 |
Gorgas Case 2018-02 |
 |
|
The following case was seen in the ICU of Cayetano Heredia Hospital in Lima by the 2018 Gorgas Course participants.

 History: 79-year-old man is brought to the ER after having vomited twice over the previous 4 hours approximately 200 cc of blood clots, and experienced one episode of black stools. Denies abdominal pain or nausea. After a new episode of hematemesis in the ER (Image 1) the patient was admitted to the ICU for vasopressor support.
Past Medical History: Intermittent cough and wheezing over the course of the last year, with intermittent, salbutamol, dexamethasone or prednisone (most recently a single dose of 20 mg prednisone 1-2 months prior to presentation). Epidemiology: Born in Piura on the north coast of Peru, moved to Lima and has been living there for the past 50 years. No known TB contacts. Physical Examination: Patient is admitted in a wheelchair, awake, breathing spontaneously, appears acutely ill. BP: 52/36, HR: 89, RR: 18, Sat: 96 % (FiO2: 0.21). Skin: pale. Chest: clear to auscultation bilaterally, no crackles. Cardiovascular: irregular heartbeats, no murmurs, no S3. Abdomen: soft, mild distended, bowel sounds heard, not tender to palpation. Gross melena on rectal exam. Laboratory Examination (on admission): INR: 6.47, PT: 13, aPTT: 66.5. WBC 12.6 (0% bands, 84% segmented, 1% eosinophils). Hb 7 g/dL, Hct 22%. Platelets 176 000. Glucose 197 mg/dl. Urea 161.7 mg/dl. Creatinine 1.3 mg/dl.
UPCH Case Editors: Carlos Seas, Course Director / Karen Luhmann, Associate Coordinator UAB Case Editor: David O. Freedman, Course Director Emeritus / German Henostroza, Course Director |
|
Diagnosis: Massive infestation with Ascaris lumbricoides
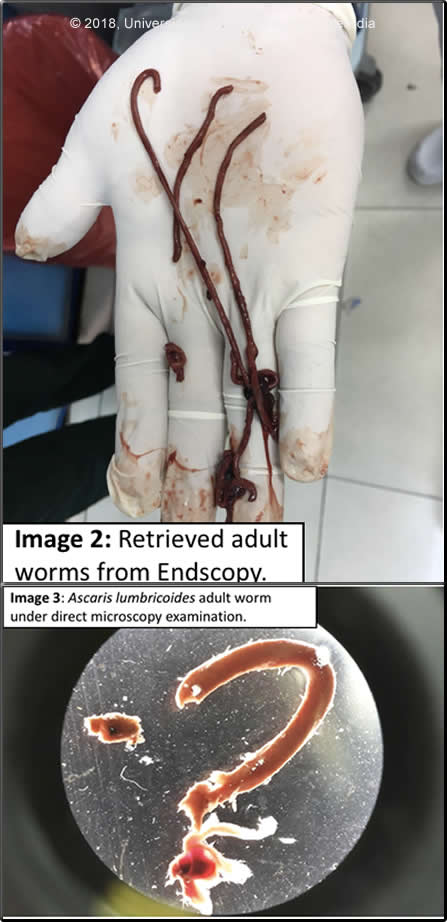
 Discussion: Upper endoscopy was technically difficult due to persistent bleeding. Endoscopy Report: A large blood clot is observed, which does not allow visualization of the gastric fundus. No active bleeding observed in the pylorus, duodenal bulb, or second portion of the duodenum. Helminth debris are found throughout. The incidental presence of massive Ascaris lumbricoides infestation in this patient with unrelated gastrointestinal bleeding and elevated INR was made by examination of the content of the vomitus from the initial presentation (Image 2-3). A stool O & P was negative for both Strongyloides stercoralis and hookworm both of which may cause bleeding in some circumstances. Ascaris lumbricoides infects an estimated 800M people mostly in the tropics with year-round transmission. Latin America accounts for approximately 8% of the total burden of infection. Children are most affected (particularly under 10 yo) but adults can also be infected. A study conducted in the Andean area of Ayacucho, Peru found that the prevalence of Ascaris lumbricoides was 4.5% among patients of all ages (Rev Gastroenterol Peru 2005;25:150). Higher rates of infection (37% among school-aged children) have been reported in a similar community in Peru (Osong Public Health Res Perspect 2017;8:302). Humans get the infection by ingesting either food or water contaminated with eggs that hatch in the small intestine releasing larvae that migrates to the large intestine and cross the intestinal wall to migrate to the lungs via lymphatic or hematogenous spread. Within the alveoli, larvae mature over 14 days to migrate to the bronchial tree to be then swallowed finally to be located in the small intestine, mostly in the jejunum. Adults do not multiply in humans; worm burden can be extremely large. Most infections are asymptomatic. During the lung passage of larvae (5-15 days after ingestion) patients may present with dry cough, fever, dyspnea and blood-tinged sputum. Wheezing can be detected on physical examination. Peripheral eosinophilia can be observed as well as migratory pulmonary infiltrates, especially when the burden of parasites is large. Our patient complained of respiratory symptoms for one year before admission, likely as a result of pulmonary migration of larvae. Eggs are not detected in the stools of these patients as the larvae must mature in the intestine later on. Intestinal manifestations are non-specific and include abdominal pain, nausea and diarrhea. When the intestinal burden is large, complications such as intestinal obstruction can be seen (Rev Chilena Infectol 2016;33:572), the ileocecal valve is the usual place of obstruction. on rare occasions, adults migrate to the biliary tract causing cholangitis, pancreatitis, and hepatic abscesses (see case 2002-05). As adult ascaris lie free in the intestinal lumen, gastrointestinal bleeding is not a complication of ascariasis. Diagnosis is generally made by detecting eggs for which the Kato-Katz test is recommended, its sensitivity has been more recently questioned compared to the Lumbreras rapid sedimentation method for detecting A. lumbricoides (85% vs. 95%, Pathog Glob Health 2016;110:130). Adult worms are sometimes regurgitated through the mouth or nose especially in children and because of the large size can be diagnosed on gross morphology as is the case in our patients. Adult worms may also be passed per rectum. Ascaris is exquisitely sensitive to all the usual antihelminthic agents used for intestinal helminths including albendazole, mebendazole, pyrantel pamoate, and piperazine (still used in resource-limited settings). |