 |
Gorgas Case 2013-07 |
 |
|
The Gorgas Course in Clinical Tropical Medicine spent its last week with a 4-day field trip to Iquitos, Perú on the banks of the Amazon River. Iquitos, with a population of approximately 400,000, is the largest city in the world that can be reached only by air or by river. The nearest road ends over 400 km away. In addition to this week’s patient, two more cases from Iquitos will be presented in the following weeks.
The following patient was seen at the Regional Hospital of Loreto in Iquitos. 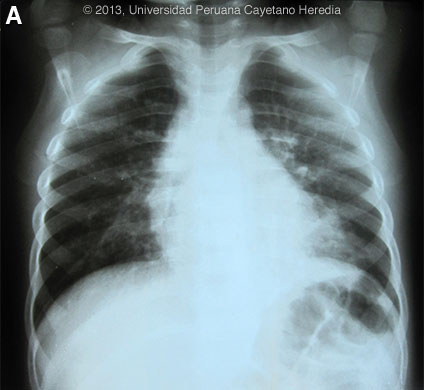  History: Previously healthy 2 year 10 month old male presents with a 2-week history of dry cough. The mother states that over the 2 weeks, the cough became paroxysmal with most of the events lasting up to a maximum of 5 minutes [see Video at right]. Between episodes the child was active with no pain. On the day of admission the child developed inspiratory stridor during the episodes of cough and developed an unquantified fever. In addition, he was less active and not playing as usual, with some diminution of oral intake. Mother denies any rhinorrhea, cyanosis or vomiting. Epidemiology: Born and raised in urbanized areas of Iquitos in the Peruvian Amazon. Lives with 4 siblings and parents all of whom are well. No known ill contacts. Does not attend a day-care center. Vaccinations completed up to 1 year of age, including hepatitis B, yellow fever, and MMR. Physical Examination (on admission): Afebrile, HR: 92, RR: 30. No acute distress. No pallor; capillary refill <2s. HEENT: Pharynx normal, no lymphadenopathy. Chest: lung fields clear. CVS: S1, S2 normal; no murmurs. Abdomen: normal bowel sounds, soft, no hepatosplenomegaly. Neurological: alert, following commands. Laboratory Results: Hb: 11.2. Hct: 34.3. WBC: 36,900 (neu: 37%, eos: 4%, mono: 1%, lymph: 58%); Platelets: 375,000. CXR is Image A.
|
|
Diagnosis: Whooping Cough due to Bordetella pertussis.
Discussion: PCR of pharyngeal secretions performed by the US NAMRU-6 in Lima was positive for Bordetella pertussis. Diagnosis is historically based on culturing B. pertussis, a small, fastidious Gram-negative coccobacillus with exclusive affinity for the mucosal layers of the human respiratory tract, from nasopharyngeal specimens obtained during the catarrhal stage and early paroxysmal stage (<2 weeks from onset). However, culture is highly specific but not very sensitive, and requires special culture media. PCR is clearly more sensitive when feasible, is useful up to 4 weeks after onset (including up to 7 days after antibiotics started) and is currently most widely used in resource rich settings. Serological diagnosis requires paired serum specimens collected one month apart, so is not useful clinically. High antibody concentrations in single sera from unvaccinated individuals suggest recent infection. During the first year following vaccination, serological testing using a single serum sample is problematic. Pertussis is a highly infectious disease with an incubation period of 9–10 days (range, 6–20 days), transmitted via the respiratory droplet route. Estimates from WHO suggest that in 2008 about 16 million cases of pertussis occurred worldwide, 95% of which were in developing countries, and that about 195,000 children died from this disease. In the early catarrhal stage, it has a secondary attack rate of up to 90% among non-immune household contacts. Untreated patients may be contagious for 3 weeks or more, although transmission diminishes rapidly after the catarrhal stage. Chronic carriers of B. pertussis are uncommon. Natural infection confers some limited immunity, especially when boosted by frequent re-exposure to B. pertussis. However, long-lasting natural immunity cannot be ensured and should not be presumed. The onset of disease is marked by non-specific catarrhal symptoms without fever. In typical cases an intermittent cough becomes paroxysmal after 1–2 weeks, typically ending with an inspiratory whoop. Whooping is characterized by the noise of the forced inspiratory effort but is not always present, especially in infants <3 months. Post-tussive emesis occurs frequently. Paroxysms can develop spontaneously or be precipitated by external stimuli. Symptoms are often worse at night, and can last from 2–6 weeks. Milder symptoms without the typical whoop may be observed in individuals who have previously been vaccinated, and older children and adolescents. In young infants, pertussis may cause apnea, bradycardia, and cyanosis without cough or whooping, whereas in adolescents and adults persistent cough may be the only manifestation. The differential diagnosis of pertussis includes RSV (respiratory syncitial virus), mycoplasma, adenoviruses and Chlamydia trachomatis. A characteristic though not constant nonspecific laboratory indication of B. pertussis infection is an absolute lymphocyte count over 10,000 lymphocytes per microlitre (21,400 in the case here). Marked leukocytosis (e.g., >60,000 cells/microlitre) has been associated with increased pertussis severity. Chest radiographs may show perihilar infiltrates and atelactasis but a consolidation should raise the suspicion of a bacterial super-infection. Pneumonia is one of the most frequent complications of pertussis with an incidence of approximately 6%, with higher rates in infants less than 6 months. Pneumonia may be a primary manifestation of B. pertussis infection or the result of secondary bacterial infection. In developing countries, the case-fatality rate for pertussis is estimated at 4% in infants aged <1 year and at 1% in children aged 1–4 years. Pertussis is a clinical diagnosis and a clinical case can be defined as an acute cough illness lasting at least 14 days accompanied by one of the following: 1) paroxysms of coughing; 2) inspiratory whoop; or 3) post-tussive vomiting. In an outbreak or following a household contact to a known case, a clinical case is defined as a cough illness for at least 14 days; presence of the typical pertussis-associated features is not required. Young infants are more likely to need hospitalization than are older children or adults and the majority under 6 months of age require hospitalization. Indications include: 1) respiratory distress; 2) evidence of pneumonia; 3) inability to feed; 4) cyanosis or apnea; 5) seizures; or 6) age <3 months. Minimum criteria for discharge include all of the following: 1) no hypoxia or bradycardia after a coughing paroxysm; 2) can feed adequately; 3) reliable care at home; 4) available outpatient follow-up. Pertussis vaccine (combined with diphtheria toxoid and tetanus toxoid) has been part of WHO’s Expanded Programme on Immunization since its inception and in 2008 about 82% of all infants worldwide received 3 doses of pertussis vaccine during the first 6 months of life. WHO recommends a 4th dose in the second year of life where possible. Perú still uses the whole cell pertussis vaccine and this child had received only the initial 3 doses despite a 4th dose being recommended according to the national program. Little data exists on the duration of protection following pertussis vaccination in developing countries. Several studies in the industrialized world show that protection wanes after 4–12 years. The child received azithromycin for 5 days for treatment of pertussis and ceftriaxone for the possibility of a non-pertussis secondary pneumonia noted clinically and on chest x-ray. Azithromycin is the sole agent of choice in infants less than 1 month and erythromycin, clarithromycin and TMP-SMX (in those >2 months) are possible options otherwise. The same azithromycin regimen is used both for treatment and prophylaxis. Treatment does not affect clinical course but stops transmission. The American Academy of Pediatrics recommends antimicrobial prophylaxis for all close contacts, such as childcare workers or household members, regardless of their immunization status. Pertussis immunization should be initiated or completed in close contacts who are not properly immunized. The utility of post-exposure antibiotic prophylaxis after 21 days of onset of cough in the index case is unclear. Children with pertussis or suspected pertussis may return to school or day care after they have completed 5 days of effective antimicrobial therapy or, if they are not treated, 21 days after the onset of symptoms. See Pediatr Rev. 2012 Sep;33(9):412-20 doi: 10.1542/pir.33-9-412 for a recent review of pertussis in children. Thanks to attending physician Dr. Camilo Ruiz, Pediatric Intensivist at the Regional Hospital of Loreto in Iquitos, and to Dr. Nicolás Barrós and Dr. Myriam Perreault-Samson for collation and comments on the case presentation.
|