Displaying items by tag: division of pulmonary allergy and critical care medicine
Tagged under
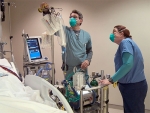
UAB is part of a clinical trial published in the New England Journal of Medicine that showed using bag-mask ventilation improves outcomes and could potentially save lives.
Tagged under
Tagged under
This finding may point to a therapeutic target to treat tuberculosis, which kills 1.3 million people each year.
Tagged under
With one in four high school students’ using e-cigarettes, UAB experts want parents to be aware of vaping’s harmful effects.
Tagged under
Tagged under
The grant, received from the NIH, aims to provide a better option for patients than what is already available.
Tagged under
A diabetes drug suggests potential therapy for idiopathic pulmonary fibrosis, based on research with human lung fibroblasts and a mouse model of lung fibrosis.
Tagged under
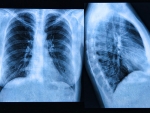
One-way valves that control air flow in the lungs have been shown to be effective in improving breathing for emphysema patients.
After living with pulmonary fibrosis for 15 years, Quintarius Daniels received a life-changing lung transplant that has helped him live the life he has always wanted.
Tagged under
Researchers will discuss how to age with a high quality of life during the Comprehensive Center for Healthy Aging 2018 Symposium on April 26.
Tagged under
This microRNA is a biomarker for bronchopulmonary dysplasia, a disease that can lead to death or long-term disease in extremely low birth-weight infants.
Tagged under
 Physicians at UAB share tips on men’s health and how it affects heart health, sexual function and memory and decreases cancer risk.
Physicians at UAB share tips on men’s health and how it affects heart health, sexual function and memory and decreases cancer risk.
Tagged under
ECMO and autoantibody reduction through plasma exchange, experimental therapies not available everywhere, help end an Alabama woman’s five-month medical ordeal.
Tagged under
A two-drug combination therapy for cystic fibrosis is shown to be effective. Triple combination therapy is close behind.
Tagged under
A new UAB study will investigate the role of autoantibodies and the benefit of therapeutic plasma exchange on a deadly lung disease.
A UAB physician will co-chair a steering committee of global cystic fibrosis experts and clinical trial investigators to support the design, conduct and execution of the triple combination pivotal study program.
Tagged under
Successful Phase III trials at UAB contributed to the development of a novel “corrector-potentiator” combination drug therapy for cystic fibrosis patients.
Tagged under
As lung diseases worsen worldwide, UAB has launched a pre-doctoral training program in pulmonary research that will focus on lung diseases such as asthma, cancer, COPD, cystic fibrosis, pneumonia, lung injury and idiopathic pulmonary fibrosis.
Tagged under