 |
Gorgas Case 2017-02 |
 |
|
The following patient was seen in the outpatient department of the Tropical Medical Institute:
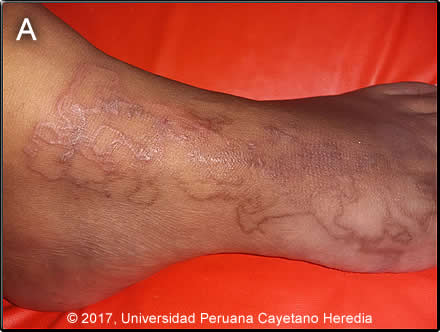
 History: A previously healthy 42-year-old female presented with a 3-month history of progressive painful and pruritic cutaneous lesions on the dorsum of the left foot. She initially noticed a painful and slightly pruritic papular lesion over the first metacarpo-phalangeal joint. During the following week, the lesion extended on the plantar surface of the foot towards the sole in a linear path that later blistered and increased to a size of 3 x 4 cm. She was treated with cephalexin and dexamethasone for a few days without improvement. One month into the illness the now markedly pruritic lesion began to migrate in the same linear path to the dorsum of the foot. No fever or systemic symptoms, no swelling in the groin.
Epidemiology: Lifelong resident of Lima. One week before the onset of symptoms she had returned from 11 days beach vacation in Cartagena de Indias, Colombia. She walked barefoot on different islands, beaches and swimming pools. She has 2 dogs at home. Physical Examination: Afebrile. Chest clear. No lymphadenopathy or hepatosplenomegaly. Skin findings restricted to the linear serpiginous tracks on the left foot shown in Image A. Laboratory Examination (on admission): WBC 7000 (57% segmented neutrophils, 2% eosinophils, 0.4% basophils, 6.4% monocytes, 34% lymphocytes). Hb 13.0 g/dL.
UPCH Case Editors: Carlos Seas, Clinical Course Coordinator/Sofia Zavala, Associate Coordinator UAB Case Editor: David O. Freedman, Course Director Emeritus |
|
Diagnosis: Cutaneous Larva Migrans due to Ancylostoma braziliense.
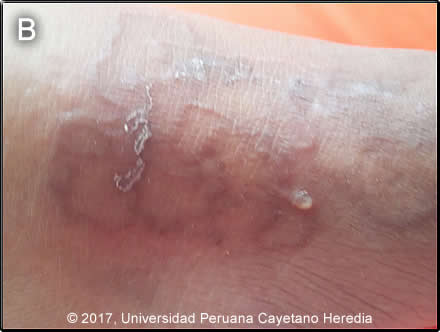
 Discussion: This is a clinical diagnosis with pathognomonic clinical findings as demonstrated in the Images [see review Lancet Infect Dis 2008; 8: 302–09–09]. Hookworm-related cutaneous larva migrans, is the term that describes the characteristic migratory dermatitis caused by initial invasion of the skin by the larva of animal or human nematodes. The larvae of the dog and cat hookworm Ancylostoma braziliense account for almost all of the clinically obvious skin lesions. Other hookworms infecting animals can invade and parasitize humans or can penetrate the human skin (causing hookworm-related cutaneous larva migrans), but do not develop any further (Ancylostoma caninum, Uncinaria stenocephala). Occasionally A. caninum larvae may migrate to the human intestine, causing eosinophilic enteritis. Because Ancylostoma braziliense does not mature or complete its life cycle in humans, the immature larvae may wander superficially for up to several months before their spontaneous death. The larvae move up to 1-2 cm per day. Biopsy of the lesions is not recommended, as the larvae are rarely isolated. Usually the larvae have migrated ahead of any inflammatory response and it is difficult to know in what direction the larva has advanced. Cutaneous larva migrans is found in any moist warm climate and is found in the southeastern USA as well as throughout the tropics. In travelers, the highest prevalence is in those returning from Caribbean destinations, followed by southeast Asia, and Central America. Larvae of human hookworm (Ancylostoma duodenale and Necator americanus) may cause an initial pruritic lesion but rarely migrate in the skin before traveling to the lung and then the intestine as they mature and complete their life cycle. In travelers the incubation period may last a month or even longer. Larvae usually migrate in the epidermis for 2–8 weeks to several months. Lesions are most common on the feet, buttocks, and thighs reflecting areas exposed to soil and sand in typical beach resort travelers. Other causes of the clinical syndrome of creeping eruption include gnathostomiasis [see example in Gorgas Case 2003-01], which tends to cause more hemorrhagic and less distinct linear tracks, and strongyloidiasis, which causes a variant usually called larva currens. Larva currens occurs due to autoinfection whereby filariform larvae of Strongyloides stercoralis passed in the stool invade perianal skin and re-infect the same host. The lesions are usually in the perianal, buttock, or abdominal region only. The lesions are highly pruritic but have a predominant urticarial component and progress up to several cm per day. They may be present for several weeks. The subcutaneous filarial infection with Loa loa seen in west and central Africa causes a migratory and transient angioedema, predominantly around joints. Linear lesions are not found. Rare cases of cutaneous pili migrans have been found in travelers. Treatment is with ivermectin 12 mg PO, which can be repeated once a day later, or with albendazole 400 mg PO for 3 days. Some cases present with folliculitis which requires more aggressive prolonged therapy [J Travel Med 2015; 22: 221–224]. Most clinicians prefer ivermectin [Clin Infect Dis. 2013 Oct;57(8):1155-7-7]. Thiabendazole topical therapy still mentioned in many textbooks is no longer used (and rarely available) and cryotherapy still used by some dermatologists is much less effective. Because of the fecal origin of the larvae, bacterial superinfection can result but antibiotics are generally only recommended if purulent infection is clinically present. In our patient, treatment was started with Albendazole 200mg bid. However, on follow up 3 days later she reported a new tract with a vesicle and the treatment was changed to ivermectin. |