes [N Engl J Med. 2002 Apr 18;346(16):1232-9]. Fasciola hepatica is the only trematode infection for which praziquantel is not the drug of choice. WHO has put the veterinary anthelmintic triclabendazole (Novartis) on its essential drugs list and has declared it the drug of choice despite the fact that human preparations are registered in only 2 countries. In Perú, the veterinary preparation is readily available and used. In the U.S. and many other countries the veterinary preparation can be obtained by special release from the manufacturer. The usual dosage is 10 mg/kg with a meal. Many practitioners repeat the dosage 12 to 24 hours later. In our institute the cure rate is 96% (A. Terashima, unpublished). Our patient was treated with a single 2-day cycle of triclabendazole with symptomatic improvement and a weight gain of 10 kg. Eight subsequent stool examinations were negative. Three months after treatment, the patient required hysterectomy for uterine fibromas and liver biopsy performed at that time due to the persistent CT abnormalities showed residual microabscesses with PMN infiltration, fibrotic granulomatous reaction but no parasites or eosinophilic infiltrate. Peripheral absolute eosinophil count at that time was 780. A final CT examination 6 weeks post-operatively [not shown] now shows significant reduction in the number of lesions. The earlier case report [N Engl J Med. 2002 Apr 18;346(16):1232-9] had followed sequential lesions over 9 months prior to any treatment. We demonstrate that in a case of massive fascioliasis such as here, the destructive inflammatory tracks made by migrating larvae persist radiologically and histologically for months even after apparent parasitic cure. In addition, the patient’s husband, due to his underlying chronic liver disease, almost certainly died of massive fasciola infection and this degreee of infection in both husband and wife was after a single exposure to contaminated watercress.
|