 |
Gorgas Case 2020-07 |
 |
|
The following patient was seen as an outpatient at Hospital Cayetano Heredia during the Gorgas Diploma Course. We would like to thank Dr. Rodrigo Cachay for his assistance with this case.
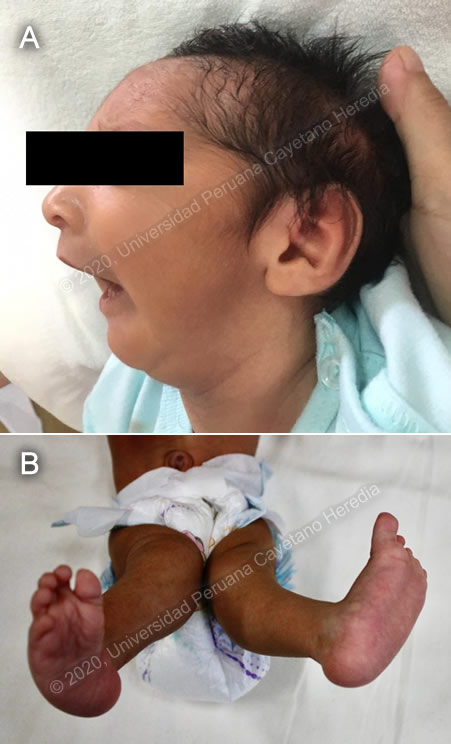 History: A 27-year-old woman presented at 10 weeks of pregnancy with a pruriginous generalized rash associated with malaise and subjective fever, which resolved within a week without any treatment. Routine obstetric ultrasounds were reported as normal up to the 25th gestational week when estimated fetal weight was shown to be below the 1st percentile, and a diagnosis of severe intrauterine growth restriction was made. Additionally, fetal periventricular, basal ganglia and intraparenchymal calcifications were described, along with right ventriculomegaly, lissencephaly, and calcification of mitral valves. A male baby was born at 36 5/7 weeks. Epidemiology: Mother denied any past medical history or drug use. Born and lived in Jaen, Cajamarca, in the high jungle of Peru. Received all recommended immunizations for pregnant women as per national guidelines. Physical Examination: At birth: Weight 1900g, height 45cm, head circumference 28cm (less 3rd percentile). The patient had evident microcephaly, retrognathia, and valgus deviation of lower extremities with a left club foot (Images A and B). At two months of age: The patient appeared malnourished. No skin findings. The pulmonary exam was normal and the cardiovascular exam revealed an I/VI systolic murmur in precordium. On neurological examination, the patient was excitable, had a punctiform fontanelle, hypertonic posture with distal quadriparesis, and did not follow objects with the eyes. Reflexes were normal and cranial nerve examination was unremarkable. Fundoscopy was normal. Imaging Studies: Hip ultrasound: type II de Graff hip. X rays of extremities: signs of mild hip dysplasia, deformation of the longitudinal axis in knees. Echocardiography: Mild left hypertrophic cardiomyopathy with preserved systolic function and diastolic dysfunction, indirect signs of mild pulmonary hypertension. Laboratory: Normal CBC. IgM for rubella, cytomegalovirus, herpes I and 2, toxoplasma were negative. Mother was also negative for TORCH and HIV. Further examinations: Electroencephalogram showed low asymmetric activity predominantly at the left hemisphere, no paroxysms. Evoked auditory and visual potentials were normal.
|
|
Diagnosis: Congenital Zika virus infection 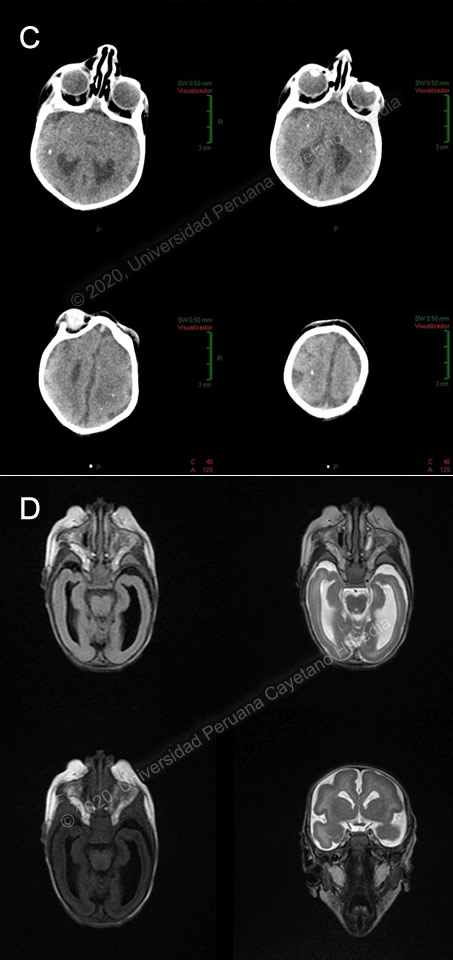
 Discussion: RT-PCR for Zika virus for the mother came back positive and close monitoring of her pregnancy ensued. Zika PCR and serology for the newborn was unavailable. A brain CT revealed microcephaly, bilateral calcifications of basal ganglia and frontal white matter, pachy-polymicrogyria in both hemispheres, and ventriculomegaly (Image C). Brain MRI showed bilateral frontal pachygyria, temporal, parietal and occipital bilateral lissencephaly, and dysplasia of the corpus callosum (Image D). Zika virus is flavivirus transmitted by mosquitoes, most commonly Aedes aegypti. It is closely related to other flaviviruses such as dengue, yellow fever and West Nile virus. Although it was first isolated in 1947, the first major outbreak occurred in 2007 in Micronesia, with an estimated 5000 infections among a population of 6700. By 2014, the virus had made its way to Latin America and after five years the largest number of cases were reported in Brazil (231,725), Colombia (98,803) and Venezuela (60,146) (PAHO/WHO). The first cases of Zika virus in Peru were reported in 2016 in the regions of Cajamarca and Loreto; last year, during the patient’s mother’s pregnancy, there was an active outbreak in the city of Jaen from February to August with a cumulative incidence of 1869 cases. Congenital transmission of Zika virus can occur at any moment during pregnancy and even peripartum, but the highest risk for fetal sequelae occurs with first and second-trimester infections. Following maternal infection, the virus is believed to infect the placenta and migrate to the fetal brain, where it causes apoptosis of neural progenitor cells (Curr Opin Virol, doi:10.1016/j.coviro.2017.09.005). Acute Zika virus infection presents with non-specific symptoms including maculopapular pruritic rash, fever, arthralgia, conjunctivitis, myalgia, and headache. It has been strongly associated with Guillain-Barré syndrome (N Engl J Med, doi: 10.1056/NEJMra1602113). Congenital infection causes a wide range of clinical manifestations in the fetus. Fetal cranial morphology may be severely altered, with microcephaly, overlapping cranial sutures, and redundant scalp skin, with extreme craniofacial disproportion. Brain anomalies such as subcortical intracranial calcifications, increased fluid spaces, cortical thinning and abnormal gyral patterns, hypoplasia or absence of the corpus callosum, decreased myelination and cerebellar hypoplasia are frequently associated. Ocular abnormalities such as cataracts, intraocular calcifications, chorioretinal atrophy, and optic nerve anomalies have also been reported. Congenital musculoskeletal abnormalities such as arthrogryposis and clubfoot are commonly observed as well, probably due to affection of the corticospinal tract or motor neurons. Cardiac abnormalities have a reported prevalence of around 10%, and are usually not severe (PLOS Negl Trop Dis, doi: 10.1371/journal.pntd.0006362). Five to ten percent of pregnancies with documented Zika infection result in fetal loss (JAMA Pediatr, doi: 10.1001/jamapediatrics.2016.3982). In the case presented, the patient had evidence of significant musculoskeletal and neurological involvement, as evidenced in the physical exam and brain imaging. Diagnosis is made by detection of viral nucleic acid by PCR or of IgM antibodies by ELISA. Viremia is usually transient, though it may last longer in pregnant women with evidence of fetal congenital infection, so a negative PCR does not rule out the diagnosis. IgM is thought to appear as viremia fades, within the first week after symptom onset, and it typically persists for months. Serology may cross-react with other flavivirus such as dengue (N Engl J Med, doi: 10.1056/NEJMra1602113). There are no reliable tests for prenatal and antenatal diagnosis of congenital Zika virus infection, although in some cases the amniotic fluid or cord blood might have a positive PCR. The diagnosis is confirmed by positive serum, urine of cerebrospinal fluid PCR for Zika virus in the newborn, in samples collected within the first two days of life (MMWR Morb Mortal Wkly Rep, doi: 10.15585/mmwr.mm6641a1). The differential diagnosis for congenital Zika infection must include other congenital infections that may cause microcephaly such as rubella, cytomegalovirus or toxoplasmosis. Rubella typically presents with congenital glaucoma and pigmentary retinopathy. Cytomegalovirus presents with a periventricular pattern of intracranial calcifications, as opposed to the subcortical distribution in Zika infection. Toxoplasmosis usually presents with diffuse intracranial calcifications. Of note, congenital Zika infection does not present with hepatosplenomegaly nor skin lesions (Am J Public Health, doi: 10.2105/AJPH.2016.303115) Although these findings may help differentiate between different entities, the final diagnosis must be made with virologic studies. Non-infectious causes of congenital abnormalities must also be ruled out. Patients with suspicion of congenital Zika virus infection should have a head ultrasound and a comprehensive ophthalmologic exam during their first month of life, as per CDC recommendations. There is no specific treatment, but patients should receive supportive management for complications (MMWR Morb Mortal Wkly Rep, doi: 10.15585/mmwr.mm6641a1). Prevention centers on avoiding mosquito bites through usage of mosquito repellent, bed nets, and window screens, and applying permethrin on clothes. Pregnant women should not travel to endemic areas. There is no vaccine against Zika, although there are several candidates in clinical phase I/II trials (Cell Host Microbe, doi: 10.1016/j.chom.2018.05.021). Our patient is being followed up by a multidisciplinary team comprised of pediatric neurologists, cardiologists, orthopedic surgeons, dietitians and, and undergoing physical therapy for hypertonicity. References: |