2009 Case #4 |
 |
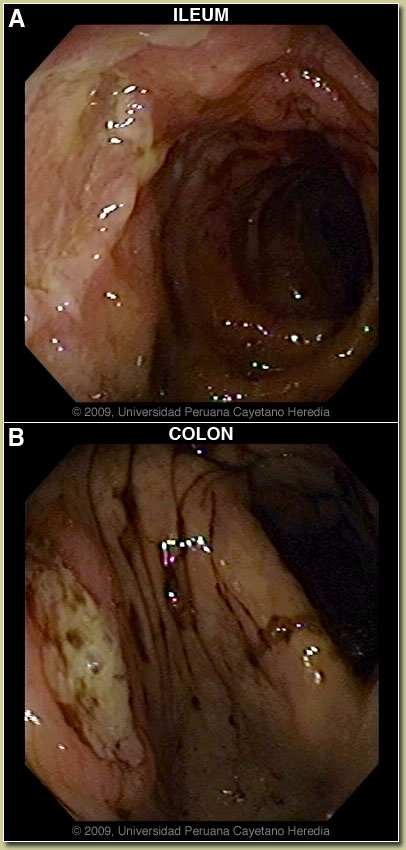
| Diagnosis: Typhoid fever complicated by gastrointestinal bleeding and intestinal ulceration. |
| Discussion: The blood cultures from the outside hospital grew Salmonella enterica, var typhi, fully susceptible to quinolones, chloramphenicol, TMP/SMX. A Widal agglutination test for salmonella at the initial presentation at Day 4 had disclosed a low titer for the somatic antigen (O 1/40); considered negative. Another Widal test on Day 12 on the outside disclosed the O antigen to be 1/160 (considered positive), H antigen 1/80, S. paratypi A 1/80, paratyphi B negative. However, the Widal repeated by us on admission showed O 1/40, H 1/80. The histology of the ulcers disclosed a dense inflammatory infiltrate composed of lymphocytes and plasma cells, mainly in the mucosa and scanty in the submucosa, with histiocyte accumulation both in the terminal ileum and colon. There were no granulomas, no parasites and no evidence of cancer. Ziehl-Neelsen stain was negative. See Gorgas Case 2008-07 for images of typical “typhoid cells” that are sometimes found in these cases.
The Widal test remains controversial because of highly variable sensitivity, specificity and predictive values in different settings. The negative Widal test in this patient with 3 weeks of illness reinforces this point. Peripheral blood cultures are positive in 40-80% of patients, only reaching higher yields if 15 ml of blood are cultured because of the extremely low numbers of organisms in peripheral blood, with 80% of those being intracellular. Culture of bone marrow increases the yield to >95% and may remain positive even in the face of several days of antibiotic therapy. Blood culture yield decreases after the first week of illness. Stool cultures are positive in 30% of cases of acute typhoid fever. Typhoid fever is a systemic febrile illness caused by Salmonella enterica sub-species enterica serotype Typhi. Prolonged fever, sustained bacteremia, and intracellular multiplication of the bacteria within mononuclear phagocytic cells of the liver spleen, lymph nodes, and Peyer’s patches are hallmarks of the infection. Paratyphoid fever is a pathologically similar but milder disease caused by a number of other serotypes of Salmonella. Transmission is usually via contaminated food and water. S. typhi can survive for weeks in water, ice, sewage and on inanimate objects. Stool from chronic carriers can contain from 106 to 109 organisms. Ingested bacteria invade small intestinal epithelial cell and are initially internalized in intestinal lymphoid cells and draining mesenteric lymph nodes. At the end of an incubation period, which is generally 7-14 days but can vary from 3-60 days, clinical disease heralds the onset of the bacteremic phase of the infection. Bacteria may invade any organ but most commonly invade mononuclear cells within liver, spleen, bone marrow, gallbladder and Peyer’s patches. Involved Peyer’s patches are generally in the terminal ileum within 60 cm of the ileo-cecal junction and in the cecum itself. Without treatment, after about 7-10 days of illness, necrosis and sloughing of the overlying mucosa may result with ulcer formation and more rarely intestinal perforation. Ulcers are usually 1 cm or less in size often multiple. Lesions are never seen in the left side of the colon [Dig Liver Dis. 2004 Feb;36(2):141-6]. Most patients are children and young adults under 25. Clinical manifestations are protean and non-specific but almost always include fever and headache. The headache often results in insomnia. Fever is initially low-grade but by the second week is high (39 to 40°C) and sustained. There may be intermittent confusion and many patients have an apathetic affect. Complications occur in 10-15% and are more frequent in patients who have been ill for 2 weeks or more. While a large number of complications have been described, clinically obvious gastrointestinal bleeding (10% of all patients), intestinal perforation (1-3% of hospitalized patients), and encephalopathy are the most common. GI bleeding is serious in 2% of all cases. Based on the colonoscopic findings other, but less likely, diagnoses in this case would be intestinal tuberculosis or Yersinia infection. Entameba histolytica and Balantidium coli infection cause ulcers and perforation but would only be found in the colon. Drug resistance in Latin America has not occurred to the same extent as in Asia and other areas of the world. Most of the typhoid in Perú remains sensitive to ampicillin, chloramphenicol, and trimethoprim/sulfa. Nevertheless, oral quinolones for 10 days remain the treatment of choice for uncomplicated typhoid due to insignificant rates of relapse and chronic carriage, as well as faster times to fever resolution of quinolones compared to the older drugs. Quinolone resistant S. typhi, which has become highly prevalent in Asia, has not emerged in Latin America, so that empiric quinolone therapy can be initiated without reservation in those who acquire infection in Latin America. In febrile patients with most diseases, clinicians often characterize a non-response of fever after 48 hours as an antibiotic failure and switch drugs. In typhoid fever, response to quinolones most often does not occur until Day 4 or 5 and with chloramphenicol it is usually longer. This patient’s non-response to ciprofloxacin after 3 days was mis-interpreted as a failure, though it is not certain that he would have avoided the GI complications had he completed his prescribed course. The chloramphenicol he received was at too low a dose to have been effective. Effective antibiotic treatment during the first week of fever reduces the complication (bleeding, intestinal perforation) rate to essentially zero. Adequate treatment doses that are delayed until the second or third week of illness dramatically reduce the complication rate but bleeding and perforation may still occur even after the patient has become afebrile. The cholera epidemic that began in 1991 in Perú and other Latin American countries resulted in the implementation in Perú of many public health and infrastructure changes that had a dramatic bystander effect on typhoid fever incidence rates [Infect Dis Clin North Am. 1994 Mar;8(1):183-205]. Unfortunately, with the disappearance of cholera from South America, other enteric diseases seem on the increase once again and typhoid rates are increasing. In the ICU, the patient was transfused and IV ceftriaxone 1g bid plus cipro 400 mg bid were started, despite the ID Service recommendation for one or the other. Fever was normal by hospital day 3. The patient had one more episode of significant GI bleeding and then nothing further. The course of the bleeding is consistent with our experience. The bleeding usually lasts few days and it is rarely necessary to perform what would need to be radical surgical intervention as a specific bleeding point is rarely apparent. |