| 2009 Case #7 |  |
|
| Diagnosis: Splenic and extrahepatic hydatidosis due to Echinococcus granulosus. |
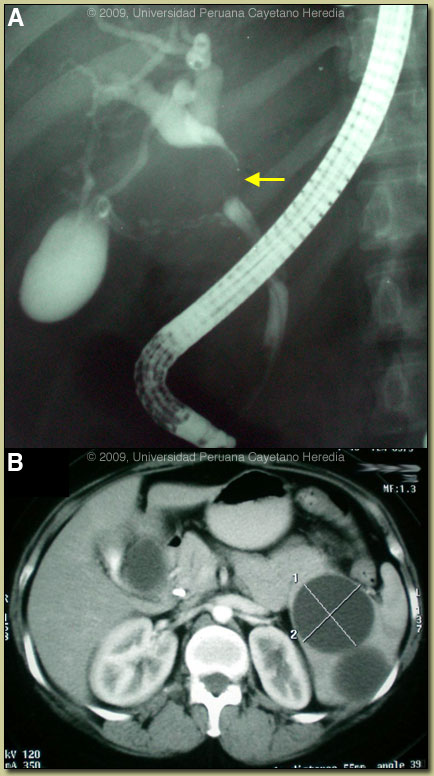
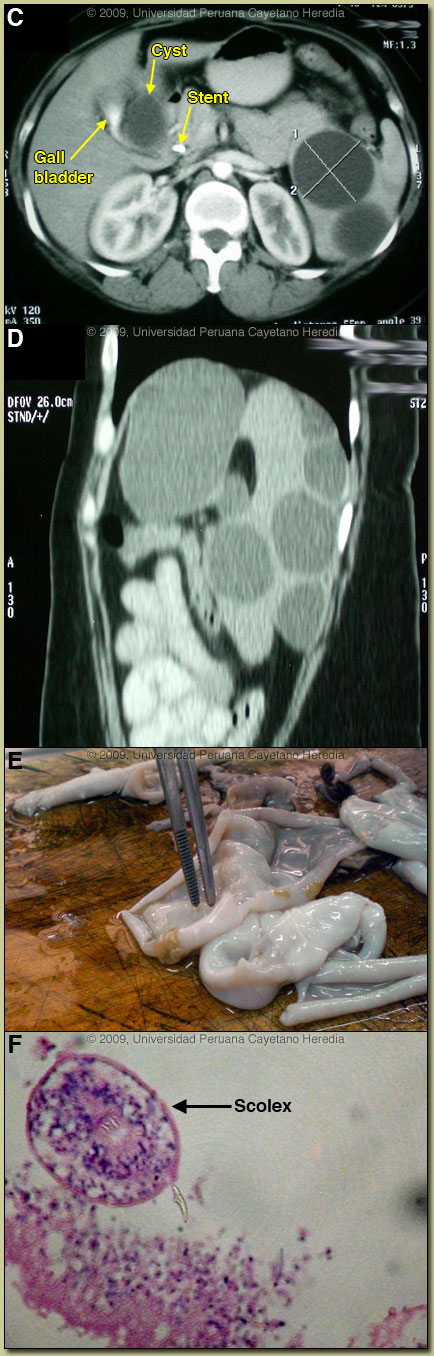 Discussion: A western blot was strongly positive for E. granulosus. Review of the CT disclosed displacement of the gallbladder due to a 3 cm cystic lesion that appeared to be extrahepatic and which at the same time appeared to be compressing the common bile duct [Image C]. Six cystic lesions within the spleen were observed [Image D]. In Perú, this is a very unusual presentation of hydatid disease with extrinsic compression of the CBD by a cyst causing cholestatis. No evidence of primary sclerosing cholangitis or cholangiocarcinoma was found during imaging or during later laparatomy (see below). Discussion: A western blot was strongly positive for E. granulosus. Review of the CT disclosed displacement of the gallbladder due to a 3 cm cystic lesion that appeared to be extrahepatic and which at the same time appeared to be compressing the common bile duct [Image C]. Six cystic lesions within the spleen were observed [Image D]. In Perú, this is a very unusual presentation of hydatid disease with extrinsic compression of the CBD by a cyst causing cholestatis. No evidence of primary sclerosing cholangitis or cholangiocarcinoma was found during imaging or during later laparatomy (see below).
Human hydatid disease secondary to Echinococcus granulosus is caused by the larval form of this dog tapeworm. Humans ingest the tapeworm eggs in environments contaminated by canine feces and become accidental intermediate hosts. Sheep are the normal intermediate hosts. Larval cysts expand slowly over years or decades becoming symptomatic as they impinge on other structures by virtue of their size. Spontaneous cyst rupture happens in the minority of cases but is not rare. The cysts contain hundreds of viable scoleces capable of becoming adult tapeworms upon ingestion by a definitive host such as the dog. The internal germinal membrane lining the cyst produces new scoleces on an ongoing basis. Each scolex is capable of becoming a new daughter cyst either within the original cyst or elsewhere should the original cyst rupture or be ruptured. Hydatid disease is common in sheep-raising areas worldwide. Most primary infections involve a single cyst. 65% of solitary cysts are found in liver, 25% in lung and the rest in a wide variety of other organs including kidney, spleen, heart, bone and brain. In patients with a pulmonary cyst, approximately 15% will also have a hepatic cyst. Splenic cysts are uncommon, occurring in about 2-5% of all hydatid cases seen at referral centers. Most series do not specifically report on rates of isolated splenic cysts compared to multi-organ presentations. Rates of splenic involvement in asymptomatic patients are unknown. Serology is usually positive with hepatic cysts but sensitivity drops below 50% with solitary pulmonary cysts even when the cyst is large. With the large burden of disease in this patient a positive serology would be expected. Praziquantel is the most potent scolicidal drug and is the drug of choice for all adult tapeworms. However, praziquantel cannot penetrate the hydatid cyst wall so is only useful as an acute therapy when a cyst ruptures (spontaneously or due to surgical mishap) and scoleces are lying free before encysting again. Albendazole is the therapy of choice for intact cysts that are not operable, such as when there are multiple or disseminated cysts. A trial of Albendazole may also be considered for solitary cysts that are less than about 10 cm. Response is generally slow and only complete in a minority of cases. Surgical resection is the therapy of choice for large intact solitary cysts and certainly in a case like this with a large burden of disease. The patient could not afford surgery at the time of initial presentation and elected a trial of albendazole 400 mg bid and which was only taken irregularly. She was readmitted 5 months after the initial presentation for an episode of abdominal pain. No further imaging was performed and at laparotomy a cholecystectomy was performed. Contrast was inserted into the stent and no compression or obstruction was noted and there was no extra biliary leakage. Only one very small cyst was noted in the left lobe of the liver and only fibrotic tissue was present in the area where a cyst had been compressing the main duct 5 months earlier. Each of the seven splenic cysts visualized at surgery was aspirated, instilled with hypertonic saline for 30 minutes to kill the scoleces inside, and re-aspirated followed by resection of each cyst. Image E shows a resected cyst lined by the inner or germinal membrane that is responsible for the ongoing generation of new protoscoleces as the cyst grows in size. Image F shows a section of a typical scolex from inside the cyst. Because of the strong possibility that the initial cyst compressing the bile duct had ruptured in the interim, the patient remains on oral albendazole and is doing well.
|