The UAB Pediatric Critical Care Fellowship is a fully accredited three-year program that combines research and clinical experiences to prepare our trainees to become excellent intensivists who are ready to become successful in the academic setting. The 36-month curriculum includes 15 months clinical service, 21 months protected research time and 16 weeks of vacation. All fellows are credentialed in Deep Sedation by the end of the first year of training.
Clinical Services are housed in the Children’s of Alabama Hospital, a 750,000 square foot, facility on the UAB health system’s downtown Birmingham campus.
Pediatric Intensive Care Unit (PICU)
- 9 months spent in PICU
- 24-bed multispecialty, combined medical surgical unit
- Approximately 2,000 admissions per year
- Wide variety of common and rare critical illnesses representing all subspecialties.
- Only level one pediatric trauma center and burn center in the state of Alabama, ensuring adequate preparation in caring for children with complex multiple traumas including those with serious traumatic brain injuries and burns.
The Cardiac Intensive Care Unit (CVICU)
- 4 months spent in CVICU
- 20-bed service
- Our institution has on average between 250-300 pump cases per year and 300 to 400 cardiac cases per year.
- Trainees are exposed to the care of children with complex heart defects including the use of extracorporeal membrane oxygenation and mechanical assist devices.
Additional clinical rotations
- Anesthesia
- Deep Sedation
- Pulmonary
- Palliative Care
- Cardiology/Interventional Cardiology
Fellows also devote time and effort to academic interests including research projects (clinical, translational, or bench research), and are able to select a research mentor from across all specialties on the UAB campus. Our faculty has developed a very extensive curriculum that is geared towards preparing our trainees to meet the challenges of being an excellent intensivist as well as facing the critical care boards successfully.
The critical care curriculum includes training in Quality Improvement with a one-day mini quality academy, and all fellows design and complete a QI project during the course of training. The fellows have exposure to a longitudinal didactic curriculum in ultrasound as well as hands-on training in the use of point-of-care (POCUS) ultrasound in the PICU, becoming POCUS credentialed by the end of training.
Program Information
-
Curriculum
First Year
-
-
4 months Pediatric Intensive Care Unit (PICU)
-
2 months Cardiac Intensive Care Unit (CVICU)
-
2 weeks Cath Lab / Cardiology
-
2 weeks Deep Sedation
-
1 month Anesthesia
-
4 months Research
-
Second Year
-
-
3 months PICU
-
1 month CVICU
-
2 weeks Palliative Care
-
7.5 months Research
-
Third Year
-
2 months PICU
-
1 month CVICU
-
9 months Research
Electives
Rotations are available in Critical Care Transport, Burn, Adult Critical Care, or any other critical care related rotations.
Point-of-Care Ultrasound (POCUS)
The fellows at Children's of Alabama have exposure to a longitudinal didactic curriculum in ultrasound and hands-on training in point-of-care (POCUS) ultrasound in the PICU. The longitudinal ultrasound educational series aims to foster clinical skills in integrating diagnostic and procedural ultrasound in the care of critically ill children. The series exposes trainees to various aspects of ultrasound, such as lectures, weekly hands-on sessions, and monthly image review sessions. The trainees also have an opportunity to participate in teaching, administrative, and research activities that will prepare them to be future leaders of critical care ultrasound at the local, regional, or national levels. The program graduated its first fellow with dedicated training in Critical Care-ED POCUS.
The educational series includes the following:
- Quarterly lectures on a diverse range of topics
- Participation in a national ultrasound educational series
- Exposure to a variety of ultrasound machines
- Proctored weekly hands-on scanning sessions
- Monthly image review and quality assurance sessions
- Opportunity to seek credentialing in POCUS to encourage independent practice and integration into patient care
- Ultrasound research
- Opportunities to educate medical students and residentsMore information about the program can be obtained by contacting Dr. Vidit Bhargava vbhargava@uabmc.edu or Dr. Luke Burton wlburton@uabmc.edu.
-
-
Conferences
PICU Noon Conference- Case Conference held weekly and Morbidity and Mortality Conference held every other month.
PICU Fellows’ Conference- The text, Fuhrman Pediatric Critical Care, 4th Edition, is used as the basis for the curriculum for this conference, with the entire textbook reviewed over a 3-year period. Journal Club is also a part of the Fellows’ Conference, and is held 5-6 times each year. Faculty facilitators assist fellows in selecting and presenting articles to be discussed at Journal Club.
Combined Fellows’ Conference- Includes fellows from Neonatology, Pulmonary, and Critical Care. The primary focus of these conferences is core physiology. Topics include research issues such as gathering and analyzing date; quality improvement topics; principles of diversity, equity, and inclusivity; and risk management topics.
Grand Rounds- features speakers from various departments here at UAB and external speakers from academic medical centers around the U.S.
Monthly Conferences
PICU/ED/Hospitalist Combined Fellow Conference- This is a combined conference for Critical Care, Emergency Medicine and Hospitalist fellows and covers topics such as shock, abuse, toxicology and respiratory cases.
Fellows’ Round Table- is an interactive session for pediatric fellows from all programs to present their scholarly work (planned, ongoing, or completed) and receive feedback from other fellows and faculty, in order to provide guidance on improving research proposals, develop presentation skills, and promote cross-divisional interactions and collaborations.
Ventilator Rounds- Co-lead by PICU faculty and respiratory therapists, this hands-on learning session discusses both the theory around and practical application of mechanical ventilation in the PICU. Topics include respiratory physiology as it pertains to mechanical ventilation, ventilator management (CMV, HFOV, APRV, etc), airway adjuncts and management of the difficult airway with focus on hands-on management at the bedside.
-
Research Training
The goal of the research experience is for the Critical Care fellow to learn sound methodology in designing and performing research studies and to learn how to correctly interpret and synthesize research data. During this phase of training, the Critical Care Fellow will work under close guidance of the research mentor and the Scholarly Oversight Committee. Fellows may choose any research mentor on the UAB campus – from clinical researchers, to translational researchers, to bench researchers.
Recent Fellows' Research Projects
-
Development of a novel delirium score for children in PICU
-
Improving sepsis outcomes through implementation of goal-directed algorithms
-
Long term PALS retention following Rapid Cycle Deliberate Practice
-
Hyperchloremic metabolic acidosis and acute kidney injury
-
Effect of Noninvasive ventilation vs. supplemental oxygen therapy on reintubation in high-risk infants following congenital heart surgery
-
Monitoring Central Venous Pressure and its Relationship to Achieving Initial Therapeutic End Points and Fluid Overload in Patients with septic shock
-
Tetranectin as a biomarker to predict low cardiac output state in pediatric patients following cardio-pulmonary bypass
-
Heparanase sulfation patterns in pediatric sepsis
-
Development of a machine-learning algorithm to predict extubation failure
-
Using the Therapeutic Intervention Scoring System (TISS) in children with chronic critical illness
Aya Al-Noubani
- QI: Improving Communication with Patients of Limited English Proficiency
- Research: POCUS Evaluation of Shorter Fasting Duration in Critically Ill Pediatric Patients
Leah Bittles
- QI: Increasing Reporting of Diagnostic Errors in the PICU
- Research: Assessment of Diagnostic Calibration in Pediatric Critical Care Providers: A Clinical Vignette Study
Chloe Braun
- QI: Improving Fluid Balance Management with Goal of Limiting Fluid Overload
- Research: Fluid De-resuscitation: Comparing the Approach of Intensivists and Nephrologists
W. Luke Burton
- QI: High CLABSI Risk—Screening and Intervening
- Research: Using Laryngeal Ultrasound to Determine Air Column Width and Its Use in Predicting Post Extubation Stridor
Josh Cooper
- QI: Handshake Stewardship Rounds in the Pediatric ICU
- Research: Trend in Use of Karius Testing at Large Children’s Hospital
Jeffrey Coote
- QI: Improving/Standardizing Procedural Consent in the PICU
- Research: Investigating the Utility of Augmented Reality Assistance in Ultrasound-Guided Procedural Training
Aphton Lane
- QI: Improving Documentation for Clinical Justification of Routine Labs
- Research: TISS-28 as a Dynamic Outcome Measurement After Pediatric Cardiac Surgery
Ananya Manchikalapati
- QI: Implementing a Need-Based Strategy to Obtain Routine CXRs and Decrease Overutilization in the Pediatric Intensive Care Unit
- Research: Tetranectin as a Biomarker for Low Cardiac Output State in Pediatric Patients Following Cardio-Pulmonary Bypass
Mitchell Moore
- QI: Improving Utilization of Patient White Boards for Following Intubation Details
- Research: A Machine-Learning Model to Accurately Predict Extubation Failure in the Pediatric Intensive Care Unit
Hugh Quach
- QI: Reducing Lab Costs Associated with Blood Gases
- Research: Effect of Sulfation Patterns of Soluble Heparan Sulfate Found in Pediatric Sepsis
Nicholas Rockwell
- QI: NG Feeding Bronchiolitics on HFNC
- Research: Improving Resident Physician History and Physical in Challenging Situations
Jeremy Ruhlmann
- QI: Improving Efficiency and Utilization of Spanish Interpreters in the Pediatric ED
- Research: Assessing Social Media Use Prior to ED Visits
Lece Webb
- QI: Using Syringe Manometer for Routine Monitoring of Endotracheal Tube Cuff Pressure and the Effect on Post Extubation Stridor
- Research: Predicting HFNC Therapy Outcomes Using ROX Index
Allison Williams
- QI: Delirium Reduction
- Research: Communicating Difficult News: Comparing Skills Retention in Pediatric Residents
Dixon Fellowship
The Dixon Foundation endows a fellowship program in Pediatrics expressly aimed at supporting post-doctoral training and research in approved Pediatric subspecialties to prepare outstanding fellows for a career in academia. The program was initiated in 1988 by Ed and Peggy Dixon following the loss of their grandson, Bradford Dean Dixon, to Biliary Atresia. As part of this prestigious award, recipients benefit from salary support and an additional $5,000 per year discretionary fund to support research and continuing education.
Chu Family Educational Scholarship
The Chu Family has provided a generous gift for educational initiatives. A large portion of the gift has been set aside specifically for Pediatric Fellows. A competitive process is in place for fellows to apply for these funds on a yearly basis. Some examples of education endeavors that are suitable for application include: Masters of Public Health, Masters of Science in Public Health, Quality Academy, Masters of Quality and Safety, Masters of Education, Masters of Business Administration and others. To date, Chu Scholarships have been awarded to 22 Pediatric Fellows to assist in furthering their educational goals.
-
-
QI Training
Quality Improvement is a systematic, data-driven, iterative problem solving process that can be adapted to local context.
Systematic: use of a standard methodology that ensures we do not “cut corners” when identifying, defining, measuring, and analyzing a problem. In other words, QI is not a NIKE project (“just do it”).
Data-driven: use of efficient and effective data gathering, measuring and analyzing techniques during baseline data collection as well as after implementation of an improvement.
Iterative: small tests of change when implementing a proposed solution are key to learning quickly about potential success.
Adapted to local context: we must recognize that the local culture (of the unit, organization, etc.) and needs of our “customers” require us to adapt a solution for best fit.
This passage by Paul Batalden (Qual. Saf. Health Care 2007;16:2-3) is a good summary: The combined and unceasing efforts of everyone – health care professionals, patients and their families, researchers, payers, planners, administrators, educators – to make changes that will lead to
- Better patient outcomes
- Better system performance, and
- Better professional development
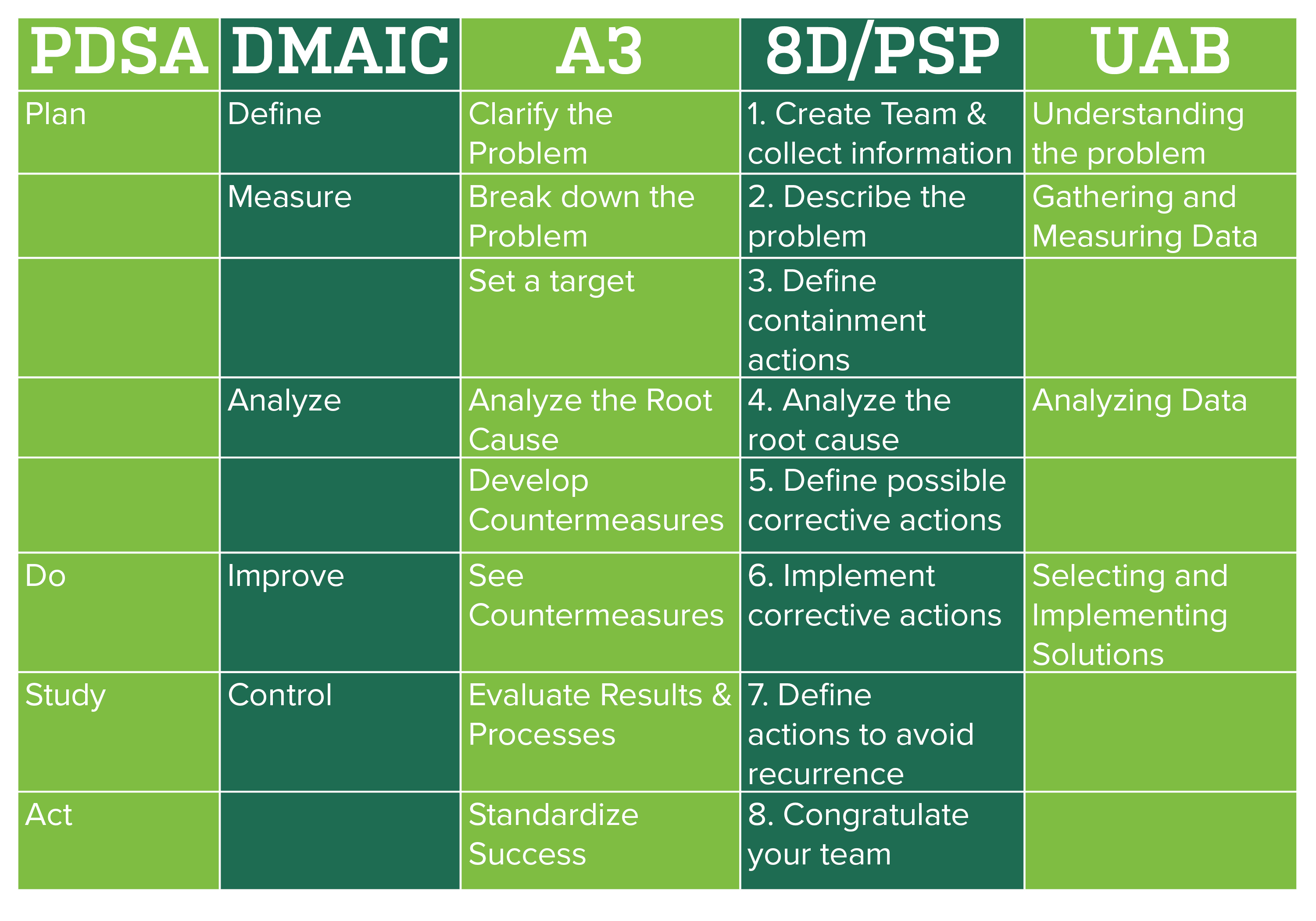
Below is a table comparing some of the more popular QI methodologies with the approach we take at UAB.Comparison of Different Quality Improvement Models
All residents and fellows at UAB/COA are provided a standard curriculum in QI and Patient Safety, through our Mini Quality Academy (MQA). This training provides the top 12 tools and skills needed to be an effective member of a robust QI team. It is offered in an adult-learning environment during a one day (8 hour) course. We are fortunate to additionally offer more in-depth training for those who wish to pursue a career in QI, Patient Safety, or Outcomes Research. These curricula include a Graduate Certificate Program in Healthcare Quality and Patient Safety, and a Master’s Degree in Healthcare Quality and Safety. Both of these programs are offered through the UAB School of Health Professions, and are excellent opportunities for our fellows to pursue during their training here.
The general outline for our fellows’ QI activity spans the 3 years of fellowship. A typical timeline for this work:
Year 1
-
Attend the MQA
-
Make observations about processes within critical care that need improvement
-
Meet with QI mentor twice to begin to identify a candidate project
Year 2
-
Fully define QI project
-
Identify team members for QI project
-
Data collection, measurement, and analysis
-
Continue regular meetings with QI mentor
Year 3
-
Implementation of improvement
-
Ongoing monitoring of the change
-
Preparation for publication of project
-
- Our Services and Facilities
FAQs
-
How can I apply for a pediatric critical care fellowship position?
To apply for an open pediatric critical care fellowship positions available, please submit your application and all relevant documents via the Electronic Residency Application Service ERAS.
-
What is the interview process?
Applications are accepted through ERAS starting in July and holistically reviewed by our program director and associate program director. We conduct our interviews virtually beginning in Late-August through Mid-October, hosting a half-day interview day where applicants will meet with program leadership, pediatric critical care faculty, and current pediatric critical care fellows. When possible, applicants will be paired with faculty who specialize in similar areas of interest.
-
Do you sponsor visas?
Yes, we sponsor J-1 and H-1B visas. You must have a valid ECFMG certificate included in your ERAS application.
-
Are there any other specific requirements for IMGs?
Yes, an applicant must meet Alabama Board of Medical Examiner requirements for State License. Must have completed USMLE steps 1-3 within 7 years of the first attempt.
-
Do UAB Pediatric Critical Care fellows have access to educational conferences?
Scholarship and learning are essential to the development and maturation of a pediatric intensivist during training. As such, conferences, case discussion, journal clubs, grand rounds and basic science seminars are fundamental experiences for each fellow during the entire training period.
Some of our conferences include:
UAB Pediatric Critical Care Division Conference, Pediatric Critical Care Fellow Journal Club, Pediatric Critical Care Fellow Career Prep, UAB Pediatrics Grand Rounds, UAB Pediatric Fellowship Core Conference, UAB Pediatric Fellowship Research Roundtable, Combined PICU/NICU Fellow Physiology Conference and Combined PICU/PEM/PHM Fellow Conference.
Some national conferences that are faculty and fellows attend are Society of Critical Care Congress, Pediatric Acute Lung Injury and Sepsis Investigators, Annual Assembly of Hospice and Palliative Care, Advances in Critical Care Nephrology, Society for Simulation in Healthcare and others.
Our Team

Priya Prabhakaran, M.D.
-
Letter from the Director
Thank you for your interest in the UAB Pediatric Critical Care Medicine Fellowship Program. Our fellowship website contains information about the fellowship program, the Critical Care Division, and the tremendous facilities we enjoy here at UAB and Children’s Hospital of Alabama.
 Our fully accredited three-year program combines research and clinical experiences that makes our graduates eligible and prepared for the American Board of Pediatrics Subspecialty Board examination in Pediatric Critical Care Medicine. The goal of the Pediatric Critical Care Medicine Fellowship Program is to provide trainees with the education, clinical experience, research training, and technical skills necessary to become excellent intensivists who are ready to become successful in the academic setting. The 36-month curriculum includes 17.5 months clinical service, 18.5 months protected research time, and nine weeks’ vacation.
Our fully accredited three-year program combines research and clinical experiences that makes our graduates eligible and prepared for the American Board of Pediatrics Subspecialty Board examination in Pediatric Critical Care Medicine. The goal of the Pediatric Critical Care Medicine Fellowship Program is to provide trainees with the education, clinical experience, research training, and technical skills necessary to become excellent intensivists who are ready to become successful in the academic setting. The 36-month curriculum includes 17.5 months clinical service, 18.5 months protected research time, and nine weeks’ vacation.
Clinical service takes place in the busy 22-bed multispecialty Pediatric Intensive Care Unit (10 months) and the 20-bed Cardiovascular Intensive Care Unit (4 months). The Pediatric Intensive Care unit is a combined medical surgical unit. With approximately 1,400 admissions per year, our trainees are exposed to children with a very wide variety of both common and rare critical illnesses representing all subspecialties. Children’s of Alabama is the only level one pediatric trauma center in the state of Alabama, and this ensures adequate preparation in caring for children with traumatic injuries, including those with serious traumatic brain injuries. The Cardiac intensive care unit is a busy service with approximately 250 cases of congenital heart disease that require cardiopulmonary bypass each year. Trainees are exposed to the care of neonate’s and infants with very complex heart defects including extracorporeal membrane oxygenation and mechanical assist devices. Both of these units are housed in the new Benjamin Russell Hospital for Children, a 750,000 square foot, $400 million expansion facility on the UAB health system’s downtown Birmingham campus. Fellows also complete clinical rotations with anesthesia, pulmonary, palliative care and cardiology/cath lab services.
Fellows devote time and effort to academic interests including research projects (clinical, translational, or bench research), and are able to select a research mentor from across all specialties on the UAB campus. The critical care curriculum also includes training in Quality Improvement with a one-day mini quality academy and a required QI project to be completed during the course of training. Our faculty has developed a very extensive curriculum that is geared towards preparing our trainees to meet the challenges of being an excellent intensivist as well as facing the critical care boards successfully.Priya Prabhakaran, M.D.
Professor of Pediatrics
Director, Critical Care Medicine Fellowship