 |
Gorgas Case 2023-07 |
 |
|
The following patient was seen as an inpatient in the Tropical Medicine ward of Cayetano Heredia Hospital in Lima by the 2023 Gorgas Course participants.
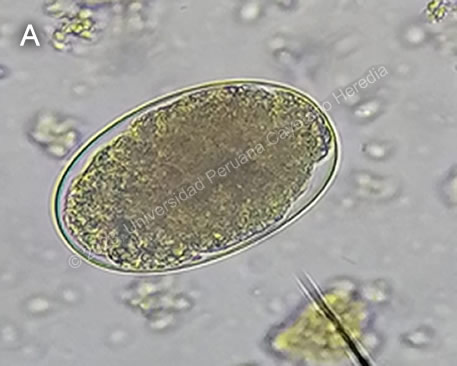 History: A 22-year-old previously healthy male patient presented with a 3-month history starting with mild dyspnea on exertion and fatigue. The dyspnea and fatigue worsened in the following weeks; two weeks before admission he stopped working due to the dyspnea. Ten days before admission, he had an episode of mesogastric pain which subsided using natural medicine. On the day of admission, he had nausea and one episode of vomiting, accompanied with fever, dizziness, and headache. Epidemiology: Born and lives in Yurimaguas, Loreto, in the Amazon Basin. Traveled from Loreto to Lima three weeks before admission. Works as a carpenter. Drinks alcohol once a month, smokes four cigarettes per day, has used cocaine paste in the past. Past medical history: No other illnesses, no past surgeries. Laboratory: Hemoglobin 2.6 mg/dL (MCV 80.3, MCH 23.6), hematocrit 10, WBC 16 190 (neutrophils 10 900, eosinophils 2 580, basophils 50, monocytes 750, lymphocytes 2 280), platelets 300 000. Ferritin 3 ng/mL (21.8-274.6), vitamin B12 198 pg/mL (normal 187-883), folic acid 4.6 ng/mL (normal 3.1-20.5). PT 13, aPTT 30, INR 0.98. Glucose 77, urea 23, creatinine 0.83, Na 137, K 4.8, Cl 95. AST 30, ALT 28, LDH 166, Alk Phos 122, GGT 22. HIV, RPR HBsAg non-reactive. Thick and thin smear were negative. AFB in sputum was negative x3. PPD was 0mm. Stool O&P is shown in Image A.
|
|
Diagnosis: Severe anemia secondary to hookworm infection. 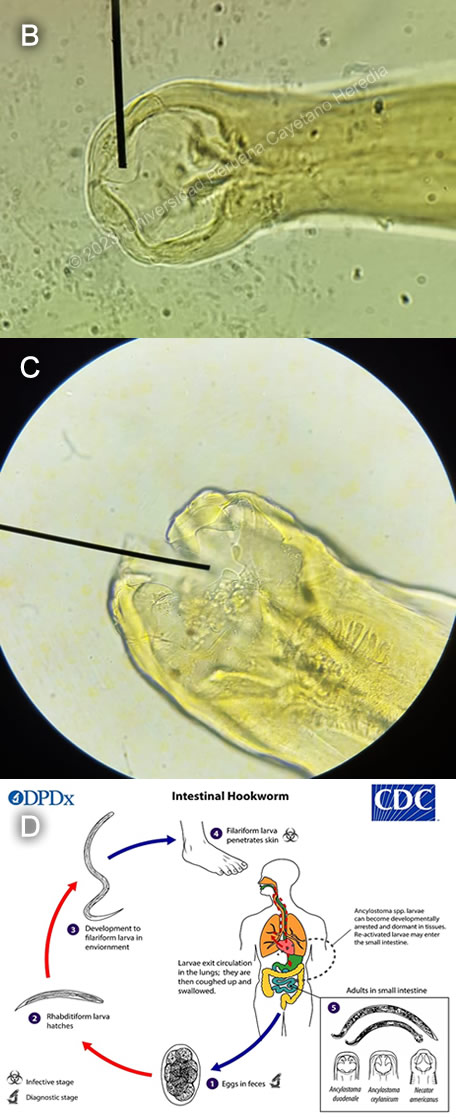
 Discussion: The stool O&P exam revealed hookworm eggs, Baermann was negative for Strongyloides. It is not possible to differentiate Necator americanus from Ancylostoma duodenale from examination of the eggs. The sample was cultured, and examination of the adult roundworm revealed the etiologic agent for our patient’s anemia to be Necator americanus (Image B), with characteristic ventral plates in the buccal capsule in contrast to the teeth that can be seen in Ancylostoma duodenale (Image C). Upon further questioning, the patient confirmed he regularly walked barefoot in the jungle when searching for timber. This patient likely had a very chronic infection with hookworms with a slow decline in hemoglobin levels over years, which only became symptomatic in the months before admission. |