Research & Innovation
UAB researchers are advancing cancer prevention and treatment through lifestyle-based survivorship care, adaptive molecular therapies and precision biomedical engineering.
This rare brain condition causes a person’s hand to move without intention or control.
New research from UAB shows a structured expert panel approach can accurately and reliably measure delirium severity in patients with and without Alzheimer’s disease and related dementias.
UAB has been a national leader in Fabry disease care and research for more than two decades.
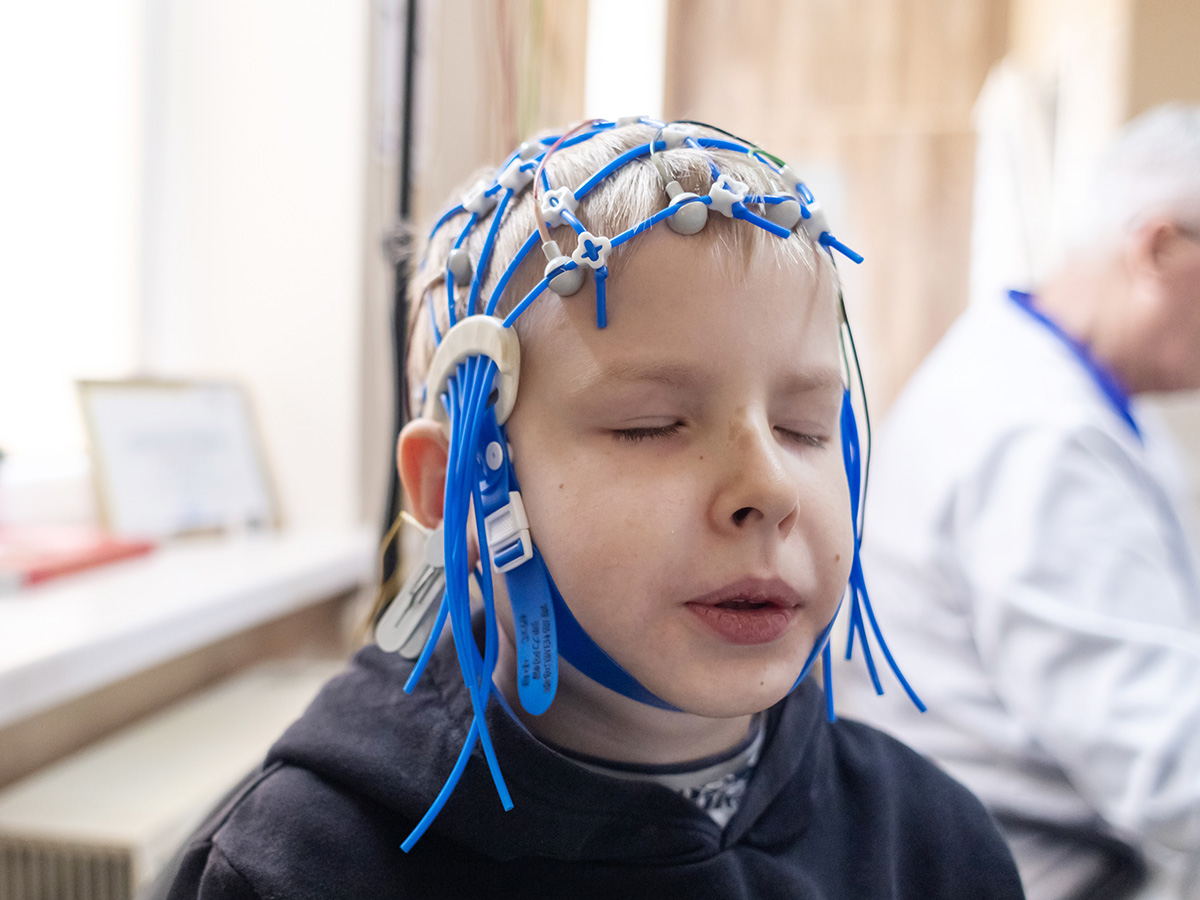
The study is aimed to track early brain and child development in the United States by following pregnant participants and their children for approximately 10 years.
UAB researchers are developing a new at-home cervical cancer screening device aimed at increasing access to screening and improving early detection.
Scientists identify an immune switch, NFAT, that is crucial to successful pregnancies, offering new insights on the causes of preeclampsia, implantation problems and inadequate blood supply.
UAB scientists discovered an oral drug stopped weight rebound after discontinuation or cessation of GLP‑1 treatment in preclinical studies, opening the door to a new approach for maintaining weight loss.
The MajesTEC-3 clinical trial shows that using a new two-drug immunotherapy regimen can lead to long-lasting remission for patients with multiple myeloma. Over 83 percent of patients enrolled in the trial are alive and progression-free three years after therapy.
The study will enroll 240 adults with HIV and insomnia, randomly assigning them to one of two treatments to evaluate how each approach affects sleep and cognitive health.
Since March 2022, UAB and McMaster University have advanced a shared vision to strengthen institutional collaboration across research, education and global health initiatives.
In a study published in the New England Journal of Medicine, long-acting injectables proved to be a more effective treatment in maintaining consistent administration for those living with HIV and facing barriers to taking daily oral medications.
Patients at the amputee clinic can receive prothesis sockets faster with the new 3D printer.
As UAB researchers continue to study how these drugs work and what comes next, their findings are helping move the conversation beyond hype, while working toward a clearer understanding of one of the most significant medical breakthroughs of the past decade.
Obstructive hypertrophic cardiomyopathy is a leading cause of heart-related disability in younger adults and the most common cause of sudden death in young athletes.
The BREATHE-3 trial is a pioneering phase 3 pivotal clinical study investigating the impact of a novel, experimental device designed to open the airways within a patient’s lungs and release trapped air in patients battling severe emphysema and COPD.
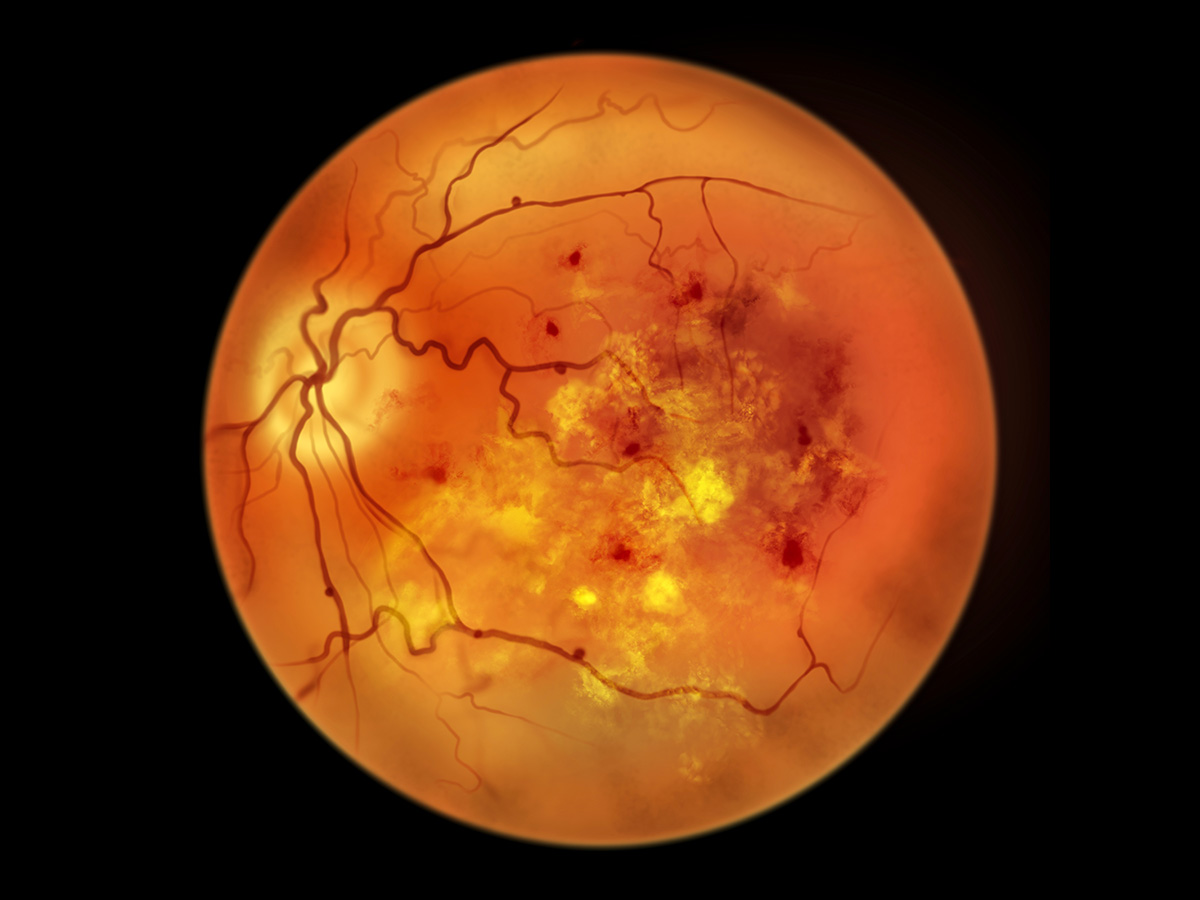
Research published in the journal Gut suggests that nutraceutical strategies restoring tryptophan metabolism and IPA levels may serve as both biomarkers and therapeutic approaches for diabetic retinopathy.
Procedures that remove plaque from a narrowed carotid artery in the neck or prop the artery open with a stent did not appear to be better at improving cognitive function than medications and lifestyle changes.
Veterans who experienced homelessness and received care in H-PACTs were more likely to consistently see the same primary care provider.
IncRNAs act like “switches,” turning off functionality for more than 3,000 genes that are essential for healthy brain functioning.
UAB researchers share a discovery that could pave the way for non‑addictive alternatives to opioid painkillers amid an era of rising overdose deaths.
The clinical trial represents a major step forward in finding new solutions for people living with treatment-resistant depression.
UAB researchers discovered that multiple myeloma is more common in men than in women through the Integrative Molecular and Genetic Epidemiology study.
A new UAB study could help doctors better understand a chronic pain-causing condition associated with diabetes mellitus and ultimately improve pain relief treatment options for diabetic patients.
UAB researchers found that specific bacteria are believed to provoke inflammation that characterizes diseases such as Crohn’s disease.
Researchers at UAB recently received a grant to help develop a plan aimed at reducing crash fatality in Central Alabama through evidence-based enhancements.
Multisite research, including research at UAB, shows that oral semaglutide is nearly as effective as the widely used injectable version for treating obesity, delivering about 13.7 percent average weight loss over 64 weeks.
In partnership with the Housing Authority of the Birmingham District, the City of Birmingham and community partners, UAB will assess the effectiveness of public housing renovations and environmental refinements on community health.
Sedative choice could improve patient outcomes in patients who have been intubated.
A new study reveals how a bacterial gene and FIVAR-equipped proteins allow pneumonia bacteria to invade heart cells, causing severe cardiac damage.