About
UAB's Global Emergency Medicine Fellowship is a SAEM-accredited, clinically oriented program established in 2012 who has continuously trained fellows to make an impact in resource limited settings.
“Up to 50 percent of the excessive mortality burden borne by low- and middle-income countries might be eradicated by the development of effective emergency care.” – World Health Organization
We envision a world where emergency medical expertise is common, specific to the needs of local patients, and evidence-based.
Objectives
- Gain knowledge and expertise in the diagnosis and management of diseases specific to tropical and resource limited emergency settings.
- Gain a broader understanding of humanitarian response, collaboration with non-government organizations, and the delivery of emergency care within the framework of SPHERE principles.
- Innovate in the education of clinicians at home and abroad in the delivery of resource limited emergency care.
- Facility to navigate the ethical issues peculiar to resource-limited medicine.
- Learn to travel wisely, including food and water safety, navigation of customs, collaboration with local medical systems.
Curriculum
The Global Emergency Medicine fellowship can take place over one or two years. Those who choose to complete the fellowship in one year will earn a Global Health Certificate through the UAB School of Public Health. Those who choose to complete a two-year fellowship will earn a master's degree in global health or equivalent.

Curriculum Outlined
Education:
- Internal lecture series (July – December)
- Diploma of Tropical Medicine and Hygiene (Gorgas or equivalent course)
- Humanitarian Response Intensive Course (Harvard Course or equivalent)
- Graduate Certificate in Global Health (15 graduate credit hours through UAB School of Public Health)
- Joint Grand rounds with University of Kentucky
Professional Development:
- Direct mentoring
- National leadership opportunities through ACEP
- Regional/national speaking opportunities
- Hospital committee engagement (SIDT, employee health, etc)
- Adjunct course instructor (MS4 course, ultrasound training for hospitalists, etc)
- Attending a national EM conference
- School of Medicine engagement
- Bedside supervision / teaching of medical students / residents / APPs
- Mentored research project
- Formal UAB research training course
Field Work:
- 1 month clinical trip (Historically Tenwek Hospital, Kenya)
- 1 – 2 short field assignments
- Trip preparation, logistics planning, personnel recruitment, wise travel preparation, collaboration with local medical systems
- Trip preparation, logistics planning, personnel recruitment, wise travel preparation, collaboration with local medical systems
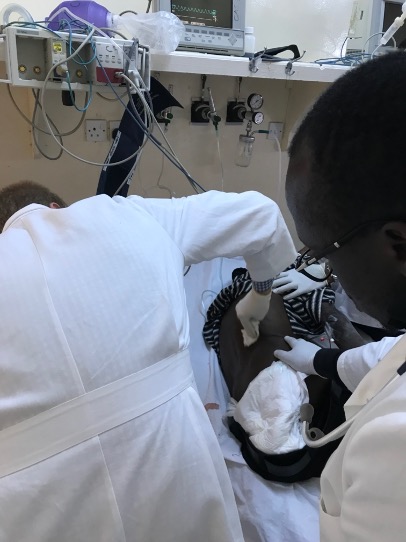

Left: Field work being completed in Kenya. Right: Gorgas Diploma course in Tropical Medicine and Hygiene (DTM&H) small group.


Left: Harvard humanitarian course simulation. Right: Fellows and faculty members teaching at the American College of Emergency Physicians (ACEP) meeting.
Combined fellowship opportunities
Fellows may choose to complete combined fellowships in Global Emergency Medicine and Point-of-Care Ultrasound in Resource-Limited Settings (PURLS) or Social Emergency Medicine/Population Health. Choosing to complete a combined fellowship will require a total of two years of study. Those who choose to combine the Global Emergency Medicine and Social Emergency Medicine/Population Health fellowships will complete an MPH degree as part of their studies.
Application
To apply, submit a curriculum vitae (CV), two letters of recommendation, and a letter of interest to the Program Director and Education Coordinator. This competitive fellowship participates in and follows the NRMP fellowship match schedule.
Key Faculty
Burleson, Samuel (Luke), M.D.
Program Director, Point-of-care Ultrasound in Resource-Limited Settings Fellowship
Greene, Christopher J., M.D., MPH
Director of the Office of Global Health and International Emergency Medicine
Assistant Physician Director of Quality and Patient Safety
Heimann, Matthew, M.D.
Associate Director, Mary Heersink Institute of Global Health
Contact

Matthew Heimann, M.D.
Program Director
mheimann@uabmc.edu

Ashlyn Gordon
Education Coordinator
ashlyngordon@uabmc.edu





