 |
Gorgas Case 2017-09 |
 |
|
The following patient was seen in the outpatient clinic of the Tropical Medicine Institute in Lima, Perú.
History: 44-year old male presented to the outpatient clinic with palpitations and dizziness. An arrhythmia had been diagnosed 5 years earlier but he reported being completely asymptomatic until the past month. He has noted daily palpitations and two episodes of dyspnea on exertion associated with dizziness that resolves with rest. He denies fevers, chest pain, syncope, and dyspnea at rest, orthopnea, nocturnal paroxysmal dyspnea or lower extremity edema. No gastrointestinal complaints. No history of hypertension or diabetes. No antecedent flu-like illnesses. He underwent surgery for kidney stones 10 years ago.
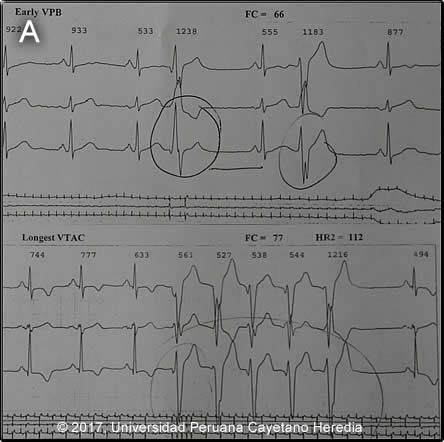
Epidemiology:Born and lived in Cajamarca and in the highlands and high jungle until age 26 with 2 years of military service during that time. Subsequently, he travelled all over the country as an outdoor antenna installer which required him to sleep on the ground whenever working in the countryside. Currently living in Lima in a rented room with electricity but no running water or sewage. No known TB contacts, no sexual risk behavior Physical Examination: HR 70x’ irregular, RR 18x’, BP 110/80, afebrile. Chest: Clear to auscultation bilaterally, no crackles. Heart: irregular rhythm, II/VI systolic mitral regurgitation. No jugular venous distension. Abdomen: normal bowel sounds, soft, non-tender, non-distended. No hepatomegaly. Neurologic: Awake, alert and oriented in time, space and person. No focal deficits, no meningeal signs. Extremities: no lower extremity edema. Laboratory: WBC 7.16 (0, 47.6, 15.2, 1, 7.1, 29.1), Hct 44%, Hb 14.5 g/dL, platelets 253 000. Urea 38 mg/dL, creatinine 0.9 mg/dL, AST 22 U/L, ALT 52 U/L. Stools: Strongyloides stercoralis 1+ Rhythm strips from a 24-hour holter monitor (Image A) and a transthoracic echocardiogram (ImageB) are shown.
UPCH Case Editors: Carlos Seas, Clinical Course Coordinator / Sofia Zavala, Associate Coordinator UAB Case Editor: David O. Freedman, Course Director Emeritus / German Henostroza, Course Director |
|
Diagnosis: Chagas cardiomyopathy

 Discussion: Two independent confirmatory antibody tests (ELISA and IFA) were positive for T. cruzi infection. On further questioning the patient recalled having been rejected for blood donation in 2014 due to a positive serology for Chagas; no further counseling was done and a cardiac evaluation was not performed. He does not recall having had contact with triatomine bugs and denied having Romaña’s sign at any time. However, his father states the presence of triatomines in the town where the patient grew up which is in a known endemic area. His EKG and echocardiographic findings are non-specific and indicative of cardiomyopathy in general. Report of the Holter monitor: basal sinus rhythm, minimum HR 49x’, maximum HR 152x’. 13% of beats were ventricular, <1% supraventricular. Ventricular premature beats and non-sustained ventricular tachycardia (Image A). Report of the transthoracic echocardiography: Moderate mitral insufficiency due to mitral ring dilation after left ventricular dilation (Image B). Left ventricular and auricular dilation with global hypokinesis of the left ventricle, no apical aneurysm. Moderate dilated cardiomyopathy with mild systolic dysfunction, ejection fraction 48%. T. cruzi is a single-celled protozoan found in two forms in infected humans. The infective trypomastigotes are found in the acute phase of disease circulating in the bloodstream. After the trypomastigotes infect muscle, nerve and other cells, they transform into small 3-micron intracellular amastigotes as the infection enters the chronic phase. Amastigotes replicate slowly by binary fission and are released after host cell rupture to infect other host cells. Initial human infection occurs when the vector, large triatomine bugs (5-45 mm in length, see Image C (take from previous case), take a blood meal at the end of which they defecate on the victim. The victim then self-inoculates with trypomastigotes present in the feces by rubbing on the irritated spot and the parasites enter by any small break in skin integrity or often through intact mucosal tissues such as the conjunctivae. In the acute stage of infection, the clinical manifestations can vary widely. Most infections are asymptomatic, up to 20% have a mild undifferentiated febrile syndrome, and less than 5% have a severe or fatal illness that is usually associated with myocarditis, heart failure or meningoencephalitis. An inoculation chancre or chagoma is seen in about half of cases, and when the entry is via the conjunctiva, unilateral bipalpebral orbital edema (Romaña’s sign) is seen. Non-specific EKG changes are common, with evidence of myocarditis in more severe cases. The severe conduction abnormalities seen in chronic disease are uncommon in acute disease. Patients in the chronic phase of disease have progressive infection of myocardial and autonomic nervous tissue and present with cardiomyopathy, cardiac conduction abnormalities and gastrointestinal disease, including megaesophagus and mega-colon. The alarmingly poor survival curves in individuals who manifest clinical cardiac disease have now been clearly elucidated [N Engl J Med. 2006 Aug 24;355(8):799-808]. Major risk factors for mortality in these patients are clinical heart failure, evidence of left ventricular dilatation or systolic dysfunction, and non-sustained ventricular tachycardia. This patient has a Rassi score >12, indicating a 10-year mortality of 85%. Unlike the acute phase, where parasites are present in circulating blood, diagnosis of chronic cases can be difficult and usually depends on serology or, optimally where available, PCR of blood. Chronic Chagas’ heart disease usually presents initially with biventricular heart failure and then other complications later during disease progression. Frequent presenting symptoms are dyspnea on exertion, fatigue, palpitations, dizziness, syncope and edema due to heart failure, cardiac arrhythmias, and thromboembolism. Chest pain frequently occurs. Typical physical findings include murmurs of tricuspid/mitral regurgitation, split S2 (bundle branch block) and a diffuse apical thrust (apical aneurysm). Manifestations of right-sided heart failure often predominate. Any type of arrhythmia may occur, including sinus node dysfunction, intermittent complete atrioventricular block (RBBB most common) and complex ventricular arrhythmias. Ventricular arrhythmias and AV block frequently occur together. In advanced disease low QRS voltage is common. Atypical chest pain is common with or without heart failure but may mimic angina. Chagas’ heart disease requires presence of parasites in myocardial tissue and reflects an aberrant immune response. Endomyocardial biopsy is rarely necessary for diagnosis. Human Chagas’ disease is found in all countries of the Americas from the southern USA to Argentina and Chile. The majority of the 10 million infected individuals are found in Brazil, though Bolivia has the highest seroprevalence rates. There are more than a hundred species of triatomine bugs in the Americas but most human disease is due to Triatoma infestans, Rhodnius prolixus, and Panstrongylus species. The vectors generally live in thatched roofs and cracks in the walls of poorly constructed homes in impoverished rural areas. More than 100 mammal species can act as reservoirs including dogs, cats and guinea pigs. In Perú, Chagas’ disease has been described with highest risk in the south, but reports of the disease in the Amazon jungle and highland areas of the north and centre of the country have occurred (General Office of Epidemiology, Peru, Report 2016) Both benznidazole, usually considered the drug of choice and the alternative drug nifurtimox are generally poorly tolerated. However, alternative dosing strategies to conventional regimens have been proposed and are being refined [N Engl J Med. 2015 Nov 5;373(19):1882. doi: 10.1056/NEJMc1510996]. Peruvian guidelines mandate treatment of all patients regardless of symptoms. Our patient received Nifurtimox with only gastrointestinal side-effects, due to limited supply of benznidazole which occurs in many endemic countries. Anti-arrythmic drug therapy is being managed by a cardiologist. |