 |
Gorgas Case 2018-10 |
 |
|
The following patient was seen in the outpatient department of the Tropical Disease at Cayetano Heredia Hospital in Lima, Peru during the Gorgas Advanced Course. 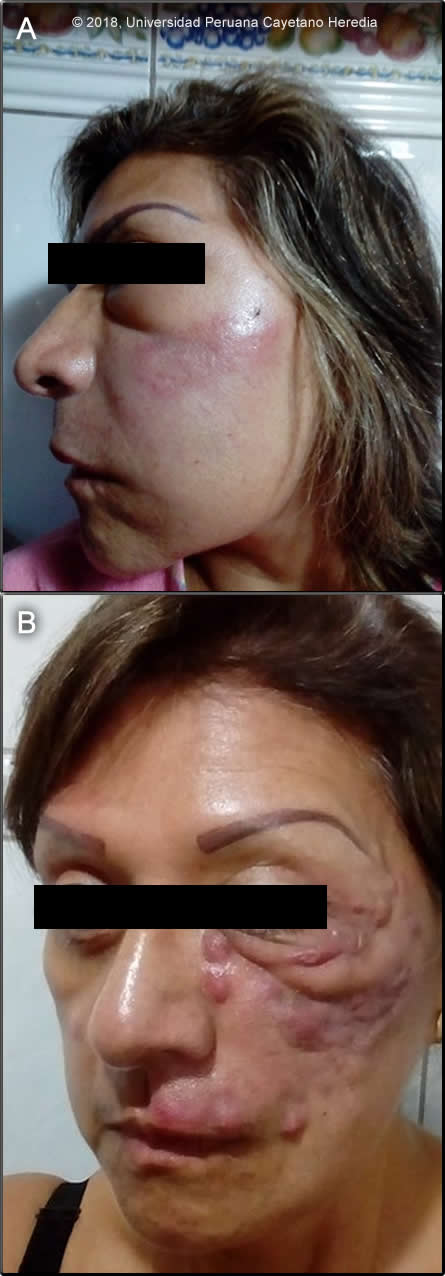
 History: A 56-year-old female presented with a 2-month history of progressive swelling of the left malar, periorbital, and upper lip areas associated with the appearance of multiple non-painful nodular lesions. The patient reports swelling and erythema of these areas (Image A) with no fever or constitutional symptoms beginning 1 week after a cosmetic procedure whereby fat from her abdomen was injected into both cheeks. She subsequently received 30 days of multiple sequential antibiotics including clindamycin, intramuscular ceftriaxone, amoxicillin/clavulanate and steroids with resolution of the swelling over the malar and periorbital regions but with the appearance of multiple painless nodular lesions ranging from 0.5 cm to 1 cm in diameter in the malar and upper lip regions. Over the next month, the nodular lesions evolved into abscesses which were drained. Culture for usual bacteria and Ziehl-Neelsen staining were negative and she was referred to our institution for further evaluation. Epidemiology: Born and resides in Lima. Recent travel to San Andres island, Colombia as well as Huancayo and Ancash in the Peruvian highlands over the last year for tourism. No known TB contact. She has had hypothyroidism for 26 years in treatment with levothyroxine. Physical Examination: BP: 120/80 mmHg. HR: 74 bpm. RR: 18 rpm. Afebrile. Skin: multiple abscesses located on the left malar region, left upper lip and right malar region over an edematous and erythematous base with skin retraction on the left suborbital area (Image B). No lymphadenopathy, no oral or intranasal lesions. Normal chest cardiovascular and abdominal examination. Laboratory Results and Imaging: Hct: 43.8%; WBC 11,700 (78 neutrophils, 15 lymphs, 5 monos); 379,000 platelets INR: 1.17; total protein 6.66 g/dl (N 5.8-8.1); albumin 3.69 g/dl (normal); globulin 2.97 (N 2-3.5); total bilirubin: 0.25mg/dl; ALT 17 U/L (N=< 40); AST 15 U/L (N=<40); Alk phosphatase 45 mg/dl (N 15-60). HIV and HTLV-1 tests were non-reactive. UPCH Case Editors: Carlos Seas, Course Director / Carlos McFarlane, Associate Coordinator
UAB Case Editor: David O. Freedman, Course Director Emeritus / German Henostroza, Course Director |
|
Diagnosis: Mycobacterium chelonae. Iatrogenic subcutaneous infection.
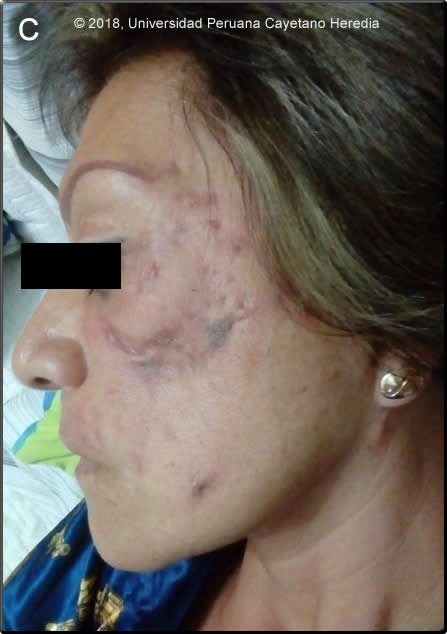
 Discussion: With an increase in cosmetic procedures (mesotherapy, liposuction, fat autografting, and breast augmentation), skin and soft tissue infections caused by rapidly growing mycobacteria (RGM) are increasing in incidence (Aesth Plast Surg 2017;41:1150–1154; Clin Infect Dis 2009; 49:1358–64). "Lipotourism" to Latin America has been associated with RGM outbreaks in returning travelers to the US and Europe <https://www.cdc.gov/mmwr/preview/mmwrhtml/mm6309a5.htm>. Common source outbreaks have also been reported after acupuncture, insulin injections, tattooing procedures (N Engl J Med 2012;367:1020-4), and potentially with any procedure that involves injectable materials, artificial prostheses, central venous catheters and implantable devices. Mesotherapy has become a popular procedure in Latin America despite of lack of scientific evidence for its utility (Rev Saúde Pública 2008;42:146-9). Mesotherapy involves injecting various substances into the dermis that supposedly eliminates fat tissue in an attempt to contour the body. Fat injection procedures are also becoming popular as they are considered safer and associated with better esthetic results (Plast Reconstr Surg 2011;128:545–555). Contamination of substances injected during mesotherapy and of tattoo ink are more implicated than the procedures themselves (Rev Saúde Pública 2008;42:146-9; N Engl J Med 2012;367:1020-4). Mycobacterium chelonae is a nontuberculous, Runyon type IV mycobacterium found in water, soil, plants, dairy products, and cold-blooded animals. In humans, it is usually seen in immunosuppressed patients, presenting with disseminated infection. However, after skin inoculation infection often presents with induration, edema, erythema, draining subcutaneous nodules, abscesses, and also with constitutional symptoms. For instance, a Peruvian report indicates that during a period of two months, 35 patients underwent mesotherapy at a local private clinic, all of them developed skin lesions,13 patients were evaluated at our Institution. In these 13 patients, the mean incubation period was 16 days; fever was reported in 40%; sub cutaneous nodules and abscesses were reported in 92% of them, 8% presented with skin ulcers; M. chelonae was isolated form 4 patients and from a procaine vial used during the procedures (Rev Saúde Pública 2008;42:146-9). Our patient presented with inflammatory manifestations very quickly after the procedure, early infections by M. chelonae have been reported even within one week but usually occur several weeks of the esthetic procedure. However, in this case we cannot rule out a cellulitis caused by common bacteria that resolved with antibiotics which was then followed one month later by the classical manifestations of subcutaneous infections caused by RGM. Diagnosis is complicated and often delayed and requires a high index of suspicion and close collaboration with the microbiology laboratory. M. chelonae, M. fortuitum and M. abscessus are RGM. These RGM have the ability to grow usually within one week on solid medium. Drug susceptibility tests (DST) are performed at reference laboratories; clinicians often claim that no direct correlation between susceptibility results and clinical efficacy is observed. DST to aminoglycosides, fluoroquinolones, clarithromycin, azithromycin, linezolid, imipenem, doxycycline, cefoxitin, trimethoprim-sulfamethoxazol and tigecycline is recommended. Unfortunately, no evidence-based data exist from randomized controlled trials to guide the proper therapy. M. chelonae is often fully resistant to first line anti tuberculous medications. Expert recommendations for limited soft tissue infections are for at least four months of treatment with two oral agents to which the cultured isolate is susceptible, but for more severe soft tissue infections parenteral therapy with two agents based on culture susceptibility results are suggested (J Infect Dis. 1985;152:500; Ann Intern Med 1993;119:482). Once the patient clinically improves, switching to oral therapy with two medications for a total of six to twelve months is advised. Multiple surgical debridements are always needed to reduce the burden of infection. The treatment recommendations at our center for this kind of infections include 3-drug therapy with an aminoglycoside (we prefer amikacin) until there is clinical improvement and two oral agents that usually include a quinolone and clarithromycin for at least 6 months. This patient was started empirically with amikacin 15mg/kg per day for 10 days, and levofloxacin 750 mg PO qd plus clarithromycin 500mg PO bid that she received for 6 months with continuous aspiration of the skin abscesses. The patient improved significantly as seen in Image C, taken after 6 months of treatment. Tobramycin, which has the highest in vitro activity against M. chelonae, is not available in Peru; the strain from our patient was susceptible to amikacin. Despite in vitro quinolone resistance, the patient was improving clinically when the DST results became available and the strain was resistant to the other drug classes as well. |