Case history
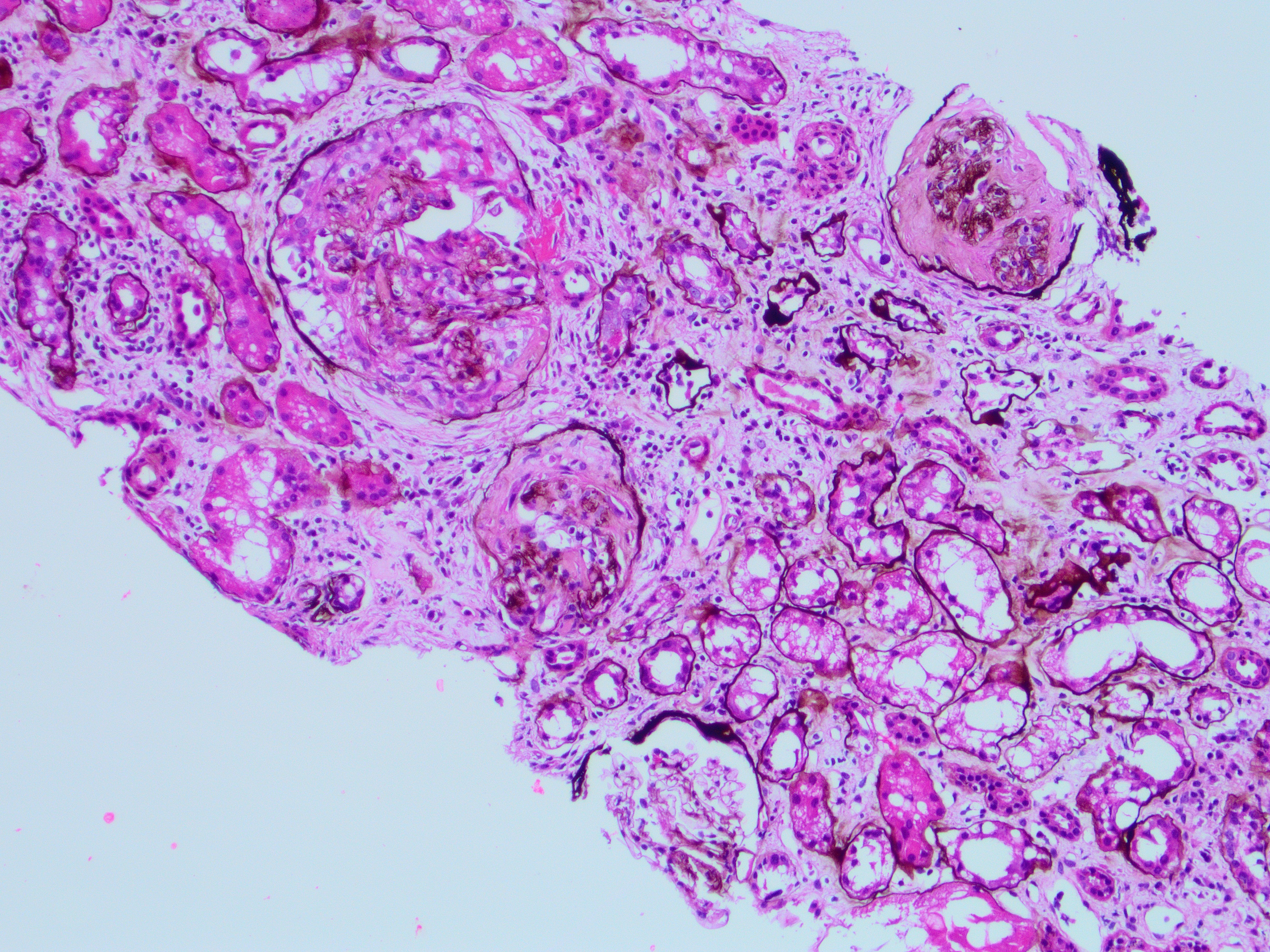
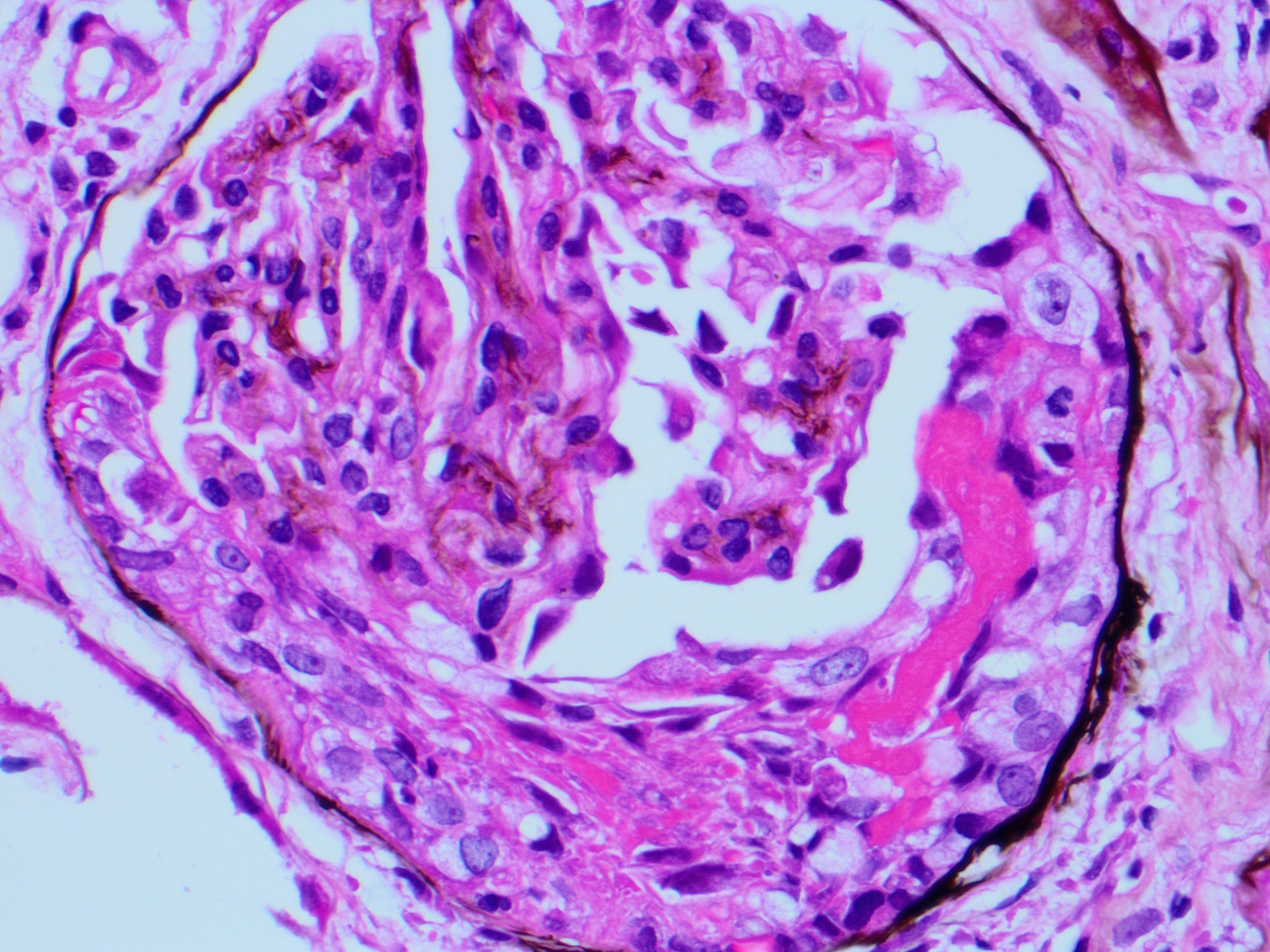
A 76-year-old man with a history of HTN and CKD Stage III presented with increased serum Cr. Renal biopsy performed showed cellular and fibro-cellular crescents with fibrinoid necrosis by LM (Jones silver, Fig a & b). IF and EM were negative.
Which of the following information, based on LM findings, is helpful in making the diagnosis?
- . Anti-dsDNA titer
- . ANCA titer
- . Anti-GBM antibodies.
- . All of the above.
Answer: “D.” All of the above
Brief explanation of the answer:
The light microscopy in this case is showing crescentic glomerulonephritis (GN). The differential diagnosis for crescentic glomerulonephritis includes; 1) immune complex mediated GN, e.g., lupus nephritis (LN), 2) ANCA associated pauci -immune GN and 3) Anti-GBM antibody mediated GN. The diagnosis relies heavily on the clinical history and IF findings. The IF will show granular staining for immune complex deposits in LN and ANA will be positive. The anti-GBM antibody GN will show sharp linear staining along the GBMs by IF and anti-GBM antibodies will be positive. The ANCA associated GN typical shows no staining by IF. This patient was positive for cANCA, MPO and anti-histones antibodies. pANCA, PR-3 and anti-dsDNA were negative. The serology and IF findings were c/w ANCA associated GN. However, anti-histones antibodies are usually associated with drug related GN. Additional history on this case revealed that the patient was on hydralazine for BP control, which has resulted in vasculitis/ GN.
ANCA associated vasculitis has been reported with propylthiouracil (most common), hydralazine, sulphasalazine, cocaine, and other drugs. The diagnosis of drug-induced vasculitis is based on the temporal relationship between clinically evident vasculitis and administration of the offending drug. Therefore, it is essential that a comprehensive drug history should be obtained in patients with vasculitis in order to make a prompt diagnosis, as treatment primarily involves drug cessation and supportive care.
Case contributed by Huma Fatima, M.D., Assistant Professor, Anatomic Pathology, UAB Department of Pathology