 |
Gorgas Case 2017-11 |
 |
|
This is our last Case of the Week for 2017. We hope you have enjoyed the 2017 series of live cases each week from Peru. The Gorgas Diploma Course, in February and March, and the Gorgas Advanced course, in August, are held annually and we will be in touch at the beginning of next year’s case series.
Publishing these case reports would not be possible without the assistance of an extremely dedicated group of people. We would like to thank in particular UPCH Case Editors: Dr. Carlos Seas, Clinical Course Coordinator and Dr. Sofia Zavala and Dr Karen Luhmann, Associate Coordinators and UAB Case Editor: David O. Freedman, Course Director Emeritus, for case selection and coordination of case summaries and images, and Alfredo Guzman of the Gorgas Center for Geographic Medicine at the UAB Division of Infectious Diseases for all publishing on the Gorgas Course website. The following patient was seen by Gorgas Advanced Course participants on the surgical ward of the Hospital Cayetano Heredia in Lima-Peru. Eduardo Gotuzzo & German Henostroza Course Directors 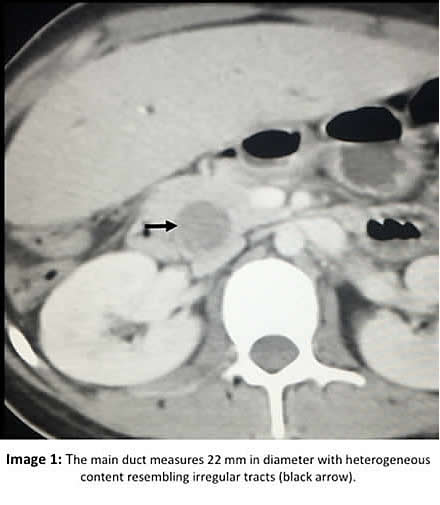 History: A 17-year-old woman, previously healthy, presented to the ER with fever, jaundice, and shock. 12 days before admission the patient developed cramping right upper quadrant and mid-abdominal pain, anorexia and nausea, with onset three days later of jaundice and dark urine. She has no previous episodes of abdominal pain or jaundice. Over the subsequent days the abdominal pain increased until three days before admission when the onset of fever was accompanied by new radiation of the pain to the back. In the ER she was found hypotensive, unresponsive to fluids and transferred to the Trauma Shock Unit for more fluids, vasopressors and broad spectrum antibiotics.
Epidemiology: Patient was born and lives in Lima. Her only travel was a single trip to Huaraz, state of Ancash in the Peruvian Andes, years ago. Has contact with dogs and cats. Denies living near a slaughterhouse. No known TB exposure. No ingestion of aquatic plants. No weight loss, no IV drug use, no alcoholism, or new sexual partners. Physical Examination: BP 82/36, HR: 124, RR: 24, Temperature 38C, Sat02 96% at room air. Patient appeared acutely ill with moderate respiratory distress No edema, no cyanosis, Skin: Jaundice 3+. Abdomen: Distended, bowel sounds present, diffuse pain on deep palpation, no peritoneal signs. Enlarged liver (5 cm below right margin). No splenomegaly or lymphadenopathy. Glasgow coma scale 15. Laboratory: Hb 10.2. Hct 31. WBC 16,600 (3 band, 82 neutrophils, 1 eosinophils, 8 monos, 5 lymps). Glucose 96. Urea 22.4. Creatinine 0.3. Bilirubin 18.5 with 16.7 direct. AST 76 ALT 76, alkaline phosphatase 387 (<150 mg/dl). HIV Negative. HBsAg Negative. HAV IgM Negative. Abdominal CT (Image 1) is shown.
|
|
Diagnosis: Echinococcus granulosus with intrabiliary rupture of hepatic hydatid cyst.
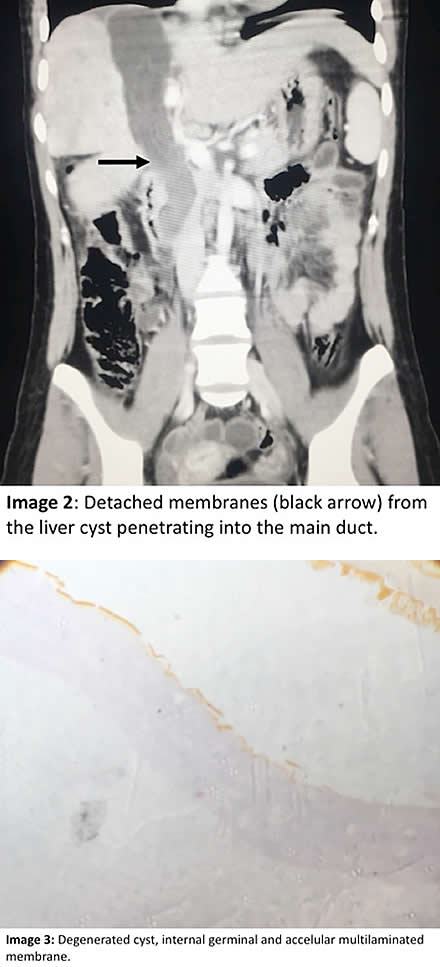
 Discussion: At surgery, the dilated main bile duct was opened and white membranes were extracted with approximately 300mL of purulent biliary secretion. The cyst in the main bile duct seemed to extend into the liver parenchyma. The abdominal CT-scan was read as showing an enlarged liver with dilatation of intrabiliary ducts and signs suggestive of cholangitis. The main duct measures 22 mm in diameter with dense heterogeneous content, resembling linear and irregular tracts (Image 1 arrow). There is a liver cyst of 11.5 cm in vertical diameter by 4.5 cm in transverse diameter; this cyst has heterogeneous content suggestive of detached membranes that are also seen in the dilated main duct, representing a communication between both (Image 2 arrow). Hydatid cyst rupture is classified into three types: a) contained rupture, when the endocyst (acellular multilaminated membrane and nucleated internal germinal membrane) ruptures but the content is confined within the pericyst (compressed host organ parenchyma), b) communicating rupture, when cyst content escapes usually into the biliary tract because the pericyst incorporates biliary branches as it expands, and c) direct rupture when both endocyst and pericyst tear and the full content splits into the pleural or abdominal cavity (AJR 1988;150:1051-3). When the cyst communicates with the biliary tract it may involve the common hepatic duct, lobar branches or small intrahepatic branches, the latter are most commonly involved. Small communications between liver cysts and the biliary tree seem to be common (40-90%) and are usually asymptomatic, but large tears are less frequent (5-10% of these) causing biliary tree obstruction and potentially serious complications such as cholangitis, hepatic abscesses, acute cholecystitis, acute pancreatitis and even biliary cirrhosis (Br J Surg 1971;58:228-32; AJR 1982;139:699-702). CT can help identifying the communication between the liver cyst and the biliary tract by showing the defect or discontinuation of the cyst or indirectly by showing linear and irregular tracts inside the biliary tract as in this case (Image 1). Multidetector CT enhances the view of the common bile duct and may be used as an adjunct diagnostic technique in cases of suspected major tears into the biliary tract (Abdom Imaging 2011;36:433-7). ERCP may be used to remove the contents of the cyst, but usually surgical exploration is needed. When a hydatid cyst becomes infected, the bacteria digest all the cyst contents and the membranes, so that in the pathology examination only the remaining hooklets can be found, the membranes and protoscolices cannot be found. In this case, the infection had not yet digested the complete membranes, that is why they were still identifiable but with degeneration (Image 3 showing internal germinal and external acellular multilamellated membrane). The remaining cyst cavity contents are probably dead, but just in case we decided to give albendazole for three months after surgery. Human hydatid disease secondary to Echinococcus granulosus is caused by the larval form of this dog tapeworm. Humans ingest the tapeworm eggs in environments contaminated by canine feces and become accidental intermediate hosts. Sheep are the normal intermediate hosts. In general, disease is diagnosed in adulthood as larval cysts expand slowly over years or decades, becoming symptomatic as they impinge on other structures by virtue of their size. The cysts contain hundreds of viable protoscolices capable of becoming adult tapeworms upon ingestion by a definitive host such as the dog. The cyst wall is composed of a 1 mm thick acellular multilaminated membrane, followed by the nucleated internal germinal membrane that is about 0.1 mm thick. The internal germinal membrane lining the cyst produces new protoscolices on an ongoing basis. Each protoscolex is capable of becoming a new daughter cyst should the original cyst rupture or be ruptured. Cystic hydatid disease due to E. granulosus is common in sheep and cattle raising areas worldwide. Most primary infections involve a single cyst. In adults, 65% of solitary cysts are found in liver, 25% in lung and the rest in a wide variety of other organs including kidney, spleen, heart, bone and brain. In patients with a pulmonary cyst, approximately 18% will also have a hepatic cyst. |