| 2003 Case #9 |  |
|
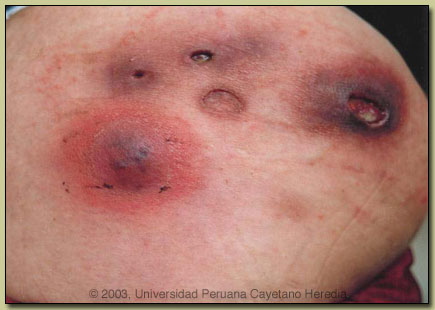
| Diagnosis: Buruli ulcer due to infection with Mycobacterium ulcerans. |
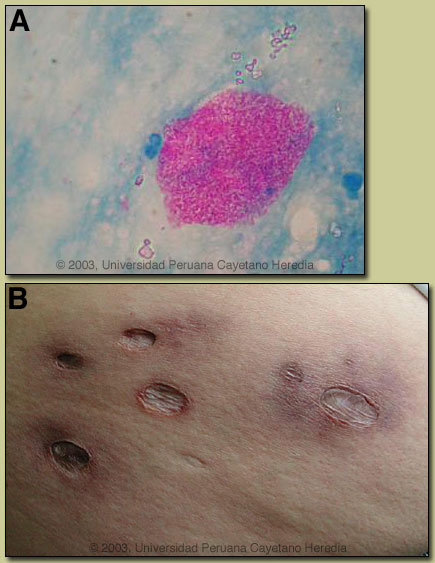 Discussion: Acid-fast stain of purulent material is shown [see image A] and demonstrates AFB extracellularly and in clusters. Histopathology of a badly preserved biopsy specimen showed widespread necrosis of fatty tissue with acid-fast organisms present locally. Material sent for PCR to our collaborator Professor Francoise Portaels at the Tropical Medicine Institute, Antwerp, Belgium was positive for Mycobacterium ulcerans. Culture was contaminated by mold and no mycobacteria were grown. Discussion: Acid-fast stain of purulent material is shown [see image A] and demonstrates AFB extracellularly and in clusters. Histopathology of a badly preserved biopsy specimen showed widespread necrosis of fatty tissue with acid-fast organisms present locally. Material sent for PCR to our collaborator Professor Francoise Portaels at the Tropical Medicine Institute, Antwerp, Belgium was positive for Mycobacterium ulcerans. Culture was contaminated by mold and no mycobacteria were grown.
According to WHO consensus criteria for laboratory diagnosis of Buruli ulcer, any 2 of the following 4 criteria are sufficient: (1) acid-fast bacilli in a stained smear; (2) positive mycobacterial culture (requires 6-8 weeks); (3) positive PCR; (4) typical histopathology in an excisional biopsy. Clinically the disease is divided into ulcerative and non-ulcerative forms and the non-ulcerative forms don?t necessarily progress to ulcerative disease. Non-ulcerative forms present as papules, nodules, plaques, or in a diffuse edematous form with non-pitting swelling. The ulcerative form when fully developed has broadly undermined edges and is indurated peripherally. The ulcer is usually painless unless there is bacterial superinfection. When more than one ulcer is seen they are close together and usually communicate under the intact skin. Contractures may occur as a complication of scarring of lesions occurring over or close to joints. Osteomyelitis may occur due to primary spread or as a metastatic process. The pathogenesis of the disease is thought to relate to inoculation of the organism from the environment into subcutaneous tissues after trauma to contaminated skin sites. There is an association with contact with bodies of water and certain aquatic insects may be involved in the spread. Human to human transmission is thought not to occur. Mycobacterium ulcerans elaborates a toxin called myolactone which has an affinity for fat cells and which causes progressive radial necrosis of subcutaneous tissues and subsequently, but more slowly, the overlying skin breaks down. In tissues, Mycobacterium ulcerans grows primarily as extracellular microcolonies and not as facultative intracellular parasites as do other mycobacteria. Excisional biopsies (punch biopsy should not be used) that sample the full thickness of the skin down to the fascia is required and should be taken from the edge of the skin surrounding an ulcer or from the middle of a papular or nodular lesion. Buruli ulcer occurs in at least 31 countries throughout Africa, Central and South America, Europe, Asia, and Australia, but it is a major public health problem mostly in Africa and in particular West Africa. A survey in Ghana in 1999 found over 6,000 cases and in some communities prevalence rates of 20% or more occur. Dr. Humberto Guerra of our institute, working together with Dr. Portaels, has confirmed at least 5 cases of Buruli ulcer here in Perú and is aware of 2 other confirmed cases. With the lack of a systematic survey the true extent of the problem is unknown. Buruli ulcer is generally an aggressive disease and Mycobacterium ulcerans is not sensitive clinically to any antibiotics or anti-tuberculous drugs. Wide excisional surgery is generally recommended and necessary. Of note is that our 5 cases in Perú have all followed indolent courses and none have required surgery. An image of our patient at 18 months after initial presentation and with only herbal therapy is shown [see image B]. Based on sequencing of PCR products of our patient specimens there are clearly some strain differences between American, African, and Australian organisms.
|