| 2003 Case #5 |  |
|
| 2003 Case #5 Diagnosis& Discussion |
 |
|
| (Links to Other 2003 Cases are at bottom of this page) | ||
| Diagnosis: Sub-acute brucellosis (due to Brucella melitensis) with multiple concomitant complications. |
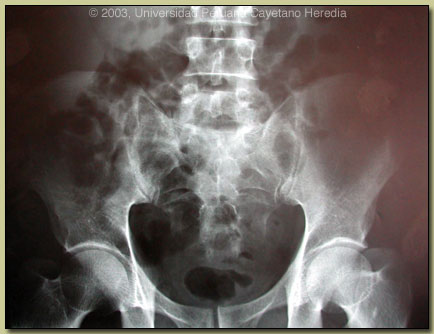
| Discussion: Most patients with brucellosis present with systemic febrile disease with no overt complications. This patient is very illustrative as he nicely illustrates multiple complications all during the course of the same illness. While hepatomegaly and mild elevation of liver enzymes are seen in 50-70% of acute cases, clinically evident hepatitis with jaundice is seen in only 3-6%. While a number of other diseases might have been thought of on the initial presentation of this patient (viral hepatitis, typhoid, leptospirosis, TB; there is no malaria in Lima), brucellosis needs to be always considered. Sacro-illitis is the most common articular manifestation in sub-acute brucellosis although it is usually unilateral (80% of the time). Brucellosis should always be a consideration in a febrile patient with fairly new onset of severe back pain with inability to bear weight. Epididymitis occurs in 3-10% of young male patients so it should be thought of along with STDs and viral diseases.
The diagnosis of Brucella is usually made by serology. In highly endemic areas a slide or tube agglutination test for Brucella is part of the routine initial testing of every febrile patient. The test is cheap, easy to do, and results are available the same day. Blood cultures are expensive, a positive result may take many days, and the sensitivity is only about 70% in Perú (and is lower in most US series) even after 2 sets of blood cultures. Bone marrow cultures are more sensitive (>90%) but are invasive and expensive. In addition, Brucella is a bio-hazard and cultures require biosafety level 3 precautions. The basic agglutination test detects both IgM and IgG antibodies. The addition of 2-mercaptoethanol destroys the binding ability of only the IgM antibody so this test detects the presence only of Brucella specific IgG. With successful treatment IgG antibody does not often persist at any positive level (≥1/80) for more than a year and should start diminishing very soon after treatment. When our patient presented the second time 4 months later with a 2ME titre that was higher than it was initially, this was a presumptive indicator of still active infection. Our patient had been prescribed a standard 6-week course of oral doxycycline and rifampin which in our hands has a success rate in preventing relapse of 90% in uncomplicated disease. However, due to economic constraints the patient completed only 4 weeks. With complicated disease we now plan on treating him for 3 full months with oral doxycycline and rifampin, and he has responded well to the therapy so far. The patient was unaware of any exposure to unpasteurized goat cheese. However, on further questioning of his wife, she relates that she frequently serves it at home. This is a frequent scenario in Perú and most countries at highest risk of brucellosis, with the predominant agent being Brucella melitensis. Brucellosis due to Brucella abortus acquired from cattle is increasingly uncommon in the US and other countries. All travellers with fevers of unknown origin should be queried for a history of goat cheese ingestion. Brucella melitensis is commonest in Mexico, Venezuela, Perú, the Mediterranean countries and several of the Arabic countries of the Middle East.
|