The UAB Department of Emergency Medicine is actively involved in emergency and acute care research with a goal of advancing the science and practice of acute care. Our department actively partners with agencies such as the Centers for Disease Control and Prevention, the National Institutes of Health, the Alabama Department of Public Health, and the U.S. Food and Drug Administration, and we currently have two faculty members listed on the Principal Investigators list in the Blue Ridge Rankings.
Areas of Focus
Geriatrics
Geriatric Emergency Medicine is dedicated to improving the acute care of older adults in the emergency department.
Medical Toxicology
UAB’s Office of Medical Toxicology’s research is multifaceted including topics on snake envenomation, heavy metal toxicity, critical care toxicology, emerging drugs, and addiction medicine. Our faculty have a wide breadth of experience and interests in treating the poisoned patient.
Population Health
We recognize our unique opportunity and responsibility to improve the health of those within our community, especially among those that may have limited access to care. As such, we have several ongoing projects aimed at this goal. This includes efforts to increase access to breast cancer screening, treatment of substance use disorder, and the diagnosis and treatment of various communicable diseases such as HIV, HCV, and Syphilis.
Resuscitation Science
At UAB, we care for some of the most critically ill patients in our region. Our team is actively engaged in research focused on cardiac arrest, with a particular emphasis on improving early response and increasing bystander CPR rates. We also maintain an active ED ECMO and ECPR program. In addition, through our strong relationship with Critical Care Medicine, we participate in a variety of research initiatives, particularly those centered on airway management.
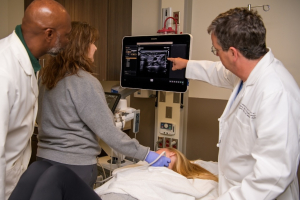
Ultrasound
Emergency Ultrasound in the UAB Department of Emergency Medicine is made up of board-certified experts in Advanced Clinical Ultrasound who strive to advance the understanding of clinical ultrasound through research and dissemination of knowledge on the role of clinical ultrasound in patient care and education.