| 2005 Case #11 |  |
|
|
During the past week the Gorgas Course in Clinical Tropical Medicine concluded with a 4-day field trip to Iquitos on the banks of the Amazon River. Iquitos, with a population of approximately 500,000, is the largest city in the world that is reachable only by air and by river. The nearest road ends over 400 km away. The patient was seen by the course participants at the Hospital de Iquitos together with Visiting Professor David Warrell (Oxford University), who provided the case presentation and commentary below. Publishing a case report every Monday for 11 consecutive weeks would not be possible without the assistance of an extremely dedicated group of people. We would like to thank in particular: Dr. Carlos Seas, Clinical Rounds Coordinator for the Gorgas Courses for case selection, coordination of case summaries and images; Drs. Jaime Cok and Juan Ferrufino for preparation and discussion of pathologic specimens; and Adam Plier of the UAB Division of Geographic Medicine for all publishing on the Gorgas Course web site. We hope you have enjoyed the 2005 series of live cases each week from Peru. The 2006 Gorgas Diploma Course runs annually in February and March and we will be in touch at the beginning of next year’s case series. The 2004 case series is now available for CME credit at no charge at http://www-cme.erep.uab.edu/onlineCourses/Gorgas04/HomePage/GorgasHome.htm. |
 History: 35 yo female walking bare-footed on her farm at dawn felt a sharp pain in her right ankle and found that she had been bitten by a 30 cm “cascavel” which escaped. Unconcerned, she continued to gather bananas for the next 20-30 minutes when she suddenly developed a headache, chest pain and loss of vision and collapsed to the ground where, according to her relatives, she remained unconscious for 30 minutes. When she awoke, she began to vomit yellowish material without blood. A tight tourniquet was then applied above the right ankle. She arrived at the emergency room at Hospital de Iquitos 2 hours post-bite complaining of headache and pain extending up the bitten limb to the right buttock and lower back. History: 35 yo female walking bare-footed on her farm at dawn felt a sharp pain in her right ankle and found that she had been bitten by a 30 cm “cascavel” which escaped. Unconcerned, she continued to gather bananas for the next 20-30 minutes when she suddenly developed a headache, chest pain and loss of vision and collapsed to the ground where, according to her relatives, she remained unconscious for 30 minutes. When she awoke, she began to vomit yellowish material without blood. A tight tourniquet was then applied above the right ankle. She arrived at the emergency room at Hospital de Iquitos 2 hours post-bite complaining of headache and pain extending up the bitten limb to the right buttock and lower back.
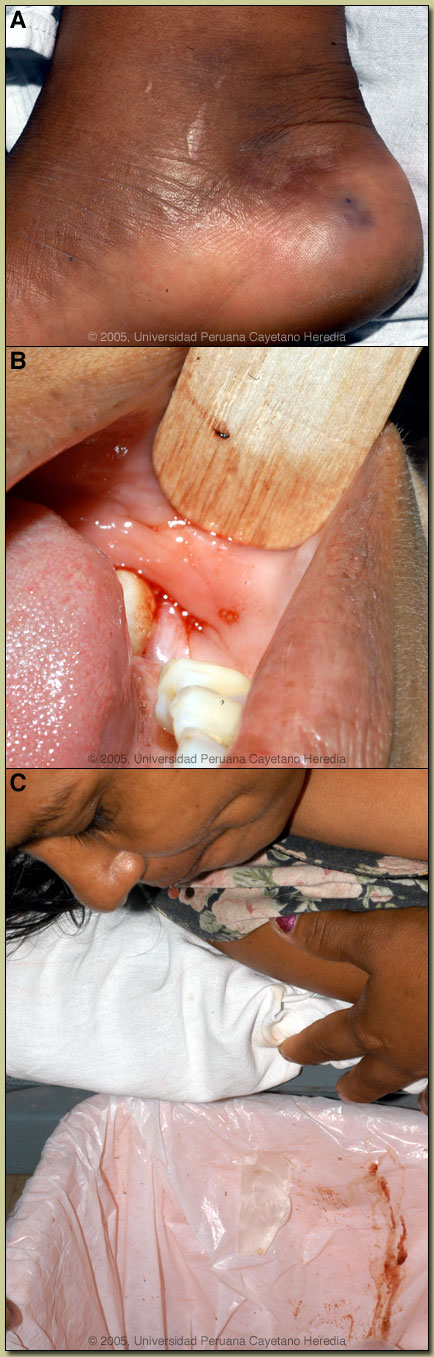
Epidemiology: Farmer-housewife from the Belen area of Iquitos. No previous snakebites. Physical Examination: On admission, she was distressed, restless and prostrate. She had not passed urine since the bite. BP 100/70 (later rising to 130/80), pulse 75/min. One fang mark (possibly two) was discernable on the medial side of the right ankle [Image A], with minimal local bruising. There was mild swelling distal to the tourniquet and tenderness of the whole right lower limb, especially below the knee and in the femoral canal and also of the right sacral region. There was brisk bleeding from several gingival sulci [Image B] but from no other site, and she spat out blood-stained saliva repeatedly [Image C]. Laboratory Examination: None performed by the time of the consultation. The Gorgas participants were asked to consider the likely snake species, whether antivenom would be indicated, and why she collapsed after the bite.
|
| Diagnosis: Envenomation with transient shock, systemic bleeding and likely coagulopathy due to Bothrops atrox [“jergón” (Perú), common lancehead (USA), fer-de-lance (France)], a common pit viper in nine South American countries. |
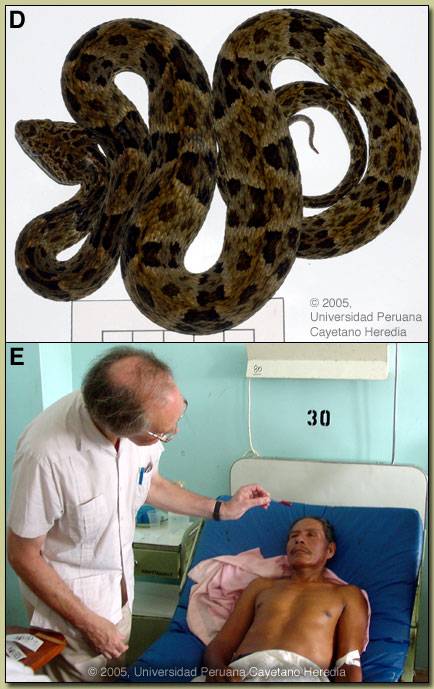 Discussion: Bothrops atrox is the most important cause of snakebite deaths and morbidity throughout the whole Amazon region, while other Bothrops species account for most serious snakebites elsewhere in Latin America. Bothrops range from Mexico and The Caribbean to Argentina. They occur in habitats from grasslands to rainforest and some are arboreal. Adult Bothrops atrox range in size from 70 cm. to nearly 1.5m. They possess heat-sensing pits between the eyes and the nostrils. Patients’ descriptions of the snake are often unreliable. In this case the patient thought she had been bitten by a “cascavel” (literally “rattlesnake”), a name used in north-eastern Perú, where there are no rattlesnakes, for juvenile Bothrops atrox because they vibrate their white tail-tips when alarmed. Discussion: Bothrops atrox is the most important cause of snakebite deaths and morbidity throughout the whole Amazon region, while other Bothrops species account for most serious snakebites elsewhere in Latin America. Bothrops range from Mexico and The Caribbean to Argentina. They occur in habitats from grasslands to rainforest and some are arboreal. Adult Bothrops atrox range in size from 70 cm. to nearly 1.5m. They possess heat-sensing pits between the eyes and the nostrils. Patients’ descriptions of the snake are often unreliable. In this case the patient thought she had been bitten by a “cascavel” (literally “rattlesnake”), a name used in north-eastern Perú, where there are no rattlesnakes, for juvenile Bothrops atrox because they vibrate their white tail-tips when alarmed.
Severe local swelling, blistering, bruising and necrosis are characteristic of envenomation by pit vipers but not elapids such as coral snakes. Local envenomation was trivial in this case, whereas systemic envenomation (early shock and spontaneous systemic bleeding) was dramatic and potentially life-threatening. She was probably bitten by a juvenile B. atrox, whose venom is relatively rich in anti-haemostatic factors and relatively poor in necrotic factors [Saldarriaga et al., Toxicon 2003 Sep 15;42(4):405-11]. The snake’s venom changes in composition as it grows, reflecting its changing prey. Coagulopathy is a common effect of procoagulant enzymes in venoms of vipers and pit vipers. Plasma clotting factors or platelets should not be administered until the venom has been neutralized by antivenom or they will merely “fuel the fire” of DIC. Many snakebites occur in settings where antivenom may be available in the absence of laboratory facilities. Using the bedside 20-minute whole blood clotting test [demonstrated by Professor Warrell on another patient without coagulopathy; see Image E], blood that fails to clot after 20 minutes in an untreated glass tube is a good sign of consumption coagulopathy, an indication for antivenom. If the test remains positive (non-clotting) 6 hours after the first dose of antivenom, another dose is needed. This patient received 4 vials of Instituto Nacional de Salud (Perú) anti-Bothropic polyvalent antivenom intravenously. Pre-treatment with corticosteroid or anti-histamines is common, but only subcutaneous epinephrine has been proved beneficial [Premawardhena et al., BMJ 1999 Apr 17;318(7190):1041-3]. Four hours after antivenom treatment, bleeding had stopped, she had passed clear urine and felt much better. No early anaphylactoid or pyrogenic reactions complicated antivenom therapy. The next day she was still feeling well. Her bitten foot was still tender but local envenoming had not progressed. There is no evidence to support the use of prophylactic antibiotics after snakebite. She probably collapsed because of autopharmacological effects of venom oligopeptides which inhibit angiotensin converting enzyme and potentiate bradykinin. In fact, the structure of ACE inhibitors was derived from a component of Brazilian Bothrops jararaca venom. The risk of envenoming after a Bothrops atrox bite is only about 50%. The practice of giving antivenom to every case of snake bite despite absence of envenoming is widespread. But antivenom is scarce, expensive and dangerous. It should be reserved for patients with systemic or severe, rapidly-evolving local envenomation. Anxiety after a bite can result in misleading symptoms including hyperventilation causing acroparaesthesiae, tetany and even syncope.
|