 |
Gorgas Case 2015-07 |
 |
|
The following patient was seen in the inpatient department of the 36-bed Tropical Disease Unit at Cayetano Heredia National Hospital in Lima, Perú.
 History: 66-year-old male presents with fever and arthritis, with onset 10 days into a jungle trip to Yurimaguas and other cities along the Marañon and Huallaga rivers (Amazon tributaries). 7 days prior to admission he developed fever, headache, muscle pain, and malaise. The fever persisted and 5 days prior to admission there was onset of a diffuse erythematous rash and diffuse polyarthralgia involving the hands, wrists and heels. The fever disappeared 3 days prior to admission, but he was unable to walk due to the severity of the arthralgia. No previous medical history.
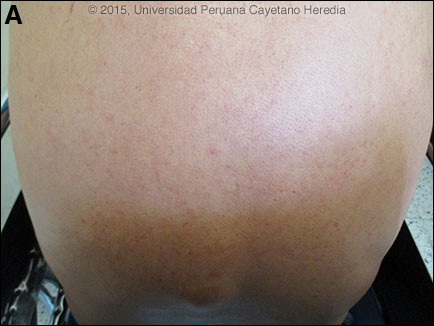
Epidemiology: Born in and lives in Lima. Retired policeman who now works as a commercial photographer and frequently visits the jungle. Sexually active, monogamous, with no history of STIs. No known TB exposures. Vaccinated against yellow fever. Physical Examination: T 36.5°C, R 18, HR 83, BP 130/69. Restricted to wheelchair on presentation. No icterus, petechiae, or mucosal lesions. Chest clear. No hepatosplenomegaly. Mild erythematous rash on trunk and lower limbs [Image A]. Severely painful arthritis in both wrists, metacarpophalangeal joints, proximal and distal interphalangeal joints, knees, wrists, and foot, with no evidence of effusion; no inflammatory signs. Bilateral patellar enthesitis (pain at the junction of the tendons with bones) and Achilles tendonitis. He had marked limited motion throughout hands, wrists, knees, and ankles [see Video]. The enthesitis precluded mobility from the chair to a standing position. Laboratory Examination: Hct. 44%. WBC 3450 (58 N, 0 Eos, 12 Mo, 30 L). Platelets 158000. ALT/AST 30/28 (59/72 IU/L). LDH 220 (125-500 IU/L). Creatinine normal. ELISA for HIV and HTLV1 negative. Serologies for Hepatitis A, B, and C negative. IgM ELISA for leptospirosis negative.
|
|
Diagnosis: Mayaro Fever with polyarthritis.
Discussion: PCR and IgM ELISA for dengue and chikungunya were negative. IgG and IgM ELISA for spotted fever and typhus group rickettsia were also negative. IgM ELISA for Mayaro virus was positive. Mayaro virus (MAYV) is an arthritogenic alphavirus first described in 1954 in Trinidad and now thought to be enzootic in a wide area of the forest canopy of northern South America, including Colombia, French Guiana, Suriname, Venezuela, Perú, Bolivia, and Brazil. Recent serosurveys indicate spread to Panama, Costa Rica and Guatemala. Transmission is primarily via canopy dwelling Haemagogus sp. mosquitoes, resulting in what is though to be limited human transmission and infrequent case clusters [Emerg Infect Dis. 2013 Nov;19(11):1839-42, Clin Infect Dis. 1999;28(1):67-73]. Experimental data indicates receptivity of Aedes sp. mosquitoes, so a potential for urbanization does exist. Several cases have been reported in tourists returning from the Amazon region, highlighting the need to consider MAYV in febrile returned travelers, especially as the related arthritogenic alphavirus chikungunya (CHIKV) becomes established in overlapping areas. Although long-term manifestations of infection with other alphaviruses such as CHIKV have been more robustly characterized [Nat Rev Rheumatol. 2012; 8:420], a report of a case cluster from the same area of Peru as visited by our patient included a prospective 1-year longitudinal study that found long-term arthralgia in more than half. This is similar to reports of other arthritogenic alphaviruses including Ross River and Barmah Forest viruses from Australia, as well as Sindbis (worldwide) and O’nyong-nyong (Africa) viruses. Previous studies have in general identified persistent symptoms in the fingers, joints of the wrist, ankle, and knee. Hip or axial pain is rare. The sequelae are generally thought not to be autoimmune in nature but are rather due to residual viral infection of macrophages and other immune cells in the joints. Acute MAYV has an incubation period of approximately 3 to 12 days and presents with fever (100%), rash of 3 to 5 days duration beginning on day 4 or 5 of illness (30-50%), myalgia (75%), retro-orbital pain (63%), as well as arthralgia or arthritis (50-90%). Patients are viremic for 5 to 7 days. Acutely, the most affected joints are hands, knees, wrists, ankles or foot, elbows, shoulders, and hips. Early on MAYV may be clinically indistinguishable from dengue, yellow fever, chikungunya, or Oropouche virus. Serologic diagnosis is available only in specialized centers where PCR may also be available. Our patient’s residual rash disappeared on the third hospital day. As no anti-viral agents effective against alphaviruses exist, he was treated with naproxen with significant improvement of the joint pain, and he was discharged after 7 days with residual difficulty in walking. Acknowledgement: We would like to thank Gorgas Course attending infectious diseases specialist Dr. Fernando Mejia for his contributions and ongoing discussions of this case.
|