| 2010 Case #4 |  |
|
| Diagnosis: Brucella spondylitis with paravertebral abscesses due to Brucella melitensis. |
| Discussion: The patient had been transferred from the orthopedic service with a presumptive diagnosis of Pott’s disease (TB spondylitis). Percutaneous drainage of the paravertebral abscess yielded 400 cc of purulent odorless pus. Gram stain was negative and AFB stain was negative, but culture for Brucella melitensis was positive.
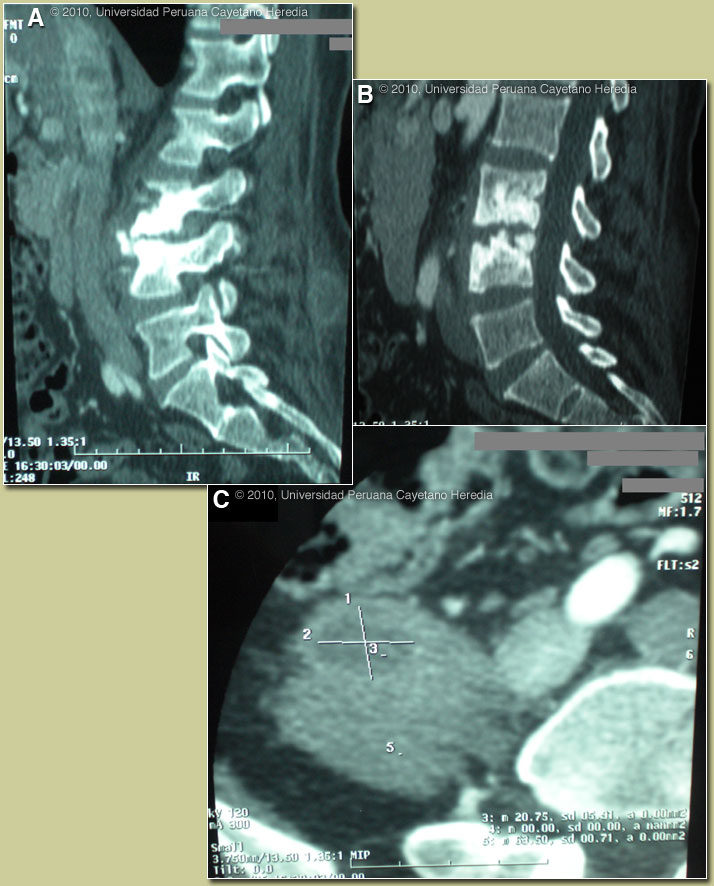
Serum agglutination test for Brucella was positive at 1/640 with 2-mercaptoethanol positive at 1/320. The diagnosis of Brucella is usually made by serology. In highly endemic areas a slide or tube agglutination test for Brucella is part of the routine initial testing of every febrile patient. The test is cheap, easy to do, and results are available the same day. Blood cultures are expensive and a positive result may take many days, and the sensitivity is only about 70% in Perú (and is lower in most US series), even after 2 sets of blood cultures. Bone marrow cultures are more sensitive (>90%) but are invasive and expensive. In addition, Brucella is a bio-hazard and cultures require biosafety level 3 precautions. The basic agglutination test detects both IgM and IgG antibodies. The addition of 2-mercaptoethanol destroys the binding ability of only the IgM antibody so this test detects the presence only of Brucella specific IgG. With successful treatment, IgG antibody does not often persist at any positive level (≥1/80) for more than a year, and should start diminishing very soon after treatment. Official reading of the CT scan of the spine: disc space narrowing between L3-4, extensive erosive lesions on the anterior-superior angle of L3 (called Pon’s sign) [Image A] and on the articular surface of L3-4 [Image B]. New bone formation with bridging osteophytes is found between L3-4 [Image A]. Marked widening of the right iliopsoas muscle with internal hypodense lesions is demonstrated in Image C. The major differential diagnosis given the fever, night sweats, and these abnormal spine films includes Brucella, TB, and malignancy. Several features of the spine films make the lesions seen diagnostic of brucellar disease: 1) lumbar location; 2) pathognomonic bridging osteophytes between adjacent vertebrae simultaneous with the presence of both osteoblastic lesions and loss of bony mass in the same vertebrae; 3) loss of disk space; and 4) loss of definition of bone at top of the affected vertebrae. Spondylitis may present as the first manifestation of brucellosis (10% in a recent review) and is usually lumbar in location. Iliopsoas abscess is reported in 10% of cases of brucella spondylitis and a paravertebral mass in 46%. On questioning, the patient gave a history of regular ingestion of unpasteurized goat cheese for the last two to three years. This is a frequent scenario in Perú and most countries at highest risk of brucellosis, with the predominant agent being B. melitensis. Brucellosis due to B. abortus acquired from cattle is increasingly uncommon in the US and other countries. All travelers with fevers of unknown origin should be queried for a history of goat cheese ingestion. B. melitensis is commonest in Mexico, Venezuela, Perú, the Mediterranean countries and several of the Arabic countries of the Middle East. The radiologic findings should be contrasted with last week’s case of TB spondylitis [see Gorgas Case 2010-03]. Classic plain x-ray film findings in brucella spondylitis can be found seen in one of our cases from 2001 [see Gorgas Case 2001-02]. Salmonella infection or staphylococcal infections may cause spondylitis and paravertebral abscess but concomitant high fever and systemic illness would be seen. Isolated paravertebral abscesses are most often caused by staphylococci and enteric organisms in the developed world, but tuberculosis and brucellosis, which cause cold abscesses, are reportedly more common causes of paravertebral abscesses in the developing world. Pyomyositis has recently become more common in non-tropical countries in HIV patients and may occur in the psoas muscle. The patient was started on a combination of doxycycline plus gentamicin for 1 week, followed by doxycycline plus rifampin for 11 more weeks. Symptoms subsided after 2 weeks of treatment (fever after 1 week and lumbar pain after 2 weeks). She is able to walk and no residual lumbar pain was observed. Duration of treatment of brucella spondylitis for 12 weeks is recommended in a recent review [Clin Infect Dis. 2008 Feb 1;46(3):426-33], but failures were reported in approximately 15-18%. No differences in outcome were observed whether aminoglycosides were used for the 1-2 weeks or not; however there were only 16 patients in the doxycycline-rifampin group. |